Obtaining optimum retention for tooth restorations
Each month, Dr. Gordon Christensen answers a question from readers about everyday dentistry.
Q: During the last few years, I have had numerous crowns come off, composites loosen, and buildups release from the remaining tooth structure. I have been using the currently advertised bonding agents exactly as manufacturers recommend, but apparently the bonds are still failing. What can I do to prevent these frustrating failures? They are upsetting to both me and my patients.
A: I hear this question frequently, and I have some potential solutions for you. As you know, there are major basic types of retention for dental restorations.
More from the author ... Comparing new vs. older dental concepts
Mechanical interlocking retention requires irregularities in the remaining tooth structure into which the cement, composite, or buildup material can flow. The resultant interlocking of the tooth and the material placed on the irregular surface creates a physical impediment to the material coming off, and that interlocking is highly retentive over the long term. Mechanical retention for dental materials is not unlike the placement of bricks on the outside of a building. Bricks placed on the building surface are retained by semi-liquid mortar that flows into the rough brick surface and the roughness of the building’s internal wall. The mortar sets to a rigid mass and the bricks are then held solidly in place.
Chemical retention is molecular contact at the surface of the substrate—tooth structure. It is the strongest mechanism of adhesion, with bonds occurring between functional groups in the adhesive and atoms/molecules on the substrate surface. This mechanism contributes to the structural strength of many adhesives, including dental bonding agents. If the expansion-contraction coefficient of the two substrates is equal, there is minimal reduction in bonding strength. Such is not the case with some dental bonding techniques, including resin-based composite bonding to tooth structure. These materials placed over tooth structure have expansion-contraction characteristics different from that of tooth structure. Hot and cold foods cause retention stress and depreciation of this chemical bond.
Difference between enamel and dentin bonding
Enamel is acid-etched, creating thousands of potentially interlocking irregularities into which the dental resin-based composite can flow. These irregularities create strong, long-term mechanical retention. This does not happen with dentin. The dentinal canals are extremely small—just a few microns in diameter. Contact of the composite and the tooth with hot and cold foods along with the inequal expansion-contraction of dentin and composite resin soon depreciate the initial bond.
More from the author ... Why should teeth be removed?
When a significant percentage of the tooth prep has enamel on it, the resin cannot come off due to the mechanical retention provided by acid-etching. If the prep is mainly dentin, the dentin-composite chemical bond is soon reduced, and the resin restoration or cement can come off.
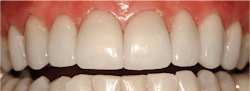
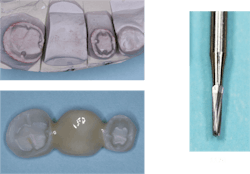
A well-known clinical situation demonstrates this phenomenon. Veneers placed on enamel must be cut off regardless of the time they have been in the mouth, while veneers placed primarily on dentin can often be removed with slight force applied to them after only a few months (figure 1).
Creating optimum retention for tooth preps mostly on dentin
Any tooth preparation cut primarily on dentin requires mechanical retention. These methods can create mechanical retention:
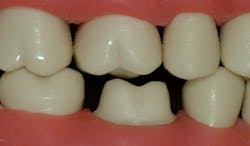
Optimum tooth preparation characteristics can provide acceptable retention for both direct and indirect restorations. It is common knowledge that an ideal crown preparation should be at least 4 mm long from the cervical margin to the occlusal table, with 20 degrees or less lack of parallelism of the axial walls (figure 2). An optimum tooth preparation for a direct restoration must be undercut on much of the tooth preparation to provide mechanical resistance from dislodgement. What if these characteristics cannot be provided when making a conventional tooth preparation? The following procedures will augment these situations by providing more mechanical retention.
