Oral and pharyngeal Cancer
by Maria Perno Goldie, RDH, MS
Oral or pharyngeal cancer will be diagnosed in an estimated 30,000 Americans this year and will cause approximately 8,000 deaths. On average, only half of those with the disease will survive more than five years. But with early detection and timely treatment, deaths from oral cancer could be reduced dramatically. The five-year survival rate for those with localized disease at diagnosis is 76 percent, compared with only 19 percent for those whose cancer has spread to other parts of the body. Healthy People 2010 states reduction of the number of oral cancer deaths as one of its goals.
This article will review the facts and causes of oral cancer, prevention strategies, as well as symptoms and warning signs that can provide assistance with early detection. It also will cover the latest detection and treatment modalities and highlight the role of the oral health-care professional in early detection and treatment of this critical health threat.
Incidence
Oral cancer, the sixth most common cancer, accounts for about 3.6 percent of all cancers diagnosed, with roughly 30,000 new cases of oral cancer reported annually in the United States. The vast majority of oral cancers occur in people older than 40 years, with men being twice as likely as women to develop the disease. In Asia, oropharyngeal cancer is the leading cancer in men; in Africa and Asia, it is the third most frequent cancer site in women. The male-female ratio for oral cancer has dropped from 6:1 in 1950 to about 2:1 at present.
The tongue is the most common site for oral cancer in both men and women. Other sites are the floor of the mouth and soft-palate tissues behind the tongue, lips, and gums. If not diagnosed and treated in its early stages, oral cancer can metastasize and cause chronic pain, loss of function, facial and oral disfigurement following surgery, and death.
Etiology
As with most cancers, the exact etiology of oral cancer is unknown. However, the carcinogens in tobacco products, alcohol, and certain foods and excessive exposure to the sun have been found to increase the risk of developing oral cancer. In fact, the use of tobacco products is responsible for 80 to 90 percent of oral cancers. Smokeless tobacco use may increase the risk for oral cancer fourfold. Approximately 12 million Americans use smokeless tobacco, and its use is increasing, especially among young males. A pack of cigarettes per day increases the risk for oral cancer 4.5 times; up to six alcoholic drinks per day, 3.3 times; six to nine drinks per day, 15 times; tobacco and alcohol combined, up to 100 times.
The use of a mixture of tobacco, lime extract, betel nuts, and spices has been observed among immigrants from Southeast Asia, where oral cancer is said to be the most prevalent type of cancer. Risk factors for oral cancer also may be genetically inherited.
Other factors that may contribute to oral cancer are poor oral hygiene, poor nutrition, or irritation from poorly fitting dentures. In addition, the Epstein-Barr virus, Plummer-Vinsen syndrome, and chronic oral candidiasis may play a role in the disease. The human papillomavirus (HPV) also may play a role in the initiation of oral cancer.
One study estimated that 50 percent of oral cancers develop directly in the white patches of oral leukoplakia, and, in some others, the cancer may be "seeded" from leukoplakia lesions. In this study, about 24 percent of the dysplastic form of oral leukoplakia progressed to malignant cancers.
Symptoms
Signs of oral cancer include the following:
- Red, white, or discolored lesions in the mouth or on the lips
- Patches or lumps in or around the mouth that are painless in the early stages, but may become more painful as the malignancy spreads; those that bleed easily; or those that persist longer than two weeks
- A swelling, growth, or lump anywhere in or about the mouth or neck
- Swelling of the jaw that causes dentures to fit poorly or become uncomfortable
- Repeated bleeding from the mouth or throat
- Difficulty chewing, swallowing, or moving the tongue or jaw
- Pain in the ear
- Persistent hoarseness
Tissue changes in the mouth that might signal the beginnings of cancer often can be seen and felt easily:
- White papillary exophytic lesions
- Red velvety lesions
- Indurated growths
- An ulcer that does not heal
- Persistent pain or paresthesia
- An extraction site that does not heal.
Early detection and diagnosis
An oral cancer examination should be performed on every client. Steps on how to perform this exam can be found at www.tambcd.edu/oralexam/nidroc00.htm. In addition, we can teach patients, especially those at high risk, to perform this exam at home. If they find anything out of the ordinary - particularly anything that does not heal or go away in two weeks, or that has recently changed - they should be instructed to discuss it with a health professional.
