Ask Dr. Christensen
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e–mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: small–diameter implants, SDIs, bone–grafting, bone quality, posterior maxilla, anterior mandible, trabecular bone, Dr. Gordon Christensen.
Q I have heard contradictory reports on the success of small–diameter implants, although I have had repeated success using them. The criticisms that I have occasionally heard make me nervous. Should I continue to use them or are there some reservations?A Thanks for your candid question. I will answer it using research, clinical observations, and my own opinions. I will also make suggestions relative to why a few practitioners have had some failures with small diameter implants (SDIs) or “minis.”You know as well as I do that many patients do not have adequate native bone quantity or quality to place conventional diameter implants, which require at least 6 mm of bone in a facial–lingual dimension, and 10 mm in an occlusal–apical dimension or significant bone grafting. SDIs often can be placed in 3 mm to 4 mm of bone in a facial–lingual dimension and 10 mm in an occlusal–apical dimension. Many patients, especially those in their senior years, cannot tolerate significant surgery, including bone–grafting. They are frequently physically or financially disadvantaged, which further limits their acceptance of conventional diameter implant therapy. SDIs are a proven alternative for many of these patients.
As you may know, the FDA clearance for small–diameter implants (<3 mm in diameter) for “long–term use” came in 1997.This FDA clearance came many years after the FDA clearance of conventional diameter (>3 mm in diameter) implants in the late 1970s. Obviously, conventional–diameter implants have proven themselves over decades of use, experimentation, and refinement. In my opinion, root form implants are the most important innovation in dentistry since the air rotor in the late 1950s, and they are now considered a routine part of oral therapy.On the other hand, research on SDIs for long–term use has had only about 12 years to mature. Many innovations in SDIs have taken place during that time, but refinements are still coming, and additional manufacturers are entering the SDI marketplace. As a result, some experienced dentists who have been successfully placing conventional–diameter implants have been skeptical about the long–term effectiveness potential of SDIs. Thus, the active controversy about this subject has continued.
Both general dentists and specialists of all varieties are placing implants. There is no specialty for implant placement, although some groups want to claim ownership of this area of dentistry. As an experienced surgically–oriented board–certified prosthodontist, I can say without reservation that a properly educated dentist of any orientation can successfully place root–form implants of any diameter in healthy patients who have adequate bone. I deny the allegations that root–form implant placement is a complex and difficult procedure for dentists who have had proper education and guidance on implant placement. Many other areas of dentistry are more challenging than implant placement. SDIs are certainly no exception.
The research on the success of small–diameter implants speaks for itself! Research projects on long–term service of SDIs show more than 90% retention of thousands of SDIs over various periods of time and for a variety of uses. The success percentages rival closely those of conventional–diameter implants.
My conclusion on the success of SDIs is that if practitioners are not having success with SDIs, they must be doing something wrong. I will direct the remainder of my answer to that point — i.e., what can you do wrong in diagnosis and treatment–planning, placement, and restoration of SDIs?
Diagnosis and treatment–planning
Bone quality and quantity vary enormously from patient to patient. In case you are not clear on bone classifications, the four classifications (as described by Misch) of oral bone are:
- D1 — Dense compact, resorbed anterior mandible
- D2 — Dense to porous compact on the outside and coarse trabecular bone on the inside, anterior and posterior mandible, occasionally anterior maxilla
- D3 — Thinner porous compact bone on the outside and fine trabecular bone on the inside, anterior and posterior maxilla and posterior mandible
- D4 — Fine trabecular with little or no cortical bone, posterior maxilla
SDIs range from 1.8 mm to 2.9 mm in diameter. Thus, they are not wide enough to reach dense cortical bone on the facial and lingual surfaces if the facial–lingual bone dimension is wide. Wider–diameter conventional implants are recommended in those areas (4, 5, and 6 mm diameter).
The most appropriate locations for SDIs are in dense bone, D1, frequently D2, and D3 when the facial–lingual bone dimension is narrow. D4 is never an appropriate location. If the preceding statements are not recognized and used as guidance for diagnosis and treatment–planning, the SDIs will fail.
Radiographs that show only two–dimensional, panoramic, periapical, or bitewing views do not show the density of bone in a facial–lingual dimension. Tomographic or cone–beam radiographs are strongly recommended before placing any diameter of implant to allow visualization of bone characteristics in a facial–lingual dimension. These types of radiographs are available in most communities if you do not have that capability yourself. If the bone appears to be porous in any dimension, conventional–diameter implants are a better choice than SDIs.
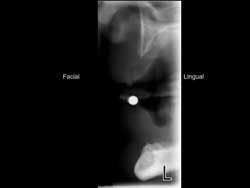
Patients having the previously described bone characteristics — i.e., at least 3 or more mm of bone in a facial–lingual dimension and at least 10 mm of bone in an occlusal–apical dimension — are excellent candidates for SDIs (see Fig. 1).
