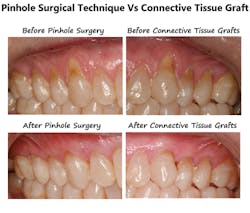
Pinhole Surgical Technique: Halting gingival recession in a single visit
Editor's note: This article, published in 2016, continues to be popular with readers. For a more recent look at PST, please read Pinhole Surgical Technique: A 10-year evaluation of root coverage, published in 2022.
As a periodontist, I see a lot of patients who have been aware of their gingival recession for several years, yet they have never followed through with treatment. Most patients with mucogingival defects have been referred to a periodontist at least once-and some may have even gone in for a consultation-but their fear of grafting prevented them from completing necessary treatment. Many patients have read or heard about others' horror stories involving horrifically painful experiences with soft-tissue grafting. These patients are so terrified that they would rather risk continued attachment loss-and potential tooth loss-than proceed with grafting.
I've even heard dentists and hygienists share the same notion that "gum grafting" is a terribly painful procedure; in fact, so much so that it should only be done when the patient becomes symptomatic or is at immediate risk of tooth loss. Unfortunately, by this time the defect may have become so severe that it requires multiple procedures with less-than-ideal results, more pain, and greater expense than if they had corrected the problem when it was first recognized-that is, if the tooth can be salvaged at all. Wouldn't you agree that the best time to intervene with most dental problems is when they are initially recognized?
The Pinhole Surgical Technique
Enter the Pinhole Surgical Technique (PST), a minimally invasive treatment option to reverse gingival recession without grafting or sutures. What is PST (also referred to as the Lunchtime Gum Lift or Pinhole Gum Rejuvenation)? It is a novel procedure that combines techniques from traditional periodontal surgical procedures, such as coronally positioned flaps and guided bone regeneration, to reverse gingival recession. A coronally positioned flap (CPF) is a technique that requires creating an incision in the sulcus and across the papillae of affected teeth, elevating a flap (either full or split thickness), pulling the flap coronally, and suturing it into place. These techniques are often combined with autogenous grafts, allografts (cadaver), or xenografts (animal).
PST procedure
Like a CPF, PST allows coronal positioning of the gingival margin to cover recession defects, but it is not done with the use of scalpels, periosteal elevators, or sutures. Instead, a small pinhole is created by piercing the mucosa apical to the mucogingival junction in the area of recession, and then inserting specialized instruments through that hole to elevate a full-thickness "flap" in an apico-coronal direction.
Once the periosteum is elevated from the underlying bone and tooth, it easily can be pushed coronally. But how does it stay in the new coronal position during the healing period without stitching? This is where I think the real genius of this procedure is-collagen strips! These collagen strips are actually pieces of a resorbable collagen membrane called Bio-Gide (Geistlich Biomaterials), which has been used for decades in periodontics for periodontal regeneration-just not in this same way.
With PST, the collagen membrane is cut into strips and placed through the pinhole that was used to elevate the periosteum. The strips are then pushed under the gingiva into the interproximal spaces, covering the facial surfaces of the previously exposed roots. And violà! The tissue is supported at the new position, and the strips assist in wound stabilization during healing to ensure root coverage.
Limitations
Like conventional grafting, there are limitations to the success of PST for reversing gingival recession. For example, root coverage is less predictable in areas of advanced bone loss due to a lack of bone support for the newly positioned tissue. Additionally, the patient must be free of inflammation and active periodontal disease at the time of surgery, compliant with postoperative instructions, and cease any traumatic activities that may have contributed to the recession, such as aggressive brushing. It is also recommended that the patient wear an appliance to protect from bruxism-induced occlusal trauma when indicated.
Advantages
A major advantage of PST compared to traditional autogenous grafting (connective tissue grafting) is the ability to treat as many teeth in one sitting as the patient desires. When using the patients' own tissue, there are inherent limitations in the number and size of the area that can be treated at one time. It is not uncommon to take over a year to treat an entire mouth, requiring multiple rounds of palatal grafting. In contrast, PST can be used to treat the whole mouth and be completed in a single sitting. Additional advantages include significantly less chair time than conventional procedures, better patient acceptance, less postoperative pain, decreased risk of postoperative trismus, and even fewer insurance restrictions.
Research
A common question concerns long-term stability of the results. The only peer-reviewed study thus far was featured in the International Journal of Periodontics & Restorative Dentistry in 2012.1 The study demonstrated the stability of PST results over a period of nine years, although John Chao, DDS, MAGD-the inventor of PST-has cases that are even older and still holding strong. (Visit pinholesurgicaltechnique.com to see examples.) Like most other treatment options for reversing gingival recession, the key to longevity lies in patient education and compliance.
If you're interested in learning more about PST, Dr. Chao's Pinhole Academy offers free live webinars to further discuss the procedure and answer questions.
Reference
1. Chao J. A novel approach to root coverage: the pinhole surgical technique. Int J Periodontics Restorative Dent. 2012;32(5):521-531.
About the Author
Tina Beck, DDS, MS
Tina Beck, DDS, MS, is a diplomate of the American Board of Periodontology, has been recognized locally and nationally for her leadership activities in organized dentistry, is an active contributor to many online and printed publications, and is the owner and solo practitioner of Southern California Periodontics & Implantology in San Diego, California.