Are posts really necessary in endodontically treated teeth?
Editor's note: Originally published in 2012. Reviewed for clinical accuracy and formatting in 2022.
Q: I'm confused about the necessity of using posts in endodontically treated teeth. Some publications and speakers say that posts are always necessary, and others say they are never necessary. When, if ever, should posts be used, and what type of post should be used?
A: During my career to date, I have watched the use of posts and cores for endodontically treated teeth evolve from complicated, expensive, difficult to make, custom cast posts and cores, to metal prefabricated posts made from stainless steel, to titanium or titanium alloy, to today's popular fiber-reinforced resin-based composite. In my opinion, there have been numerous misunderstandings about the need or lack of need for posts.
I will discuss several factors to consider before making a decision about whether or not to place posts in endodontically treated teeth. My conclusions about posts are based not only on the research literature, which contains many excellent but sometimes confusing in-vitro studies on extracted teeth, but also my clinical experiences over many years as a practicing prosthodontist.
Factors to consider
Many have stated that the main reason for placing a post is to strengthen the connection between the coronal build-up material or remaining tooth structure to the root portion of the tooth. In my opinion, that is only partially true. Additionally, the following potentially negative or positive factors should be considered in the decision to use a post. All of these factors should be observed before making the decision:
• Quantity of remaining tooth structure
• Quality of remaining tooth structure
• Remaining adjacent teeth
• Occlusion
• Planned restoration to be placed on the tooth
Also by Dr. Christensen:
Increasing practice activity: An ongoing team effort
Is an implant better than a tooth?
Quantity of tooth structure remaining
Some teeth have most of the coronal tooth structure remaining after endodontic treatment, and others have very little tooth structure remaining. What is the significance of the amount of remaining tooth structure? For simplicity, I'll divide the discussion of remaining tooth structure into several categories, and I'll list them in decreasing order of clinical success:
All of the coronal tooth structure present except the endodontic access hole
If other negative factors (to be discussed later) are not present, such teeth usually do not require posts. After the endodontic procedure is completed, tooth colored resin-based composite should be bonded into the pulp chamber. These teeth usually continue to serve adequately as though they were vital teeth.
At least one-half of the coronal tooth structure remaining
This situation is one of the most common. Assuming the remaining coronal tooth structure does not have any of the negative characteristics discussed next, the occlusion is not heavy, and there are other teeth contiguous with the one being treated, this tooth may not need to have a post. The coronal tooth structure can be built up, usually with retentive resin-based composite build-up material, to provide additional retention for the subsequent restoration, and these teeth have excellent potential to serve uneventfully. However, if other negative factors are present, it is prudent to place a post.
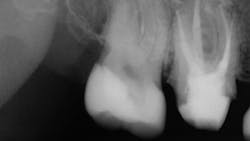
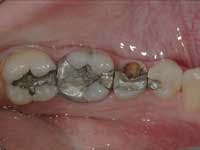
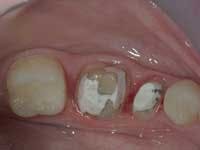
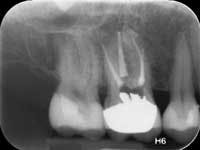
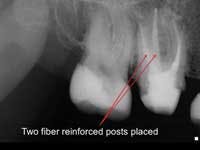
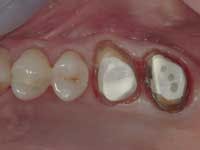
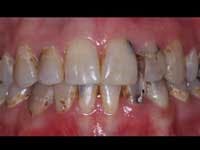
Less than one-half of the coronal tooth structure remaining (Figs. 1-6)
It is my opinion, regardless of the other factors present, that it is still advisable to place a post or posts in such teeth. Endodontically treated teeth with less than one-half of the coronal tooth structure remaining have a reduced chance of long-term service, and patients should be so advised as the treatment plan is developed.
No tooth structure remaining coronal to the gingival tissue
There are clinical situations in which these teeth should be retained, including if the practitioner plans to extrude the tooth orthodontically. However, when considering the clinical success of dental root-form implants compared to questionable teeth, it is often better to extract the teeth and place implants. In the debatable event that a decision is made to restore such teeth, a post in single-rooted teeth or more than one post in multirooted teeth should be placed. Even with adequately placed posts present, the long-term success of such teeth is very questionable.
No tooth structure coronal to the bone
These teeth should usually be extracted. The only procedure, infrequently accomplished, that may allow teeth with long roots to be retained is orthodontic extrusion of the tooth. However, the cost of orthodontic extrusion and the time involved in waiting for the tooth to extrude and stabilize make the procedure questionable unless there is some major reason to retain the tooth.
Quality of remaining tooth structure
Assuming that there is a significant amount of coronal tooth structure remaining, the quality of the remaining tooth structure should be considered. Often, remaining tooth structure has discolored areas, slightly demineralized areas, cracks, undermined areas, or other negative characteristics. Removal of tooth structure with these characteristics allows a realistic and necessary appraisal of the amount of viable tooth structure remaining. After removing the affected areas, the same suggestions stated in the previous section on quantity of tooth structure remaining apply. Posts are often indicated.
Remaining adjacent teeth
If an endodontically treated tooth stands alone without adjacent teeth present, it will receive significantly more occlusal forces on it when compared to a tooth that has sound adjacent teeth. When restoring a tooth that has no or few surrounding teeth, it is appropriate to use a post or posts to augment the strength of the endodontically treated tooth, and to ensure that the remaining coronal tooth structure is strongly connected to the root portion.
Occlusion
One of the most important factors relative to the question of post placement in an endodontically treated tooth is the nature of the patient's occlusion. Patients with bruxing or clenching habits place far more stress on teeth than those patients with normal occlusion. Usually, bruxers move their mandibles in left-right and forward-back movements, grinding off canine rise and incisal guidance. Enormous lateral stresses are placed on the teeth of these patients. Clenchers place forces in an apical direction with intense load and frequency. A logical decision is to place posts in bruxing and clenching patients.
Planned restoration to be placed on the tooth
An endodontically treated tooth planned to receive a single crown has minimal stress when compared to a tooth that is planned to be an abutment for a fixed prosthesis or an abutment for a removable partial denture. If an endodontically treated tooth is expected to have significant load placed on it in service, posts should be placed.
In summary: Yes, posts are often needed, and there are many clinical factors related to whether or not they should be used, in addition to just how much tooth structure is remaining. Clinical judgment is still critical in deciding whether or not to use posts.