Converting to the Imetric system: All-digital, model-free hybrids
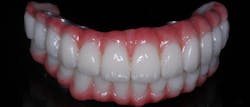
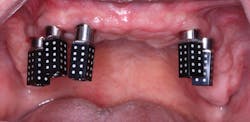
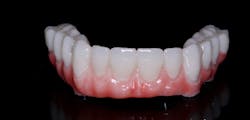
BEFORE I HAD RESTORED a lot of dental implant cases, I had always thought, “Taking an impression for an implant restoration must be so easy!” There was no cord packing, no tooth prepping; just screw in an impression coping, and off you go. While this is true with most single-unit posterior cases, the longer I practice, the more I realize that getting a good implant restoration from a polyvinyl siloxane (PVS) impression can be tough. First, you need to make sure the parts involved are actually seated. Then, you need to cope with the inaccuracies that are caused by the impression material or the lab inserting the analogs incorrectly. When we first started using scan bodies (3Shape), I jumped on the bandwagon. The difficulty multiplies exponentially when dealing with multiple splinted implants, which is what we see in hybrid cases (figure 1).
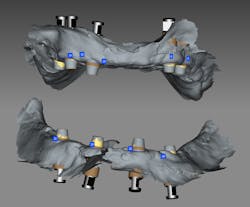
Using naive logic, one would think scanning for a hybrid is pretty easy, right? Just screw in scan bodies and you are off to the races. Well, hold up! As many digital dentists know, the more images you take, the less accurate the scan. This is due to the fact that, like a panoramic picture, an intraoral scan is really made up of multiple images that are “stitched,” using common overlapping data. This mathematical extrapolation introduces slight error that can add up with the number of images you need to take for a full-arch scan. Searching the literature for real numbers on the accuracy of full-arch intraoral scans on edentulous cases is like finding a needle in a haystack, in spite of the growing number of intraoral scanners on the market (figure 2).
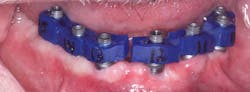
Currently, the gold standard for restoring implants is to lute together impression jigs via a process called a corrected cast. This process involves taking an initial inaccurate impression, making jigs and a custom tray, and then repouring the model or cutting out analogs to make up for the inaccuracies of regular impression copings and a stock tray (figure 3).
This model can have scan bodies inserted and scanned with a lab scanner. You may be wondering why a lab scanner is more accurate than an intraoral scanner. There are two reasons. First, there is no saliva and no patient movement in a lab scanner. The model and the scanning camera are fixed or may rotate, but there is no wiggling. Second, a lab scanner needs fewer images than an intraoral scanner as it captures more data per shot. Enter photogrammetry. With photogrammetric scanners, scan bodies that look like dominoes are captured with extraoral images taken with a scanner. In this case, we used the Imetric 4D scanner (figure 4).
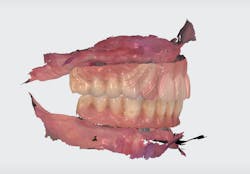
Three separate scans were taken of this patient. First, as with anything we do in dentistry, we have to establish the bite. This was achieved with a pre-op scan with the patient wearing his converted denture. Next, after removing the converted denture, healing abutments were screwed into the multiunit abutments and a soft-tissue scan was taken. Finally, the Imetric 4D scan bodies were screwed in and an extraoral scan was taken. These three scans were then combined and exported to Exocad, a powerful lab-based CAD/CAM software (figure 5).
Once a month, I volunteer at a clinic in Phoenix called Brighterway, where we provide dentistry to the homeless as well as low-income veterans and their families. A number of companies have donated high-tech toys for me to play with, including Trios intraoral scanners (3Shape), a Carbon 3-D printer, a Ceramill CAD/CAM system (Amann Girrbach), and the Imetric 4D scanner.
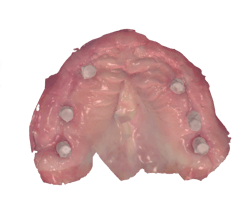
In this case, we had a veteran with implants placed in an All-on-4 arrangement and a converted hybrid denture on multiunit abutments. The implant positions were captured using domino-like scan bodies, and the soft tissue was scanned with a Trios scan. The patient’s bite was established by scanning the converted denture intraorally (figures 6 and 7).
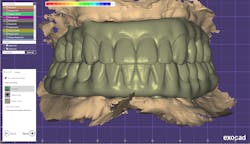
In Exocad, Burbank Dental Lab designed the hybrids (figure 8).
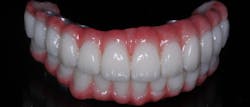
In this case, we used a polymethyl methacrylate (PMMA) acrylic hybrid that the patient will wear for a few months to verify occlusion, phonetics, esthetics, and cleansability. Once we are all happy, the final can be milled in zirconia or with an enhanced polymer, such as Pekkton (Anaxdent), with IPS e.max crowns (Ivoclar Vivadent) for the individual teeth. Gingival composite was layered on the PMMA, and the teeth were stained and glazed with an acrylic glaze (figure 9).
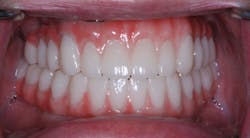
Three things blew me away with this case. First, the fit was completely passive. We do something with hybrids called the Sheffield test. One screw is tightened on one implant, and pressure is applied to the contralateral side to see if there is rocking. Although our previous hybrids passed this test, they felt tighter than the hybrids made using the corrected cast. Second was the occlusion. No occlusal adjustment was needed in this case. Finally, we were all thrilled with the esthetics (figure 10). Using Imetric and Trios scans is going to be our standard protocol going forward at the Brighterway clinic.
About the Author
August de Oliveira, DDS
AUGUST de OLIVEIRA, DDS, graduated from the University of Washington School of Dentistry in 1997 and completed his general practice residency in Los Angeles in 1998. He has written three books: Implants Made Easy, Guided Implantology Made Easy, and Dental 3D Printing Made Easy. Dr. de Oliveira lectures for several dental companies, including Implant Direct and Dentsply Sirona. He lives and practices in Los Angeles, California.