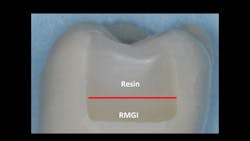
Reducing caries in proximal boxes of Class II resin restorations
Q: I am a practitioner of many years, and I have a frustrating question for you. For most of my career, I have used amalgam as my primary operative dentistry restorative material. Although unsightly, it has served my patients very well. A few years ago, I started to use resin-based composite as my primary material. The initial esthetic result has been very gratifying, but now I am seeing far more caries on the apical portions of Class II box forms and marginal breakdown on occlusal extensions than I have ever seen on amalgam restorations. Is there something I am doing wrong, or is this what I should expect from composites?
A: You are not alone. This phenomenon is being observed throughout the profession. Research on the challenge is minimal, but let’s discuss several concepts that, in my opinion, probably contribute to the problem. I will state the issues and provide a potential solution for each.
Curing lights
Authorities in dental-resin light curing have shown that up to two-thirds of curing lights are ineffective in typical general dental practices in North America. So, what is wrong with the lights? A variety of problems have been found to be present; among them are: older generation low-energy lights, cracked or broken light guides, curing lights with degenerated lamps, debris on the tip of the light guide, and numerous other challenges.
The solution? Get a new light. Examples of well-researched and proven lights that Clinicians Report Foundation has found include: Bluephase Style from Ivoclar Vivadent, Elipar from 3M, Fusion from Dentlight, The Light from GC, Valo from Ultradent, and numerous others.
Proper use of lights
Another problem with lights is they are being used improperly. The light energy emitted from the tip of your light guide should be aimed perpendicular to the resin surface and as close to the resin as possible without touching it. The light should also be used for an optimum time.
You can determine the time required for your light by making a test sample about 10 mm thick of your most-used color and brand of resin. Place the sample on a white piece of paper. Cure the resin from the top of the 10-mm sample, and then turn the sample over and scrape the bottom portion of it with a knife. When you cannot scrape any more partially cured resin off the test sample, it indicates that the remaining resin is converted to the optimum extent.
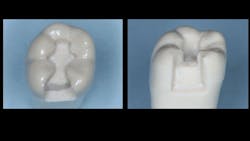
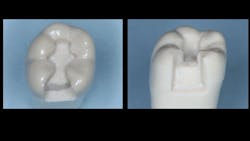
Figure 1: A typical GV Black prep is shown here. Much smaller preps are now promoted and accomplished, but the sample shown is about the size that is seen after a tooth has had a previous restoration removed. Tooth preparations are conventional for this technique without significant modifications.
Partially cured resin feels hard, but you can still scrape it off. Trying to cure resin deeper than what your light can do is foolish and will cause failure. After doing this rather crude test, adjust your curing time accordingly. Don’t trust the suggested curing times as stated by the manufacturers. Lights can vary significantly!
Note: When placing resin restorations, remember to use an airstream from your air/water syringe on the tooth to cool the tooth and the pulp.
Bulk filling
Although bulk filling done properly can work well, the fact is that many clinicians do not use this technique to an optimum degree. Some of the observed disadvantages, challenges, and improper use of bulk fill are:
- Ensuring complete resin polymerization because of poor curing light utilization, as stated above
- Making adequate contact areas
- Overfilling, which causes significant finishing effort and potential margin damage
- Potential increased finishing time
- Developing a “white line”–margin ditching due to aggressive finishing of the bulk material
- Influence of typical 2% restorative resin shrinkage, which pulls the resin mass away from the apical margin of the box form and toward the light source, opening the apical margin of the box
Reducing some of these challenges can be accomplished by using the following bulk-fill technique:
1. Prep the tooth with special attention to the box form to remove all caries.
2. Accomplish your normal etching/bonding technique on the entire prep.
3. Place a small amount (0.5-mm thick) of the restorative resin you are using or a similar amount of a flowable resin on the most apical portion of the box. After curing, this technique attaches the small amount of resin to the apical portion of the box and can minimize how much the subsequently placed bulk of resin pulls away from the gingival margin.
4. Continue with the major resin placement.
Disinfection of the tooth preparation
Although not known or practiced by most dentists, disinfection of the tooth preparation has been shown by the Technologies in Restoratives and Caries Research (TRAC) Division of Clinicians Report Foundation to greatly reduce the quantity of microorganisms remaining in tooth preparations. The most adequate application technique is placement of one of the following products: G5 by Clinicians Choice, Gluma by Kulzer, Glu/Sense by Centrix, or MicroPrime by Zest.