New technology
The Fairfield DNA Ploidy System (see the list of resources) has been touted as a powerful predictor of the risk of oral cancer developing in patients with oral leukoplakia. Leukoplakia may resolve without ill effect, but in a number of cases may progress to oral cancer. Indi viduals were studied for a mean of almost nine years. Those with a normal amount of DNA per cell ("diploid") were found to be at a low risk of progression to cancer (only three out of 105 patients, or 3 percent, developed cancer), while white patches with abnormal amounts of DNA ("aneuploid") were at a high risk (21 out of 25 patients, or 84 percent, developed cancer in an average of 35 months). The study found that 20 patients fell into a third group, with double the normal amount of DNA per cell ("tetraploid"). These patients were at an intermediate risk of progression (12 out of 20 patients, or 60 percent, developed cancer). Cumulatively, those with the low-risk diploid lesions had a 97 percent survival rate, compared with 16 percent in the high-risk group and 40 percent in the intermediate group.
In an editorial commentary in the New England Journal of Medicine, written by individuals from the MD Anderson Cancer Center, University of Texas, Houston, the study of this system was described as an important advance in the molecular assessment of the risk of oral cancer in patients with leukoplakia.
The Fairfield Ploidy System may be useful in deciding which cases of leukoplakia require "watchful waiting" or more aggressive treatment, particularly since there are no other reliable methods to predict which patients will progress to cancer. Leukoplakia is particularly amenable to early detection by self-examination or in routine oral examinations.
An in-office test, the OralCDxRegistered, is a transepithelial oral biopsy to assist in the detection of oral cancer in the early, more curable stages. It may be used to test any lesion, without an obvious etiology, with epithelial abnormality, including red, white, mixed, ulcerated, thickened, traumatized, or irritated lesions. However, those of fibrous connective tissue origin or nodular elevated lesions, such as papillomas, fibromas, pyogenic granulomas, salivary gland tumors, or cysts would not benefit from this test.
The test is administered by brushing the lesion with the OralCDxRegistered brush biopsy instrument, being sure to apply pressure to reach all three epithelial layers. The cellular sample is then rolled onto a glass slide and sent to the laboratory for analysis.
According to The Council on Scientific Affairs of the American Dental Association, "persistent lesions, even with negative results, must receive adequate follow-up evaluations." OralCDxRegistered atypical or positive results require a scalpel biopsy.
In a recent "Letter to the Editor" in the Journal of the American Dental Association, five oral and maxillofacial surgeons and pathologists criticized the test. According to the authors, because mucosal abnormalities are clinically recognizable, a scalpel biopsy should be done immediately. The authors state: "Fear of performing a scalpel biopsy, or inadequate training in its performance, should not be construed as an indication to perform other tests that will further delay completion of the definitive diagnostic test." They also argue that the test delays definitive diagnosis.
In a perfect world, all dentists would immediately biopsy (or refer) all lesions of unknown origin. However, many dentists will "watch" lesions rather than performing a biopsy.
This dilemma is compounded by the fact that it is impossible to tell a benign lesion from early cancer or precancer simply by looking at it. Clearly, the brush biopsy is intended to test benign-looking lesions, and the scalpel biopsy is required for suspicious lesions. Each has its place. Client fear also weighs into the decision about whether to biopsy with a brush or a scalpel. While a scalpel biopsy may be preferable because it yields a histopathologic diagnosis, a brush biopsy has its place in a general office for lesions that are benign in appearance and have been monitored in the past. For these types of lesions, a later diagnosis is better than no diagnosis at all.
A new product by Zila Professional Pharma ceuticals, a division of Zila, Inc., is the ViziLitetrademark chemiluminescent oral examination device. The ViziLitetrademark device is used in conjunction with a conventional, visual, oral mucosal examination to improve the identification, evaluation, and monitoring of oral mucosal abnormalities in those at increased risk of oral cancer. The ViziLitetrademark test kit includes a hand-held, disposable, chemiluminescent light and a 1 percent acetic mouthrinse that work together to help dental professionals detect abnormalities in the oral cavity that might not be visible to the unaided eye.
