10 steps to efficient endo in the general practice
by Jack D. Griffin Jr., DMD, FAGD
Making endodontics less frightening for patients and dentists
Some patients are afraid of endo … so are some dentists. Neither should be. If a patient says, “That wasn’t bad at all” after treatment and the tooth is comfortable for many years, the patient is happy and the staff is rewarded. If done well, endo can be one of the most rewarding, predictable, and profitable treatments a dentist can do.
Root canal therapy has made great strides in ease, efficiency, and predictability during the last few years, with increasing levels of patient acceptance. Advances in anesthetic materials and techniques, digital radiography, apex locator accuracy when teeth aren’t perfectly dry or filling-free, rotary files that take most of the physical finger work out of the procedure, and obturation materials that are simple and effective mean there is no reason endo shouldn’t be routine in most dental offices. Certainly, it is not something to loathe.
1. Methodical diagnosis
It’s really satisfying to do great endo, and it’s a real bonus if you do it on the correct tooth! Working on the wrong tooth is no practice builder. Therefore, it is imperative to our patients’ well-being, our practice reputations, and the practitioners’ peace of mind that we diagnose accurately and have confidence in our decisions.
Often the diseased tooth is obvious, but other times our evaluation must involve a series of tests that are challenged and scrutinized by our own skepticism. Endodontic teacher Dr. Steven Buchanan calls the search for the correct tooth “Methodical Skepticism.” It means being sure about something that is not easily seen. One must have a system of repeatable diagnostic tests that allows checking of all teeth in a suspect quadrant, and then be diligently thorough.
The patient interview and historyis the place to start. We repeat the same questions on every patient: “What makes it hurt?” “How long have you had the pain?” “Is it sharp or throbbing pain?” “Does it hurt or feel better to hot or cold?” “Do you feel pain radiating to other places?” These start the evaluation to help differentiate between pulp pathology, periodontal issues, tooth fractures, or restoration failure.
Quality digital X-rays cannot be overstated. Periapical radiolucencies and opacities are still the best indicators of a diseased tooth. Poor X-ray developing, improper angles, and faulty exposure settings all contribute to incomplete and unreliable diagnosis. Digital X-rays can help remove these errors, can be manipulated in the software to increase their diagnostic contribution, and the images have almost zero wait time. Perhaps the greatest advantage of all is that the digital image is usually seen on a 15 by 20 inch monitor instead of a 2 by 3 inch film on a view box (Fig. 1). It is certainly easier to diagnose from an image that is seven times larger with sharp detail.
Cold testing with lingering pain is one of the classic signs of irreversible pulpitis. The use of a freezing spray on a cotton swab can be less messy, more precise, and less uncomfortable for the patient than dripping ice. For about $7, a can of Radio Shack component cooler can be sprayed on a cotton tip, touched on the buccal of a tooth, and patient reaction can be monitored. Once the patient feels cold on the tooth, the swab can be removed, and since no cold water lingers in the area, the sensation should quickly disappear. Lingering or intense pain can often identify the culprit.
Tooth loading is a great way to determine if biting sensitivity is from a fracture. Since people are keeping teeth longer than ever, fractures are a growing problem. Patients who complain of pain upon biting with no other symptoms can have their problem cusps identified by loading each tooth in the quadrant with a ToothSlooth II and reproducing the pain. For patients who have symptoms consistent with irreversible pulpitis, loading the central fossa of each tooth can reveal the ones with periapical inflammation.
Of course, there are many other tests that can be done, such as percussion, heat, and vitality. Find the testing methods that are most reliable for you and stick with them on every case to develop a comfort level.
2. Gentle treatment presentation
“No offense, Doc, but I hate dentists!” is often heard in our office, to which we respond, “It’s OK, we don’t like patients.” It kind of makes things even. The second most popular phrase we hear is, “I don’t want a root canal, they hurt!” Just telling patients, “Trust me, I’m a doctor!” doesn’t always work; it’s about being confident that we can fix the problem and explain it in a way that is informational but not scary.
We should be careful how we describe things so we don’t stir up unnecessary fear. This isn’t deception, it’s using words and phrases that reduce patient stress. Usually, “root canal” to the patient means pain - real or imagined - multiple appointments, and even torture. Just as we don’t ask the assistant for “the needle” when doing an injection, we also want to avoid words that conjure up fearful images about endo. Careful wording can increase a patient’s acceptance and ease apprehension.
