Incorporating LAAs into perio therapy
Do you ever wonder if you could provide better treatment options for your periodontal patients and increase your revenue at the same time? Local delivery of antimicrobials/antibiotics, or LAA, may be an option for you to incorporate into your practice. With the first introduction of Acticite® in the 1990s, local delivery products are now considered a fast, easy, and effective treatment for the reduction of periodontal pockets. Products on the U.S. market include the chlorhexidine chip (PerioChip®; Omni Pharmaceuticals, West Palm Beach, Fla.), doxycycline gel (Atridox™; CollaGenex Pharmaceuticals Inc., Newtown, Pa.) and minocycline HCl 1 mg microspheres (Arestin®; OraPharma Inc., Warminster, Pa). These newer products have certain advantages. They are biodegradable, bioadhesive, and cost-effective to the patient. Can the use of these products also help you generate revenue in your practice? Let’s discuss the benefits.
Why use local delivery of antimicrobials/antibiotics?
LAA delivers a potent dose of an antimicrobial or antibiotic into the periodontal pocket. There are several reasons why LAA are beneficial.
▲ Mechanical therapy by scaling the tooth and roots does not remove all of the plaque bacteria (now called biofilm) from the tooth surfaces. Even a highly skilled dentist or dental hygienist cannot remove it all. Although hand scaling or the use of power instrumentation is necessary to break up the biofilm, placing LAA in the pocket will help kill or suppress the remaining bacteria.
▲ Periodontitis is now considered a chronic disease. You and your staff need to tell this fact to your patients. It cannot be cured, but it can be controlled - maybe. After you scale your patients, research shows that bacterial levels start to reach prescaling levels within 8 to 11 weeks. Unless your patient is on a two-month recare schedule, those bacteria are partying long before the patient returns to see you. LAA release the drug at high levels for 7 to 21 days (depending on the product) to kill most of the bacteria we want to eradicate. This gives the pocket an extra “boost” until recare treatment.
▲ Patients are concerned about the overuse of systemic antibiotics. LAA can provide a high level of drug to a specific site or sites without the drug being distributed throughout the body. Also, you don’t have to worry about the patient complying with daily pill-taking.
▲LAAs are easy to use. For example, Arestin (minocycline HCl 1 mg) is premeasured and can be placed in several pockets in a few minutes. It releases a high dose of antibiotic for 14 to 21 days to achieve improved pocket depth reduction over scaling and root-planing (SRP) alone. Also, it is legal in most states for dental hygienists to perform so it can easily be incorporated into the SRP appointment.
Who should be treated with LAAs?
First, many offices are not thoroughly probing and performing a comprehensive periodontal examination on each patient. The result is that millions of Americans are walking around with undiagnosed periodontal disease and an active infection! With all of the recent press about the possible link between periodontal disease and systemic disease, patients are very interested in knowing about their condition. In addition, chronic periodontitis can cause bad breath and poor esthetic results. All patients have a right to know their condition. The keys to effective treatment are diagnosing the disease and telling your patients in layman’s terms.
Any patient with moderate chronic periodontitis and pocket depths ≥5 mm with bleeding is a candidate for LAA. Perform a complete medical history on each patient. Next, determine if the patient is allergic or has sensitivities to the tetracycline class of drugs. Atridox and Arestin are derivatives of tetracycline, and PerioChip contains chlorhexidine. A comprehensive periodontal examination (code CPE) D0180 is required to diagnose the patient’s current periodontal condition. This examination includes full-mouth probing, clinical attachment levels/recession, furcation involvement, mobility, occlusal assessment, and a full-mouth X-ray series if needed. Once the patient has been evaluated and diagnosed, he or she should be provided with a thorough explanation including all treatment options. LAA have been found to be an effective treatment regimen and should be one of the therapeutic options discussed and offered to patients.
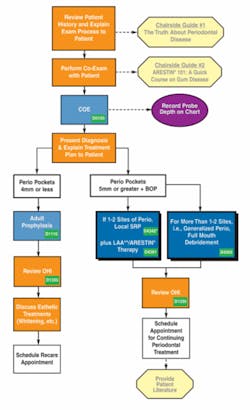
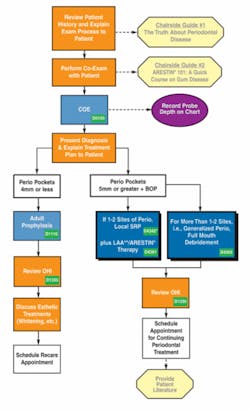
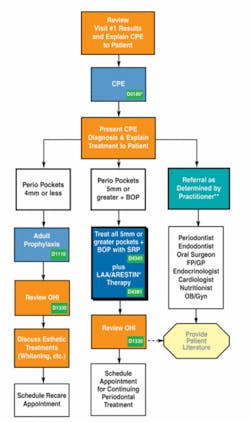
What about the rest of the treatment sequence? Although much has been written about the science behind LAA therapy, little has been written about how to implement it into the dental practice. OraPharma, Inc. (Arestin) has published “Periodontal Treatment Protocol” to guide dentists and their teams in the use of LAAs. The protocol includes appointment sequences with insurance codes, brochures for patients, forms for office use, and verbal skill suggestions. Figures 1 through 3 display treatment sequences and protocols borrowed from the Periodontal Treatment Protocol.