Oral health-care professionals should be responsible for tobacco risk management by educating patients as well as detecting and treating related disease. Using the ViziLitetrademark device with a mirror or intraoral camera, the oral health-care professional can involve the client in the oral exam, with both parties looking for lesions that appear bright white under illumination. The ViziLitetrademark has the potential to enhance the quality of the oral exam.
Treatment
Oral hygiene is extremely important in reducing the incidence and severity of cancer treatment consequences, which may include radiation caries, stomatitis, xerostomia, and candidiasis. Oral-care procedures should include the following:
- Gentle cleaning (with a very soft toothbrush)
- Moisturizing the lips and oral cavity
- Saliva substitutes
- Methods to alleviate pain and inflammation.
Chlorhexidine rinses are helpful, but avoid mouthrinses containing alcohol. Moisturizing can be achieved with water-soluble lubricating gels and pain reduction by a topical anesthetic. Coating agents (such as milk of magnesia) mixed with a topical anesthetic (such as dyclonine or lidocaine) may be very helpful in controlling pain. Products containing ingredients that are hygroscopic (take up and retain moisture), such as glycerin, must be used with care. Some of the additives in local anesthetics might intensify and prolong mucositis.
Fifteen to 40 percent of cancer patients develop problems with nutrition early in the course of their illness, and more than 50 percent of patients undergoing cancer treatment experience substantial weight loss. An interdisciplinary team approach to postoperative and nutritional care should include a psychological assessment, support, and education for the patient and family. Depression and anxiety are common symptoms in patients with cancer.
As oral health-care providers, it is our responsibility to educate clients in the prevention of oral and pharyngeal cancer. Tobacco cessation is part of this process. Early diagnosis of lesions is critical to ensure timely and, perhaps, life-saving treatment. Treatment regimens may induce oral manifestations; consequently, being familiar with various products that alleviate pain and treat xerostomia may provide a better quality of life for patients.
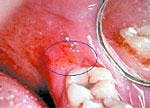
Ulcerative Lesions
ORAL CANCER LESIONS
null
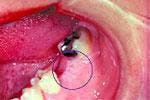
White lesions
null
null
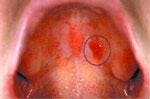
Red Lesions
null
Photos reprinted by permission of CDx Laboratories, Inc.
Oral cancer resources
- "Oral Health in Cancer Therapy: A Guide for Health-Care Professionals," (888) 443-2439 - DOEP Projects
- Fairfield Imaging Ltd., a UK-based biomedical company, part of the Medical Solutions group, develops, manufactures, and markets digital imaging solutions for pathologists
- www.tonguecancer.com - American Oral Cancer Clinic - Listings of specific oral and pharyngeal cancers
- www3.cancer.org - American Cancer Society - "All About Oral Cavity and Oropharyngeal Cancer"
- www.cancer.gov - National Cancer Institute: "What You Need To Know Abouttrademark Oral Cancer"
- www.tambcd.edu/oralexam/nidroc00.htm - "Detecting Oral Cancer," NIH, NIDCR, Baylor College of Dentistry
- www.tambcd.edu/oralexam/nidroc05.htm - "Routine Head & Neck Exam Tutorial"
- www.nohic.nidcr.nih.gov/publinks.html - National Oral Health Information Clearinghouse: Special Care Publications
- "Detecting Oral Cancer"
- "Dry Mouth"
- "Oral Health, Cancer Care, and You"
- "What You Need to Know About Oral Cancer"
- Various tobacco publications
- www.nidcr.nih.gov/Spectrum/NIDCR3/3menu.htm - "Oral Cancer: Confronting the Enemy" - NIDCR Spectrum Series
- www.oralscan.com - Oral CDxRegistered
- www.oralscan.com/dentists/index.htm - "Step-by-Step and Clinical Lesion Guide"
- www.laclede.com - Dry mouth products
- www.nospit.com/ResGuide.pdf - "Oral Cancer Resource Guide"
- www.doep.org/TFacts.pdf - "Tobacco Facts for the Clinician"