When we suspect endo is needed, we describe the procedure like this: “We will remove decay and the diseased part of the tooth, clean out infected debris, disinfect the inside, and then fill it with a sterile filling material.” We call it tooth disinfection, nerve work, or endodontic therapy, but never a “root canal” unless the patient asks, “Isn’t that like a root canal?”
3. Efficient, organized setup
The materials used in endo are seldom used for anything else, and lend themselves well to being “packaged” together in a single basket or drawer for easy retrieval (Fig. 2). This makes it very efficient to have everything ready when the “surprise endo” happens. The files, measuring device, apex locator, irrigant, paper points, sealer, and obturation materials are all kept in a small, inexpensive basket that is quickly pulled out and unloaded in seconds for endo at any time.
Endo baskets can be kept in each treatment room close to the assistant’s position, or in a central location that is quickly accessed. Often the assistant can have all instruments ready in about the same time it takes the doctor to explain the treatment to the patient. This concentration of endo paraphernalia makes the setup much faster and relieves your staff of considerable stress.
4. Effective numbing
After correct tooth diagnosis, the lack of profound anesthesia may be the greatest cause of staff and patient stress in endo. As we drill toward the pulp, will the patient squirm, scream, jump, or run out the door? Pain control is critical for patient comfort, staff peace, and practice enhancement. Anesthetic choice and delivery method are crucial.
A systematic approach to local anesthesia is important to achieve consistent, profound pulpal numbing: 30 seconds of topical anesthetic followed by a half carpule of prilocaine (Citanest) to achieve initial soft tissue anesthesia, followed by one to two carpules of articaine (Septocaine) to provide great deadening in almost all cases. For maxillary teeth, anesthesia must be delivered deep enough into the tissue to reach all the way to the end of the roots. An anesthetic working time of five to eight minutes is sufficient to achieve sensation control.
On mandibular teeth, the cannula is placed into the tissue just inferior to the maxillary second molar, and the prilocaine is injected slowly as the cannula is advanced toward the ear and along the ramus of the mandible. The remainder of the carpule is emptied at the suspected mandibular nerve location and followed by two carpules of articaine to the same location, with one minute between each carpule.
Most dentists who use these anesthetics report significantly greater anesthesia success. Keep in mind that some reports show an increase in the risk of paresthesia than with other 2 percent strength anesthetics. Since both of these anesthetics are 4 percent in strength, they should be injected slowly after aspiration to decrease chances of neurotoxicity and longer-than-desired paresthesia.
With these 4 percent anesthetics, the need for intrapulpal, intraligamental, or transosseous injections is much less. However, in those rare times of difficulty in numbing, the transosseous method is extremely effective. Stabident (Fairfax Dental) provides reliable anesthesia in almost any situation. Using a small osseous perforator on a slow-speed hand piece, a small amount of anesthetic is delivered through the cortical plate between adjacent tooth roots. Anesthesia is almost always reliably achieved in even the hardest-to-numb situations.
5. You can’t fix what you can’t see
Since the assistant gets tired holding a magnifying glass over the tooth during long procedures, loupes with magnification are used in many dental offices. Loupes are fairly inexpensive and comfortable. Surgical microscopes would be nice in every operatory; however, most of us don’t have them.
Finding canals, locating fractures, and excavating decay are exponentially easier with 2.5 to 4.0 magnification loupes. If they have fiberoptic lighting, it’s even better. Once a classic endo access is made, even those “fourth” canals in upper molars are seen more easily. In those cases where a canal is hard to find, a caries indicator helps locate them. After removing all soft tissue from the pulp chamber, dry it thoroughly and apply a liberal amount of caries indicator. After rinsing and drying well, the missed pulp canal can often be seen.
