Implants made easy
by August De Oliveira, DDS
Dental implants are all the rage these days. Simply stroll through any dental convention and you'll see booth after booth selling everything from the fixtures themselves to grafting supplies and CBCT scanners.
Why the sudden surge in popularity? Implants have a long track record of success, so why are they now stealing the spotlight from veneers and lasers?
According to a study done by Straumann (Straumann CBC 2012: "How will dentistry look in 2020?"), the U.S. ranked fifth behind countries such as Germany and Japan in total implant placement. Why is this?
Even in countries with socialized health care, more implants are placed than in the U.S. In my opinion, the answer lies in the number of general dentists placing implants. According to a 2007 study printed in JADA, only 12% of all GPs surgically placed implants, and of those, the average number of implants placed per year was 32.4.
Whenever I treatment plan a patient, I ask myself, "Could a specialist do a better job?" If the answer is yes, then I send the patient on his or her way with a referral card. I don't extract impacted thirds. I don't do a lot of re-treats. I don't perform orthodontics or manage advanced periodontal disease. Why? Because I have a team of specialists that can offer patients better care in these areas. I feel the same way about implants. I still refer out some implant cases. I do not do sinus lifts or extensive grafting. However, since I know what I can and can't tackle, my specialists are seeing many more referrals from my office than ever before. It is my opinion that general dentists, with the proper hands-on training, should be able to treat the "easy" implant cases and refer out the more complex cases. Many dentists treat only single root endodontics and refer out molars. I think the same "triage" should apply to implants.
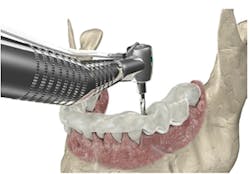
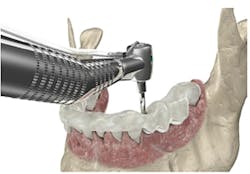
With the dawn of CBCT use and guided surgery (Fig. 1), it is far easier for general dentists to place implants safely as well as make the decision of which cases to treat and which to refer. Although some may disagree that all dentists need to know how to place implants, I don't think any could argue about the benefits of this modality. With a cone beam scan, doctors can determine the buccolingual width of the ridge, the proximity of anatomy, and the quality of bone. These variables were elusive in our limited 2-D scans.
I wrote the book, "Implants Made Easy," to show general dentists what constituted an easy implant case, and to give dentists a stepping-stone for further education. After taking an extensive hands-on live patient course, there is no reason why many dentists should not be able to tackle certain cases in good bone on healthy patients.
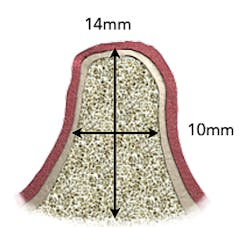
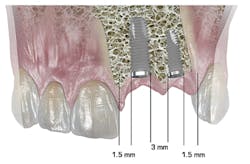
A good starting case would be a posterior implant with an edentulous space with at least 10 mm of bone buccolingually and a crest to a nerve, sinus, or floor of nose of at least 14 mm. These dimensions are easy to see in a CBCT scan, but 2-D images can be used along with "bone sounding," a technique of piercing the gingiva to assess the shape of bone along the ridge in order to get these values.
By being aware of certain guidelines in placing implants, a GP should be able to decide whether or not a case is within his or her ability. (Fig. 3)
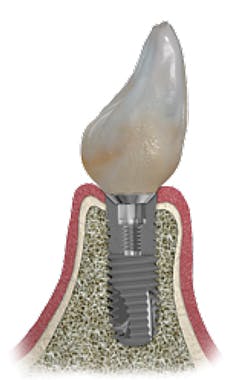
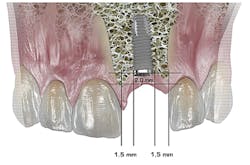
In the past, the general opinion was that an implant "was not a tooth," and although this is true, our patients seem to think otherwise. In my opinion, two principles make up a truly exceptional case, and these are managing the soft tissue and developing the crown's emergence profile. Although many factors add up to this, placing the implant platform at the correct height occluso-apically will go a long away in improving both hard and soft tissue esthetics. To get enough emergence profile "runway," the implant platform should be at least 2 mm to 3 mm apical to the adjacent teeth's CEJs.
However, one can overdo this. To develop a papilla between a natural tooth and an implant, the implant platform should be no deeper than 5 mm apical to the most cervical aspect of the adjacent teeth's contacts. (Fig. 5)
Many dentists state that they do not surgically place implants because they're afraid of the inferior alveolar nerve, and rightly so. However, knowing a bit about the characteristics of the nerve can help one avoid it.
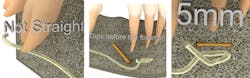
One misconception is that the nerve's course within the mandible is parallel to the buccal or the lingual. The nerve weaves from the lingual to the buccal, especially as it enters the mental foramen. (Fig. 6)
The nerve also moves up and down. The nerve will dip, on average, 2 mm prior to entering the foramen. (Fig. 7)
Finally, the nerve may extend mesially up to 5 mm past the mental foramen. In some cases the nerve may extend past the canine. (Fig. 8)
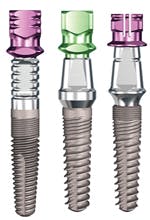
When choosing an implant system, it's important to know a bit about the implant you're placing. Some implants may be placed flush with the crest of the ridge. These have many names but are frequently called bone level implants (Fig. 9a). Some implants may have an extension that protrudes through the gingiva. These may be called tissue level implants (Fig. 9b). Implants may be roughened through various treatment processes or may be coated with substances such as hydroxyapatite crystals (Fig. 9b). Some implants may be called one-piece implants and may have attached to the platform a connection such as a locator, ERA, or GPS attachment (Fig. 9c). Some implants may come attached with an angled or straight abutment (Fig. 9d).
If one looks at the various styles of implants, one may be completely different from another. As implants and research on bone loss progresses, we see a number of trends. Implant threads get larger in the apex and center of the implants to grab on to the less dense trabecular bone. As the threads reach the platform of the implant, threads get finer to exert less stress on the crest of the ridge leading to less bone loss. Also, the use of a platform switching abutment is becoming more common. As the abutment attaches to the implant, a "notch" or neck allows for room for bone and gingiva to grow over the platform of the implant. (Fig. 10)
Also, as implants progress, we can see that the internal connection types are getting deeper. Early root form implants had less contact internally and some may even have an external bevel. As implants become engineered to reduce bone loss, the abutment/implant interface is being placed more medial and further inside of the implant. Lead-in bevels and conical connections provide a greater surface area between the abutment and the implant internally, leading to less micro movement and bone loss. (Fig. 11)
Implants are the fastest growing market in the dental industry. We all know that implants, in many cases, are the best, most conservative treatment for our patients. As more and more dentists get interested in implants and patients become more aware of this option, it becomes increasingly important that doctors know not only how to perform the surgery, but how to treatment plan. There is no replacement for in-depth, hands-on education and proper diagnostics. Dentists need to know which cases they can tackle and which to refer out.
Finally, knowing which implant to use and how to reduce bone loss is important. In my opinion, adding implants to your practice is one of the best things you can do for your patients!
August de Oliveira, DDS, began lecturing on 3-D technology in 2004, when he became a CEREC basic trainer. Since 2008 he's been involved with Implant Direct's R and D department. Dr. de Oliveira has written two books on implantology, and has been involved with beta testing Sirona's Sidexis program. He lectures nationwide for Sirona on the Galileos cone beam system and guided implant surgery, and teaches for Implant Direct at their Las Vegas facility. Dr. de Oliveira practices in L.A.
Past DE Issues