Using Combination Microabrasion, MI Paste, And Whitening To Treat Fluorosis Stains
By Jessie Stasulis, DMD
Enamel fluorosis is a common dental condition wherein teeth have intrinsic white or brown mottling or striations. Fluorosis is caused by hypomineralization in the enamel due to increased fluoride ingestion during early childhood (the second and third years of life in particular). These stains can be quite esthetically displeasing to patients, and most are unaware of the treatment options available. Previously, fluorosis stains were treated aggressively with hydrogen peroxide and heat, phosphoric acid with Superoxol, composite veneers, porcelain veneers, or even full coverage crowns. Thankfully, it is no longer necessary to compromise healthy tooth structure or risk damaging pulp tissue in order to achieve optimal esthetics. The combination therapy of enamel microabrasion, MI Paste™ (GC America) application, and at-home bleaching described in this case report provides predictable results and patient satisfaction.
Enamel microabrasion is a nonrestorative, conservative treatment that works both chemically and mechanically to remove up to 0.2 mm of affected enamel per application. For some patients, the depth of the staining may be beyond the scope of microabrasion alone. Conservatively targeting the deeper stains (without covering them with composite) can be achieved by adding MI Paste to the treatment sequence.
Lastly, at-home bleaching is encouraged for patients to brighten the transformed smile. The following case is an example of the results that can be achieved by this combination therapy.
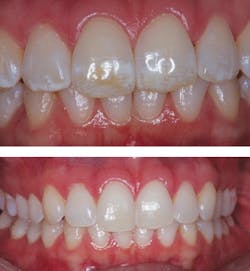
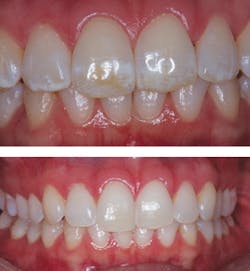
A 27-year-old female presented with healthy dentition but was not content with the esthetics of her teeth. Both maxillary and mandibular anterior teeth displayed white and brown mottling due to enamel fluorosis. The patient desired removal of the affected areas, and a whiter, brighter smile. The treatment protocol was as follows:
I placed local anesthesia from bicuspid to bicuspid in the maxilla and the mandible. I achieved isolation with a rubber dam from second bicuspid to second bicuspid in the maxilla to protect the gingiva from the hydrochloric acid. In areas with deeper stains, I used a superfine grit diamond in a light sweeping motion for five to 10 seconds to allow penetration of the hydrochloric acid, as well as to remove surface stains from affected teeth.
I placed Opalustre slurry (Ultradent, a slurry of 6.6% hydrochloric acid and silicon carbide microparticles) on each tooth in 1 mm thick increments. I then attached a contra-angle, slow-speed handpiece with an Opalcup, and at a slow RPM, I applied medium to heavy pressure for 60 seconds to each tooth. I then carefully rinsed and lightly dried the treated teeth to evaluate the results. I performed two more microabrasion treatments to affected maxillary teeth and, after proper isolation of the mandibular teeth, repeated the sequence described above. I then finely polished the teeth with sandpaper disks and silicone polishing burs.
Once the microabrasion was complete, fluoride trays filled with APF gel were placed for four minutes. The excess fluoride was suctioned and the patient was instructed not to eat or drink for at least 30 minutes.
For the next three weeks, the patient placed MI Paste in her custom bleaching trays and slept with the trays in place. The following two weeks, the patient performed at-home bleaching. The patient was very pleased with the results and now smiles with confidence.
Jessie Stasulis, DMD, practices general dentistry in Terryville, Conn. She graduated from the University of Connecticut School of Dental Medicine in 2008 as a member of the OKU Dental Honors Society and is an active member of her state and local dental societies. You may reach her at [email protected].
Past DE Issues