Treatment of the aging patient
Q: I practice in an area where there are mostly older adults, and many of them have been my patients for decades. As these patients continue to age and acquire the health maladies of old age, they become major challenges for dental treatment. What do you advise to keep these patients pain free and comfortable as they near the end of their lives?
A: I share your frustration, since I have many similar patients. I will describe one example of this type of challenging patient as he or she reaches this time of life. Usually, you have been providing preventive care and treatment for this patient for many years. Throughout this time, the patient has been able to afford the necessities of dental treatment, including restorative dentistry, some crowns, maybe a few implants, and routine dental hygiene. The treatments have served for many years and appear to be in serviceable condition, but they are becoming increasingly questionable.
However, what happens to this aged patient as he or she experiences poorer health? Unfortunately, his or her zest for life can be markedly reduced. Oral hygiene depreciates significantly. Plaque and food debris are consistently present in the mouth. Diet degenerates into softer, sugar-rich foods that pack constantly around the teeth. Life begins to be difficult, and daily chores make the patient more tired and often irritable. The restorative dentistry in the patient’s mouth begins to degenerate. Fixed partial dentures that you placed years ago now have caries on the gingival margins of the abutments, and you can’t determine if the carious lesions are progressing deeply under the crowns. You hope that they can be salvaged. Periodontal disease is now increasing without adequate oral hygiene. The patient becomes intolerant of dental procedures, unpleasant, and difficult or nearly impossible to treat.
Have I described this kind of older patient adequately? With a few exceptions, these are not pleasant patients.
What is the best way to keep them pain free and comfortable as they pass through this last season of life?
Minimally invasive treatment
If it is obvious that the patient has the previously described characteristics, and it is your opinion that things are not likely to change, minimally invasive procedures are in order. Some of the most important procedures and concepts you can focus on are frequent hygiene appointments, use of a 5,000 ppm fluoride toothpaste, trays with fluoride gel in them, preventive restorative materials, gentle treatment, and avoidance of difficult, expensive treatment. I will elaborate on each of these areas below.
Frequent hygiene appointments
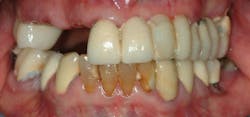
Debridement of the teeth and periodontal pockets on a two- or three-month schedule allows not only removal of debris, but it also allows you to accomplish a thorough exam more frequently to see the progression of caries and other oral problems before they require more difficult and expensive procedures (figure 1). Another advantage is clear. Hygiene appointments are usually relatively pain free, and patients feel better after the appointments are completed. Additionally, oral hygiene instruction provided on a more frequent basis just might encourage better patient hygiene behavior.
Figure 1: A near-90-year-old patient with missing teeth and many restorations that are questionable and need repair. Frequent recare appointments can reduce the need to accomplish extensive dental treatment.
Use of a 5,000 ppm fluoride toothpaste
Elderly patients are much less likely to change their oral hygiene procedures significantly, even in the presence of excellent oral hygiene instruction. Most patients brush their teeth at least occasionally, so changing to stronger, more preventive toothpastes is a logical decision. Such a change does not require a major patient behavior change. Over-the-counter toothpastes have about 1,000 ppm fluoride in them, and most patients use them. But they are not as effective as prescription-level fluoride-containing toothpastes. At the very least, put these patients on a 5,000 ppm fluoride toothpaste. Colgate PreviDent 5,000 Booster Plus (1.1% sodium fluoride) is a popular and long-proven brand. Advise patients to use a significant amount of the toothpaste. Tell them to place it around all of the teeth and let it sit on the teeth for a brief time before brushing.
Trays with fluoride gel
Unfortunately, some elderly patients will not comply with this suggestion, so you must make a judgment call as to whether or not to suggest it for them. For patients who are more cooperative and not significantly debilitated, use of fluoride in custom-fitted “suck-down” trays has been shown to provide optimum delivery of fluoride. Make the tray in clear plastic. An example brand is ProForm .030 Retainer Material, or there are many others. This is the same type of material that many dentists use as a shell to make provisional restorations. Patients can usually use them for several months before needing a replacement. The patient should put several drops of 5,000 ppm fluoride gel into the tray, suck the saliva off their teeth, and place the tray(s) into their mouth for five minutes before going to bed. A well-proven example brand is Colgate PreviDent Brush-On Gel.