6. Tooth preparation
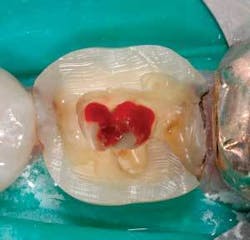
Visibility is often the limiting factor for chamber and canal identification. Rubber dam use and classic endo prep are critical. Because the general dentist is usually the professional in charge of the final restoration, it is occasionally advantageous to do the definitive restoration prep prior to doing the endo. Doing the prep first can remove tooth structure that would otherwise be in the way, and decrease the time needed to locate wayward pulp tissue (Fig. 3).
Rotary files are now the standard in many offices. They are made of metals that flex easily and make canal preparation much faster than with hand files. They also are particularly safe to use with the newer electric handpiece engines with automatic reverse feature, should too much torque be placed on the file.
7. Finding the canal lengths
Electronic apex locators are terrific these days and, like digital X-rays, have reduced the amount of radiation exposure in many offices. These length-finding devices work best if the pulp chamber is devoid of soft tissue and blood, which is often present when the tooth is opened (see Fig. 3).
Once the pulp chamber is cleaned out, the electronic probe is placed on the file and taken toward the apex. Results are extremely accurate, within .5mm of the apical constriction. The Root ZX (J. Morita) works best when:
- The filling material is removed first
- The pulp chamber is rinsed well with water
- A small file is quickly taken down the canal to remove excessive tissue
- The canal is dried with air before using irrigants.
The electronic apex locator can remove the aggravation caused by waiting for poorly composed X-rays to be developed.
8. Single-appointment obturation
Single-visit endo is widely accepted in the industry. Not only is it more efficient for the office, it is a benefit for the patient in that there is no second appointment or anesthesia. You also have the opportunity to complete the procedure while the tooth morphology is fresh in your mind. In most cases, the long-term results are the same as multiple-visit endo.
Lateral and vertical condensation with master and auxiliary points has been the standard in endodontic therapy for many years. However, newer materials can simplify treatment and may provide a better bacterial seal, resulting in better long-term results. ThermaFil (DENTSPLY Maillefer) has been around for nearly two decades, and has proven to be quite effective with much research behind it. Most studies show the bacterial leakage to be at least as good as vertical condensation as long as a sealer is used. With accurate length determination, thorough canal preparation, and effective disinfection, these obturators make it almost as easy as making a hole and stuffing something into it.
Newer epoxy-resin sealers and obturation materials such as Resilon and Epiphany may provide the best antibacterial sealing yet while being kind to tissues. These materials can decrease postop concerns by allowing less microbe proliferation, which can decrease future patient problems and stress for the dentist.
9. Definitive restorations help prevent failure
Definitive, nonleaking restorations may be as important to endo success as filing and obturation. The sooner the definitive restoration is placed, the greater the likelihood of treatment success: studies show it only takes 30 days for bacteria to migrate down the root and contaminate the apex from a faulty coronal seal. We have all seen patients with a grossly decayed molar that had previous endo who say, “I never had it finished.” It’s a shame so many patients leave the office with an endo temporary, experience no pain, and then return after the tooth is too far gone to restore it.
The general dentist is in a great position to place the definitive restoration at the endodontic appointment. As long as the occlusion is properly adjusted, placing a more long-term restoration of composite, onlay, or even crown may be more important in endodontic success than filling to the apex. Provisional restorations have been shown to leak almost immediately. Placing at least a well-bonded build-up material or composite may increase your endodontic victories.
10. We have a support group
We have specialists who deal with endo complications and difficult teeth every day - we always have the option to refer when the case appears too difficult or when we have complications. Having the endodontist standing behind us is comforting; however, his or her support does not give us the right to consistently get in over our heads. Continuing education and reading the clinical literature are the best ways to increase our skills and comfort levels, as well as learn our limitations.
Doing endo routinely in general practice is both rewarding and one of the lowest-overhead procedures we can do. Endodontic therapy is rewarding as long as sound systems are used for diagnosis, treatment, and tooth restoration. The only fear with endo should be running out of supplies from doing so many.Dr. Jack Griffin has maintained a full-time practice in St. Louis county, Mo., since 1988. In a busy practice, his office has consistently maintained a 50 to 55 percent overhead doing all phases of dentistry with an emphasis on cosmetics. The practice is focused on current technologies, materials, and procedures, and is the head of the Missouri MasterTrack AGD program and the St. Louis area CEREC study club. Dr. Griffin also speaks at many study groups and courses.