Increasing practice revenue with LAA
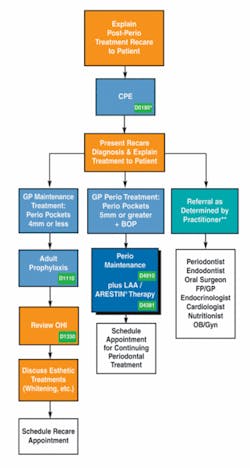
In my seminars on nonsurgical periodontal therapy, many dentists and hygienists approach me about the way their offices deal with periodontal patients. If what they are telling me is true, many offices are not charging appropriate fees for treatment, and they are not coding truthfully. For example, many periodontal patients are being charged and coded adult prophylaxis fees. In addition, many offices do not offer therapeutic treatments such as LAA therapy because they fear their patients will reject it because of cost. Figure 4 lists the current billing codes that should be applied according to the patient’s condition. If these codes alone were applied appropriately, office revenue would increase; but the use of LAAs can increase the revenues even more. Following are three ways to make it happen -
1. Talk to the patient. Assume that the patient wants to know about his or her condition and they want to know about all treatment options. Are you knowledgeable about current procedures for periodontal care such as advanced hand and power instrumentation, use of chemotherapeutics, current evidence about biofilm formation and control, and local and systemic antibiotics? Have you read about the oral-systemic links and are you able to answer patients’ questions about periodontal disease? Why am I asking this? Because if you do not believe in the therapies you are proposing to your patients, they will sense it and not accept the treatment.
Are you using appropriate verbal skills with your patients? Following are a few examples of what you should be saying to patients.
→ Review of Health History Form: “Mike, I noticed some areas of concern on your health history that I’d like to discuss with you. You checked off that you (smoke, have diabetes, have bleeding gums, receding gums, etc). This puts you at greater risk for periodontal disease. Periodontal disease is an infection in the gum tissues. If we catch it early, we can take the necessary steps to prevent it from progressing. That is why I am going to measure your periodontal pockets. As I do it, I’ll let you know what I find.”
→ If probing results are 3-5 mm: “Mike, I see some bleeding when I measure in certain areas and your gums are a bit tender and inflamed in some places. This looks to be the beginning stages of periodontal disease.”
→ If probing depths are ≥5 mm: “Mike, in this procedure, I will not only scale the visible parts of your teeth, but also remove harmful plaque, bacteria, and tartar that have built up below the gum line - the cause of periodontal disease. Once everything is clean, I will place a locally administered antibiotic/antimicrobial called (name the product) particularly in the areas where infection is present. (Product name) is similar to an oral antibiotic/antimicrobial except it is not a pill or rinse. It is tasteless and odorless and is placed at the site of infection - under your gums. It fights the infection at its source to help treat the periodontal disease and hopefully save your teeth. We need to treat the infection in order to bring your teeth and gums back to a place of health. Shall I proceed with this treatment?”
→ Fee discussion: “Mike, our office uses a locally delivered antibiotic along with scaling and root-planing as a standard treatment for the kind of periodontal disease you have. The cost will be ___ dollars. May we proceed with treatment?”
2. Code and charge according to the patient’s condition. The comprehensive periodontal examination will assist in forming the diagnosis of the patient’s periodontal condition. If the patient has pocket depths of ≥5 mm with bleeding upon probing or shows any signs of loss of clinical attachment due to destruction of the periodontal ligament and loss of the adjacent supporting bone, they should not be considered an adult prophylaxis case. This patient needs more extensive scaling and root-planing and more frequent recare appointments. Treating chronic periodontitis equates to a higher fee than an adult prophylaxis. Yet, many offices lose thousands of dollars each year because they do not diagnose properly or charge appropriate fees. According to Karen Davis, practice-management consultant, an office may increase their annual revenues by approximately $20,000 just by daily substituting one adult prophylaxis appointment for a SRP appointment. This amount is based on a fee of $75 for a prophylaxis versus $180 for a SRP and working 16 days per month.
Insurance is another area where proper verbal skills are needed by all team members for enhanced communication with the patient. We all know that most dental insurance plans do not provide complete coverage. Decisions on how to diagnose and treat the patient should always be based on the patient’s condition and not on how much the patient’s insurance will “assist” in paying for the procedure. Educating the patient up front about the realities of dental insurance may release some of the stresses of talking about treatment fees.
3. Charging for LAA. When I ask audiences how much they charge per site for LAA, I receive responses ranging from the cost of the product to $50, $75, and even $100 per site. Most patients will be put off by the thought of paying a lot, especially if they need multiple treatments. Why not charge less per site and increase revenues by increasing patient acceptance? Using Arestin as an example, the product costs the office anywhere from $10 to $16 per cartridge depending on how many boxes are purchased. Since the product has a two-year shelf life, consider buying multiple boxes. I recommend a fee of $25 to $30 per site, which will still increase revenues and patient acceptance. Based on this charge and working 48 weeks per year, 16 days per month, the dental hygienist can increase revenues by $4,800 per year and profit by $2,592. If he or she places five sites per day, the revenues go up to $24,000 and the profit by $12,960 - all of this for about one minute or less per site. Also, since the local delivery of antibiotics/antimicrobials is legal in the majority of states for dental hygienists, it makes sense to incorporate this therapy into the hygiene appointment. The patient can then be scheduled for a three-month recare appointment where the results of the treatment will be reevaluated. If the treatment was not effective, the product may be placed again. Just as with any antibiotic/antimicrobial, results are not always obvious the first time around and it may take an additional treatment to see improvement.
So - go ahead and try it. You will be providing a treatment that has been studied extensively and has shown to be beneficial to thousands of periodontal patients.
The local delivery of antimicrobials/antibiotics are a safe and effective treatment for moderate, chronic peridontitis patients. This is one easy way for the dental hygienist to provide a therapy that is based on evidence and that also will increase revenue. Go for it!
Editor’s note: Rebecca Wilder received an honorarium from OraPharma for writing this article.
Rebecca Wilder is an associate professor and director of graduate dental hygiene education at the University of North Carolina Chapel Hill School of Dentistry. She also is an international speaker, author, and consultant to the dental industry. She may be reached at (919) 966-2800, or e-mail [email protected].