The changing reality of implant dentistry
by Gerald A. Niznick, DMD, MSD
Editor’s Note: This is the first of a four-part article covering the past, present, and future of dental implants and their impact on the practice of general dentistry. The first installment discusses the history and evolution of the modern dental implant.
Advances in dental implant technology and increased public awareness have created greater possibilities for general dentists to expand their practices by placing dental implants. Today, many general dentists are realizing that dental implants are an integral part of conventional dentistry and can be offered successfully with a minimum investment of time and money. In this challenging economic environment, as patients encounter financial hardships that limit their discretionary spending, more GPs are realizing the importance of broadening the range of services they are able to offer to the diminishing number of patients with discretionary income.
There are major differences in the cost of dental implants and abutments to GPs versus surgical specialist. The largest implant companies sustain high prices for GPs ordering implants and abutments on a per-patient basis, while discounting heavily to surgical specialists buying in volume. Dentists need to evaluate their options with at least the same degree of diligence as they apply to buying a new car. Understanding the features, benefits, cost, and support offered with each implant system is important in making an informed decision.
Dentists should begin by selecting the system, then taking the training on that system with a focus on learning how to do the simplest and most predictable applications. These include single-tooth replacement in an extraction socket, and stabilizing a lower denture with two to three implants in the symphysis. Once you can do these procedures, it is a small step to being able to offer teeth-in-one-day procedures and more complex fixed restorations on multiple implants. Organized implant dentistry dates back to the mid-1960s with the start of the American Academy of Implant Dentistry. The popular implants in the 1960s and 1970s were subperiosteal and blade implants. Subperiosteal implants got their name because they consisted of a cast chrome frame made by reflecting the tissue on an edentulous jaw in order to make a bone impression.
A second surgery was required to seat the frame, with the reflected periosteum reattaching through the openings in the frame, locking it in position. Four posts projected through the gingiva to provide support for an overdenture. This procedure was technique-sensitive because it required an extensive impression. The blade implant, made from titanium, was placed in a slot in the ridge using high speed drills. The blade would then be tapped into place, wedging it between the buccal and lingual plates of bone to achieve initial stability. A post projecting through the tissue could be bent to create parallelism with other blade implants or with preparations on adjacent natural teeth. The implant(s) and natural teeth were splinted with a cemented temporary bridge and put into immediate function.
Soft-tissue encapsulation often resulted around the blade, and failure could not be detected until extensive bone loss had occurred. There were some one-piece screw implants available in the 1970s but they were not very popular because of limited applications without the ability to angle or prepare the abutment post.
Straumann introduced an endosseous, hollow-basket, one-piece implant in the late 1970s that also did not allow for angulation or preparation of the post. The post projecting through the tissue was narrower than the body, resulting in an infrabony defect at time of implant placement that encouraged down-growth of epithelium. Straumann’s basket-and-screw titanium implants had a textured surface created by plasma-spraying titanium. This additive process could create a soft-tissue problem if the rough surface became exposed to the soft tissue. By 1980, after a decade of experience with the implant systems described above, I had become disenchanted with their lack of predictability. Necessity being the mother of invention, I focused my attention on solving my most troubling clinical problem as a prosthodontist — stabilizing a lower removable denture.
In 1982, I launched the Core-Vent system and received patents on the implant design and an overdenture attachment that allowed for vertical and rotational movement to reduce the stress on the free-standing implants. It was a radical concept at the time. Today, the American College of Prosthodontists considers this a minimum standard of care.
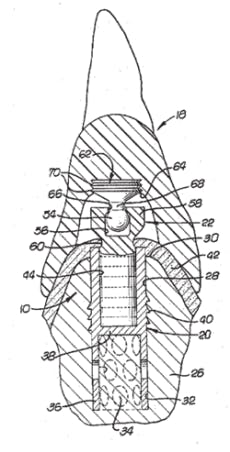
The Core-Vent implant was made of medical grade titanium alloy for strength, and had a medium rough surface created by blasting and etching for increased bone attachment. Its design included a hollow-basket apical end with external threads in the upper half that maintained the same diameter throughout. The Core-Vent had an internal hex hole for ratcheting to place. The implant was designed to be buried under the soft tissue for a three-to-four month unloaded healing period, after which the top was exposed and an abutment cemented into the hex hole. The Core-Vent system introduced the concept of implant prosthodontics to the dental profession by providing a variety of abutment posts, selected for specific clinical applications.
In 1983, the Journal of Prosthetic Dentistry published a series of papers on the Swedish Branemark system that had been presented at a 1982 University of Toronto conference. The conference was restricted by invitation only to academicians from throughout North America. The articles documented the use of the Branemark external-hex, internally threaded implant in Sweden, dating back to the late 1960s.
The system offered a single screw-receiving abutment for fixed detachable restorations in totally edentulous jaws. Four to six implants were placed in the anterior and splinted together with cantilever extensions distally.
The Branemark implant differed from the Core-Vent in several significant ways. It was made of pure titanium, which was weaker than Core-Vent’s titanium alloy, resulting in increased risk of fracture. Its machined surface was relatively smooth without blasting, acid etching, or TPS coating to create additional surface texture.
The Branemark system initially targeted oral surgeons and prosthodontists, requiring teams to attend a three-day university-sponsored training course with surgical placement restricted to operating in a totally sterile environment. The Core-Vent system, on the other hand, was taught to all dentists in readily available and affordable one- and two-day courses.
The team approach to implant dentistry has proven successful in North America, but in Europe it is the exception rather than the norm. Many GPs have proven over the last three decades that they can provide a high quality service to their patients by both placing and restoring dental implants.
Some have taken extensive training in bone grafting procedures and have demonstrated proficiency in more complex cases. Image-guided surgery is shortening the learning curve for placement of implants. General dentists are limited only by their commitment to education and their willingness to expand their horizons with new technology.
In 1986, Core-Vent launched the Screw-Vent System, and in 1999 offered this implant in a tapered version. Twenty-four years after the Screw-Vent was introduced, it is the mainstay of the Zimmer Dental product line, acquired with its purchase of Core-Vent Corporation’s assets in 2001. The Screw-Vent introduced the concept of an internal connection, combining a wrench-engaging surface with internal threads in the same internal shaft (Niznick US Pat. #3,960,381). The internal connection solved the loose screw problems that plagued external hex implants and allowed narrower designs, expanding the clinical applications of dental implants. It provided greater tactile sense when seating an abutment, eliminating the need to take X-rays to confirm full seating.
Over the years, the prosthetic options for internal connection implants have expanded, increasing both functionality and esthetics. This connection has become the cornerstone of modern implant design, licensed to a number of companies including BioHorizons, 3i, Straumann, and Friadent.
A number of foreign companies in countries such as Brazil, Israel, Italy, and Korea, where the patent was never filed, copied the Screw-Vent’s lead-in bevel and internal hex connection and are now able to sell in the U.S. as the patent expired in 2007. In 2008, Nobel launched the NobelActive implant with an internal bevel and internal hex, referring to it as the “implant of the future.” Implant Direct launched its Legacy system in 2007 and expanded it to include the Legacy3 in 2009. Legacy3 in 6 diameters, with all-in-one packaging, includes a cover screw, healing collar, transfer, and preparable abutment. It has progressively deeper body threads and micro-threads near the top for increased initial stability. As shown at left, it offers color-coded platforms for simplified product identification.
Dr. Gerald Niznick graduated from the University of Manitoba Dental School in 1966 and then earned a master’s degree in prosthodontics at Indiana University in 1968. He has been awarded 36 U.S. patents and received honorary doctorate degrees. Reach him at [email protected].