Placement of small-diameter implants
Currently, the most popular SDI brands listed in order of decreasing use are: MDI from Imtec, a 3M Company (Ardmore, Okla.); Atlas by Dentatus (New York, N.Y.), and the ERA Implant System by Sterngold (Attleboro, Mass.). Several other brands are on the market, and others are coming.
When adequate bone is present as described, SDIs may be placed without making a surgical flap. However, in my considerable experience placing them, I prefer to make a conservative flap, especially if the bone quality is at all questionable.
The initial osteotomy depth is directly related to the density of the bone. Dense bone requires an osteotomy of up to one–half the length of the implant. Less dense bone should not have deep osteotomies. One–fourth to one–third of the length of the implant is desirable. This allows condensation of the bone as the screw–shaped implant is rotated into place. Making osteotomies too deep dooms the implant to failure. You should feel significant resistance screwing the implant into place for success.
As reported by manufacturers, the average length of SDIs placed is about 13 mm. I suggest that shorter implants must be in dense, preferably Type D1, bone for success.
The less the implant protrudes from the bone, the less the lever arm is on the implant when loaded, and the better the chance for success. If coronal soft tissue over the implant is thicker than 2 mm, I suggest removing the excess using a V–shaped wedge on the occlusal and closing it with simple suturing.
My recommendations would be to place two SDIs for every location where you might have considered one conventional–diameter implant to be sufficient. As an example, in an edentulous mandible, you may have considered two implants, 3 mm or more in diameter, one in each canine area, to be sufficient.
When using SDIs, two implants either in the general canine area or spread evenly from canine to canine are recommended. Some dentists and companies are using six SDIs in such situations. I have had routine success using four implants in mandibular arches, and occasionally six in the less acceptable bone in maxillas.
The implants should be as parallel as possible, although divergence from parallelism up to 15 degrees has been shown to function well.
SDIs are usually loaded immediately on placement, or if a flap has been used, up to two weeks after placement. If waiting to load the implants, make sure that soft denture liner is placed in the old prosthesis to prevent excessive load being placed on the implants during their healing period.
The above suggestion reduces or eliminates failure when placing the implants.
Restoration of small-diameter implants
Most dentists using SDIs have experienced success well more than 90% of the time. The uses are listed below in order of decreasing reported frequency of use:
- Edentulous mandibles
- Edentulous maxillas
- Augmentation of retention and support of mandibular removable partial dentures
- Augmentation of retention and support of maxillary removable partial dentures
- Augmentation of retention and support of fixed partial dentures
- Sole retention and support of fixed partial dentures
- Sole retention and support of single crowns
Categories 1 through 4 have high success, and I do not resist suggesting their use when adequate bone is present. In my opinion, Categories 5 through 7 need additional research and observation. However, many dentists are using SDIs in Categories 5 through 7 with reported success, and I will use SDIs in these situations if there are no other viable alternatives.
Restoration of SDIs is no different from restoration of conventional–diameter implants. I have the following suggestions based on my own experience and observation of available research:
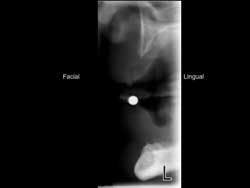
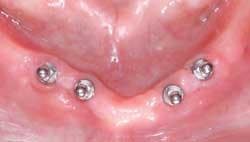
- Use flexible “O” ring attachments whenever possible with complete and partial dentures. The flexibility afforded by these attachments reduces the chance of too much load being applied to any implants (see Figs. 2 and 3).
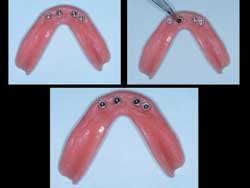
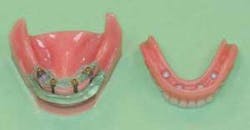
- When the bone is dense, SDIs can use abutments such as the Sterngold ERAs. Four implants in dense bone on the mandibular arch with ERA abutments provide an excellent stable service for patients (see Fig. 4).
- Usually, flexible “O” rings fitting over spheres are used as abutments, but some brands of SDIs, including the IMTEC system shown here, have provided tapered abutments that can be used for fixed prostheses (see Fig. 5.)
In summary, the rumors that SDIs are not acceptable are grossly overstated, and are usually started by persons not familiar with the techniques or research on the subject. If SDIs are planned, placed, and restored properly, there is no reason they should not serve well over many years.
To further answer your questions, Practical Clinical Courses has two one–hour videos that show in live, close–up views the placement and restorations of small–diameter implants. They are:
V2317, “Mini Implants for Your Practice”
V2337, “Restoring Mini Implants”
We also have a popular two–day, hands–on course offered both in Provo, Utah, and Scottsdale, Ariz., that will further prepare you to place and restore these small–diameter implants. Call or contact PCC for details and dates. For more information, visit us online at www.pccdental.com or contact us by phone at (800) 223–6569.
Editor's Note: References available upon request.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing–education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.