If the patient lives in a nonfluoridated area, instructions should include removing the tray after five minutes, spitting, and then going to bed. If living in a fluoridated area, patients should remove the tray, spit, rinse with water, spit again, and then go to bed. If patients are willing to do so, a five-minute repeat of the previously described tray technique just after breakfast is advisable, but the before-bed application is the most important one, because the fluoride remains on the teeth as patients sleep.
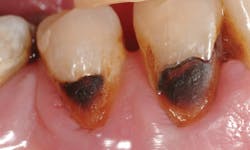
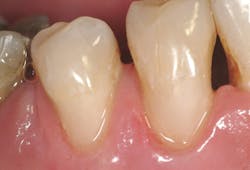
Figure 2: The well-known sandwich technique is often indicated for aging patients. This example has glass ionomer on the inside of the tooth preparations and composite resin on the exterior.
Preventive restorative materials
Oftentimes elderly patients are not concerned about tooth esthetics. Resin-based composites are highly esthetic, but not cariostatic. In fact, they are somewhat cariogenic, since under the observation of a scanning electron microscope, all of the composite restorations have a void around their margins due to the approximate 2% shrinkage in almost all composites. Preferably, use the new forms of conventional glass ionomer in these aged patients. The following example brands have no void around their margins, because there is no shrinkage. They have high fluoride release, better wear characteristics, greater strength than in the past generations, and somewhat better esthetics. Examples include Equia Forte from GC America, IonoStar Plus from Voco, and Ketac Universal from 3M.
Conventional glass ionomer materials are somewhat difficult to use, because they are stickier than typical composites. The suggested process listed below will require some personal experimentation before putting into practice:
1. Begin the tooth preparation for the repair restoration.
2. Have your dental assistant mix the material as you begin the approximate two-minute tooth preparation.
3. Your dental assistant places the material on a paper mixing pad while you finish the prep. The material becomes more putty-like as it begins to set.
4. At the time of the experimental, previously determined desirable putty viscosity, place the material in the prep and cure some bonding agent on it.
5. Go take care of another patient, such as a hygiene check, while the glass ionomer starts to develop some strength.
6. Go back to the restorative patient and carefully finish with a dull bur, such as a No. 7901 12-bladed pointed taper carbide bur, No. 7406 12-bladed football-shaped bur, or other appropriate-shape bur.
7. Place a layer of bonding agent, any brand, on the glass ionomer restoration and cure. The bonding agent will wear off soon, but it protects the restoration from saliva while the material is maturing its chemical set.
8. If necessary, any major finishing can be done on a subsequent recall appointment months later.
Gentle treatment is necessary
Fragile patients deserve careful, gentle treatment. The previous suggestions usually reduce the severity of their dental repair needs and gentle treatment is possible.
Avoid difficult, expensive treatment
Elderly patients may have only a short part of their lives remaining and, in my opinion, extensive treatment usually is not indicated.
As patients near the end of their lives, dental treatment becomes more challenging. The concepts described in this article have been shown to reduce the frustrations encountered when treating patients in this time of life.
Author’s note: The following educational materials from Practical Clinical Courses will help you and your staff better cope with the frustrating topic of this article:
Editor's note: This article was originally published in 2019 but has been updated as of April 2025.
One-hour videos:
- Treating the Aging Population—A Frustrating Challenge (Item No. V4777)
- Diagnosis and Treatment of Failing Implants (Item No. V2391)
Two-day hands-on course:
- Restorative Dentistry 2—Fixed Prosthodontics with Dr. Gordon Christensen
For more information about these educational products, call (800) 223-6569 or visit pccdental.com.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.