Ask Dr. Christensen
by Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: mini implants, conventional-diameter implants, SDIs, osteotomy, flap operation, Gordon J. Christensen.
Q I have seen many articles and courses supporting “mini” implants, but the oral surgeon with whom I work condemns them. The technique seems to be simple and noninvasive, which makes the controversy even more frustrating to me. What can I expect from the “mini implant” concept for my patients, especially for lower complete dentures?A I have heard complaints about mini implants similar to those you mentioned for more than eight years. During this same period, I have had significant clinical success with these small-diameter implants. I will answer your question by comparing mini implants with conventional-diameter implants in cases of mandibular edentulism. These are the types of cases where they are most recommended. My pictures with this article will demonstrate adequate placement under a mandibular denture.Mini implants are usually defined as root-form implants smaller than 3 mm in diameter. This definition is related to the 1976 FDA clearance of root-form implants 3 mm in diameter and larger and the subsequent initial 1977 FDA clearance of root-form implants under 3 mm in diameter for “long-term” use. Those persons and groups defining implant terminology are trying to call these small implants “small diameter implants, or “SDIs.” However, the phrase “mini implants” is already so embedded in the dental terminology that it will probably continue to be used.
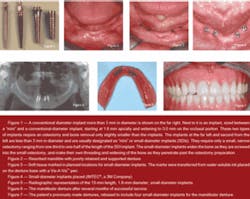
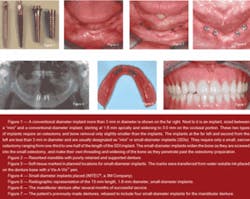
Figure 1 shows the differences in the diameter of SDIs (less than 3 mm compared to conventional-diameter implants (3 mm and larger). The most common and needed use of SDIs is for mandibular edentulism, which is the most debilitating, frequently occurring condition in dentistry. There are numerous research projects supporting the use of SDIs for mandibular dentures. If you are interested, visit the Web site, www.pubmed.com, and read these research reports.
My use of SDIs for mandibular edentulous patients has become routine; however, I still use both conventional-diameter implants and SDIs for support and retention of mandibular dentures. Most of the elderly edentulous patients I treat have only minimal bone (Fig. 2). These patients are frequently in ill health, and the surgical trauma of conventional-diameter implants is significantly more difficult on them than placement of SDIs. Therefore, if the patient has minimal bone in a facial-lingual dimension and is in ill health, SDIs are definitely the treatment of choice. If these implants are placed adequately and the denture is fabricated adequately, there are no reasons to question the use of SDIs.
On the other hand, if the edentulous patient has adequate bone and appears to be in good health, conventional-diameter implants, which have been used for nearly 50 years, should provide excellent support and retention for mandibular overdentures.
A state-of-the-art comparison of SDIs with conventional-diameter implants is revealing. It makes the decision on whether to use conventional-diameter implants or “mini implants” for edentulous mandibles more difficult. The following comparison explains my opinions on the subject:
• SDIs expand the bone as they are placed, producing immediate stabilization in most situations with minimal bone removal. Most conventional-diameter implants are placed in an osteotomy only slightly narrower than the implant diameter.
• SDIs require only a narrow-diameter osteotomy that does not extend to the depth of the implant. Conventional-diameter implants require an osteotomy extending to the entire depth of the implant, thereby removing significantly more bone.
• SDIs usually are loaded on the day of placement, reducing the length of the treatment period. Most conventional-diameter implants are not loaded immediately, requiring the patient to use a provisional restoration for a longer period of time.
• In the event of the infrequent failure of an SDI, it is merely unscrewed and the osteotomy closes and heals within a few weeks.
• SDIs cost significantly less than conventional implants; however, two SDIs must be used where only one conventional-diameter implant would have been used. Therefore, cost of implant therapy is only slightly less for the SDI technique.
• The surgical trauma caused by an SDI placed without a soft-tissue flap is minimal, and most patients do not require an analgesic postoperatively. In a recent CLINICIANS REPORT survey of 200 SDI users (CRA Newsletter, November 2007), only 20% of SDIs were placed with a flap operation. It has been estimated that the reverse is true with conventional-diameter implants, with 80% requiring a flap.
• Placement of SDIs is relatively easy after obtaining minimal continuing education.
• Placement of conventional-diameter implants is somewhat more difficult than SDI placement.
Several brands of small diameter implants have been cleared by the FDA for “long-term” use. These brands are:
- Dentatus® — www.dentatus.com, (800) 323-3136
- Dental Implant Technologies — www.dentalimplant tech.com, (800) 452-0582
- Implant Direct™ — www.implantdirect.com, (888) 649-6425
- IMTEC®, a 3M Company — www.imtec.com, (800) 879-9799
- INTRA-LOCK® System International — www.intra-lock.com, (877) 330-0338
- Sterngold® — www.sterngold.com, (800) 243-9942
Making the decision on whether to use conventional- implant or SDI techniques for edentulous patients requires consideration of the following points:
1) Quantity of bone: The following are my suggestions concerning the amount of bone necessary for conventional implants and SDIs. Few patients want to have or can afford extensive bone-grafting. Therefore, the amount of bone present is a major factor in deciding which concept to use.
For implants 3 mm and larger (conventional diameter):
6 mm in a facial-lingual dimension
10 mm in a crestal-apical dimension
1 mm to 2 mm from vital structures
For implants up to 3 mm in diameter (SDIs):
3 mm to 4 mm in a facial-lingual dimension
10 mm in a crestal-apical dimension
1 mm to 2 mm from vital structures
2) Quality of bone: Dense bone is significantly better for SDIs than highly trabeculated porous bone. If the bone is porous in the area being considered, conventional implants are probably the best choice.
3) Age and physical health of the patient: If the patient is older and has significant physical health challenges, the SDI concept is easier for the dentist and less threatening for the patient.
Technique for small-diameter implants for mandibular overdentures (Figs. 3-7)
- Deliver typical local anesthetic.
- Decide on the best location for the implants by marking the internal area of the denture and transferring the marks to the soft-tissue.
- Decide whether to make a flap to facilitate implant placement. Making a flap is usually necessary only for minimal facial-lingual bone (3 mm to 4 mm).
- Place the SDIs.
- Make an impression to rebase the patient's previous denture or to make a new one. Various attachments including rubber “O” rings, ERA, or Locator attachments can be used, depending on the SDI brand used.
- Rebase the previous denture or make a new one.
- Seat the denture and adjust it.
- Readjust the denture after a few days.
As a brief summary answer to your question, “mini implants” are not only working well, they also have been cleared by the FDA, supported in the research literature, and they provide a viable alternative to the more invasive, time-consuming, and somewhat more expensive conventional-diameter implant concept.
However, don't forget about conventional-diameter implants, which are great for use in some overdenture situations where adequate bone is present.
Practical Clinical Courses (PCC) has significant information available on “mini” implants in hands-on courses and live clinical-action video. Call (800) 223-6569 or visit our Web site at www.pccdental.com for more information.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and Dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.