With a microbrush, carefully place a small amount of one of these solutions on the tooth preparation. Allow the solution to remain on the tooth preparation for one minute, and then suction—not wash—it off. A second one-minute application is mandatory for optimum disinfection. Placement of the glutaraldehyde-containing solution should be done immediately after completing the prep and before any liners or bases. This procedure both desensitizes and disinfects the preparation.
Cariostatic restorative materials
Conventional resin-based composite does not have cariostatic properties. With any patient for whom future caries involvement is expected, the use of cariostatic liners, bases, and restorative materials is a wise choice. This technique is well-known in countries where amalgam has been criticized and/or banned:
1. Make a standard Class II preparation for resin-based composite in a well-isolated clinical field (figure 1).
2. For a normal-depth tooth preparation, a typical acid-etch/bonding technique is now used, including two one-minute applications of a glutaraldehyde solution between the etch and bond as described previously. If a liner is deemed necessary, the glutaraldehyde solution should be used before the liner, with a brief additional contact with glutaraldehyde after the acid etch and washing.
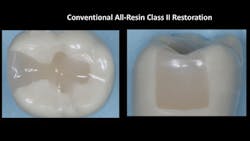
3. At this point in the process, the clinician may elect to use a cariostatic restorative material. However, a typical Class II resin-based composite restoration (figure 2) would have minimal caries potential if the proper light techniques discussed previously were present and the patient had optimum oral hygiene.
Figure 2: Although Class II resin-based composites often look excellent when initially placed, a few years of service frequently shows significant degeneration of margins and recurrent caries.
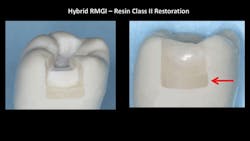
4. To use the cariostatic restorative material, a matrix is placed as usual and a preventive restorative material is placed in the apical one-fourth or one-third of the proximal box (figure 3). Excellent examples of new currently available preventive materials are Equia Forte from GC and Ketac Universal from 3M. These conventional glass ionomers have high fluoride release, faster set, increased resistance to dissolution, and greater strength than previous generations.
Figure 3: Cariostatic material—in this case Equia Forte from GC—placed in part of the box form is commonly used in countries where amalgam is not used. This technique can greatly reduce the incidence of new caries on the apical portion of box forms.
5. Typical composite resin is placed in the remainder of the tooth preparation and finished in a conventional manner (figure 4).
This technique is especially desirable for patients who have known active caries tendencies, deep box forms, poor hygiene, or poor diet.
Figure 4: This restoration has cariostatic material on the apical portion of the box form, and conventional resin-based composite on the remainder of the box form and the occlusal surface.
Use of a dual-curing restorative material
A relatively new concept that still needs significant clinical research and observation is the use of dual-curing restorative materials. This concept has the potential to reduce or eliminate the threat of the light-curing challenges described in this article, including the shrinkage of resin caused during polymerization that pulls the resin up from the apical portion of the box form toward the occlusally placed light source. This is not a well-known concept among most dentists.
Example products are: Bulk EZ from Zest, Fill-Up! from Coltene, HyperFil from Parkell, Injectafil from Apex, and LuxaCrown from DMG America. Some practitioners are using such materials in the proximal box and conventional light-cured resin on the occlusal areas.
Summary
There is no question that resin-based composites can have significant carious lesions occur around their margins. That problem is especially present on the proximal box form in the most apical location. I have discussed several techniques expected to reduce or eliminate this problem. Although some of the techniques are relatively new and require more long-term research, the technique using a cariostatic material in a portion of the proximal box is well-proven in countries where amalgam is not used.
Author’s note: Additional educational resources are available from Practical Clinical Courses, some of which relate directly to this article:
Two-day courses in Utah
• Restorative Dentistry 1—Restorative/Esthetic/ Preventive with Dr. Gordon Christensen
• Restorative Dentistry 2—Fixed Prosthodontics with Dr. Gordon Christensen
One-hour CE videos
• Class II Composite Resins Can Be Predictable, Non-Sensitive, and Profitable (Item No. V3554)
• Mastering Frequent Esthetic Challenges with Resin (Item No. V3582)
For more information about these educational products, call (800) 223-6569 or visit pccdental.com.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.