Ask Dr. Christensen
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Gordon J. Christensen, DDS, MSD, PhD
For more on this topic, go to www.dentaleconomics.com and search using the following key words: removable partial dentures, small diameter implants, Dr. Gordon Christensen.
Q I see zirconia-based, full-zirconia, and IPS e.max restorations advertised in many magazines and journals. They seem to be serving relatively well in my practice. However, I am worried about the future with them. I recently had to remove a zirconia-based bridge, and the task required major effort and destruction of several burs. Additionally, I was worried about the trauma to the teeth as I removed the restorations with difficulty. It is obvious that the profession will be facing a dilemma as more of these types of restorations begin to fail clinically and have to be removed. What is the best way to take off these very strong restorations when necessary?
AYour question is very important, since both zirconia and lithium disilicate restorations are becoming very popular. Currently, many practices are using these restorations more than porcelain-fused-to-metal (PFM). The increasing price of metal and the rapid growth of laboratory digital dentistry and in-office CAD/CAM milling of restorations prompt me to predict that all-ceramic crowns will soon not only be more popular than PFM, but will eventually replace PFM.
However, there are looming problems with these all-ceramic restorations. When removing PFM or full-metal crowns, dentists have been accustomed to the simple task of making a slot in the restoration with a bur, placing a screwdriver-like instrument in the slot, and popping the crown off with little or no difficulty.
Such is not the case with zirconia or lithium disilicate restorations. The arduous task of making slots in the restoration and slowly chipping the material from the tooth, piece by piece, is well known to dentists (Figs. 1-5).
There are several important separate points that relate to your question. They include the following:
- ◆ The adequacy of the tooth preparation at the time of cementation
- ◆ The physical characteristics of the ceramic used
- ◆ Whether the restoration is bonded or luted
- ◆ The instrument used to remove the restoration
I will discuss each point individually to answer your question.
Tooth preparation adequacy
It is a well-known fact that many crown tooth preparations have excessive taper on them. Such tooth preparations are not retentive, and removing the restorations is much easier than removing crowns from conventional tooth preparations with near parallel walls. Also, some tooth preparations are too short from the gingival margins to the occlusal table.
Fig. 1: The prosthesis shown is a prematurely failed three-unit fixed partial denture requiring removal. It was fabricated with a zirconia-base and superficial layered ceramic. The reason for failure appeared to be inadequate contouring of the zirconia framework into a miniature crown form. As a result, the layered ceramic was too thick and weak, and it fractured from the framework.
It is generally accepted that when using current cements, at least 3 mm of circumferential parallel tooth structure is necessary to retain a single crown without a buildup. In either of these cases, removing the restorations is easy if they have not been bonded to the tooth surface. However, on the negative side, they are more prone to come off during service.
For optimum service potential, making adequate tooth preparations is suggested, in spite of the increased difficulty when removing the restorations.
Physical characteristics of the ceramic used
The most popular types of all-ceramic restorations currently are zirconia-based, full-zirconia, and lithium-disilicate (IPS e.max). All of these restorations are very difficult to remove. Alumina-based restorations are still used to a minimal degree, and are somewhat easier to remove than zirconia or lithium disilicate. Still available, but not very popular, are leucite reinforced restorations (IPS Empress).
Fig. 2: The fractured piece of ceramic was too thick for optimum strength.
In spite of having lower strength than zirconia or lithium disilicate, the beauty of these restorations is respected and used by knowledgeable clinicians, especially for single crowns in the anterior portion of the mouth.
Leucite reinforced restorations can be relatively easy to remove because of their lower strength. However, almost all dentists bond leucite-reinforced restorations, which can make them more difficult to remove.
Bonded or luted restoration
Clinicians and manufacturers generally accept that nonconventional tooth preparations for ceramic restorations, without typical nearly parallel and slightly tapered tooth preparation walls, require bonding for optimum retention. Additionally, inlays, onlays, partial crowns, and flat tooth preparations with the often-described "circle of circumferential enamel" require bonding. Depending on the nature and adequacy of the bond, these restorations can be very difficult to remove.
On the other hand, clinicians and manufacturers also generally accept that full ceramic crowns can be cemented with conventional cements such as resin-modified glass ionomer. It is obvious that removing a restoration that is "luted" instead of "bonded" would be easier, since the retention of the ceramic to the tooth is primarily achieved by mechanical irregularities rather than chemical bond.
Instrument used to remove the restoration
Most tooth restorations placed early in life require replacement later in life, due to either esthetic or functional unacceptability. In my opinion, one of the most negative characteristics of the strong ceramic restorations is the potential damage caused to the tooth when the restoration must be removed. Extreme care should be taken to minimize the tooth trauma that is inevitable on restoration removal.
Many types of instruments have been suggested to remove ceramic crowns or fixed prostheses, most of which are intended to remove the restoration without damage, thereby allowing recementation and further service. However, when a ceramic restoration breaks, the intention is not additional service in the mouth. The goal is to remove the restoration quickly and easily with minimum irritation or potential damage to the tooth.
If the object is to make an endodontic access hole in an otherwise acceptable restoration, I suggest using very fine grit diamond burs (Fig. 3), running at high speed, using a light touch, and using a virtual flood of water lavage.
The object is to produce as few micro cracks in the functioning restoration as possible, allowing the restoration to remain in service without breaking.
On the other hand, if the object is to remove only the failed restoration, I suggest using a coarse diamond, similarly running the diamond at high speed, using a light touch, and using lots of water.
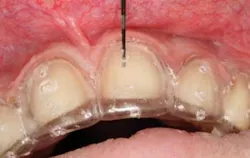
Fig. 4: In this example, the initial attempt to remove the failed restoration was to cut typical slots through the ceramic extending to the tooth preparation, expecting the ceramic to break away and loosen the prosthesis. This did not occur as with PFM restorations.
I suggest using low-cost diamonds such as the NeoDiamond from Microcopy. It is illogical to use high-cost diamonds or special burs for crown removal.
To summarize my answer, I am concerned about the challenges involved in taking off zirconia or lithium disilicate crowns. Both of these popular types of restorations are extremely difficult to remove. The technique I suggest, used with care, is state-of-the-art, but it still has the possibility of causing tooth damage.
Fig. 5: Attempts to segregate the restoration from the tooth were partially successful, even though the prosthesis was cemented with resin-modified glass ionomer. Removal of the prosthesis required several diamond rotary instruments and significant time.
Gordon and Practical Clinical Courses (PCC) have produced two new one-hour videos that are receiving an excellent reception by the profession. Both subjects are in clinical areas that are known to be only marginally acceptable as taught in most schools.
PCC offers a DVD title related to this query – V1993 "Long-Term Maintenance and Repair of Fixed Prostheses." For more information on this title, contact PCC at (800) 223-6569 or visit the website at www.pccdental.com.
Dr. Christensen is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.
Past DE Issues