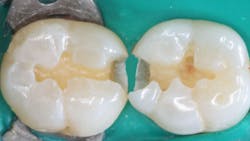
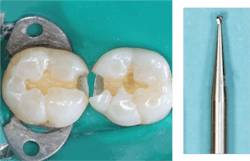
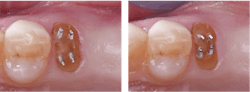
Undercuts in the prep, either natural undercuts or those made with rotary instruments. Proximal box forms in class II restorations usually have a small amount of enamel on the facial and lingual surfaces of the box, creating some mechanical retention after etching the prep. However, the deeper the box form, the less enamel is present. Usually, mechanical retention should be placed with a small round bur (1/2 or 1/4) at the facial and lingual axial juncture of the internal cervical dentin box (figure 3). Failure to do this often causes the composite to come loose in the proximal box.
Irregular surfaces on the prep made with a coarse rotary diamond. This procedure is especially important for indirect restoration preps that are too short, too tapered, or both. Mandibular second molars often have these challenges. During the seating appointment, roughen the surfaces on all the axial walls of the prep and preferably on the intaglio surface of the crown to be cemented. This procedure is appropriate for any situation where the crown prep does not have adequate parallelism or is too short, and certainly for cementation of zirconia crowns that have come loose in service.
Grooves perpendicular to the occlusal plane made on the axial surfaces of preps for crowns. These grooves can be made on short or overly tapered crown preps to increase retention. They are made parallel to one another with tapered burs such as a 1170 or 1171 or similar-shaped diamonds (figure 4). Advise the lab technician to make the crown fit into all the grooves. Some technicians don’t do this, which eliminates the value of the grooves.
Grooves horizontal to the occlusal plane. In clinical situations requiring optimum retention of a short crown, an abutment on a long-span fixed prosthesis, or cementation of a crown that has come off in service, shallow (1/2 mm deep) horizontal grooves can be made on the facial and lingual surfaces of the prep at the seating appointment.
Undercut “potholes” with a small-diameter bur. When amalgam was popular, this procedure was used as one of the primary retentive features for large restorations or buildups. It can also be applied for large composite restorations or buildups. Pear-shaped rotary instruments, such as 330 or 245 burs, can create undercut potholes about 1 mm deep. When the composite material is adequately placed in the holes, significant retention is obtained.
Retentive pins placed into dentin. To my dismay and probably because of overly optimistic acceptance of bonding agents on dentin, many dentists do not place retentive pins. I would be severely handicapped in some situations if I didn’t have retentive pins, especially when more than half of the coronal portion of the tooth is gone. Properly placed pins provide optimum retention of buildup material or large direct restorations. There are three major types of retentive pins: stainless steel, titanium alloy, and pure titanium. The type least likely to make cracks in the dentin is pure titanium, which adapts better to the dentin as the pin is screwed into the tooth. (Examples include Filpin or Nordin.) Pins should be placed at least 15 degrees parallel to the long axis of the tooth, 2 mm deep, and then bent over toward the center of the tooth to be incorporated into the planned restoration material (figure 5).
Summary
Mechanical retention provided by the methods described in this article is essential for many clinical situations since conventional bonding agents provide initial bond to dentin but not long-term retention.
Author’s note: These educational materials from Practical Clinical Courses offer further resources.
One-hour videos:
- Strong, Comfortable, Esthetic Rehabilitations with Zirconia (Item #V1942)
- Foolproof, Fast Single-Crown Restoration (Item #V1980)
Two-day hands-on courses in Utah:
- Faster, Easier, Higher Quality Dentistry with Dr. Gordon Christensen
- Restorative, Esthetic, Preventive Dentistry with Dr. Gordon Christensen
- Simplifying Complex Treatment with Dr. Gordon Christensen
For more information, visit Practical Clinical Courses or call (800) 223-6569.
Editor's note: This article appeared in the January 2024 print edition of Dental Economics magazine. Dentists in North America are eligible for a complimentary print subscription. Sign up here.
Gordon J. Christensen, DDS, PhD, MSD, is a practicing prosthodontist in Provo, Utah. He is the founder and CEO of Practical Clinical Courses, an international continuing education organization founded in 1981 for dental professionals. Dr. Christensen is cofounder (with his wife, Rella Christensen, PhD, RDH) and CEO of Clinicians Report.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.