The rapid evolution of restorative dentistry
by Stephen D. Poss, DDS
This clinician has had the privilege of practicing clinical dentistry since 1983. My, how things have changed in the last 30 years!
The restorative dentistry challenge in the early '80s was determining how far below the gingiva the clinician needed to place the margin of a PFM for esthetic reasons. In addition, for most posterior direct restorations, the main concern was the shiny high polish that was placed on the amalgam restoration.
In the last few years, composite placement has exceeded amalgam as the direct restorative material of choice. The placement of composites has become faster and easier due to the bulk-fill nature of most composite restoratives.
Newer composites have one-half the volumetric shrinkage of similar materials from just a few years ago. Larger class II composites can now be placed with much less concern about shrinkage, dramatically reducing the layering of the composite restoration. These improvements have allowed clinicians greater confidence with composite restorations and have saved much chair time.
Through the years, dental manufacturers have tried to simplify dental adhesives. This was primarily due to complaints about thermal and pressure sensitivity from the total-etch technique. Most of these problems were derived from either overetching the dentin or overdrying the dentin. Since this total-etch technique has been the gold standard for many years, it has taken dentists some time to feel comfortable using self-etchants for restorative needs.
Self-etching adhesives have improved greatly since they were first introduced nearly 10 years ago. Many universal adhesives such as Prime&Bond Elect (DENTSPLY/Caulk), OptiBond XTR (Kerr), Clearfil SE (Kuraray), and Scotchbond Universal (3M ESPE) have simplified adhesive dentistry for direct and indirect restorations.
It is apparent that, as the results of more long-term studies are made available on universal self-adhesives, dentists will continue to migrate toward universal adhesives over the total-etch technique.
In the 1980s there were fewer materials and technological options available for indirect restorations. At that time, every indirect restoration was tooth-borne and would be either a PFM or full-metal restoration – period. The biggest decision the dentist had was whether the metal was going to be precious, semiprecious, or a base metal.
Some of the first metal-free crowns that I placed in the '80s were Dicor (Corning). Dicor crowns were cemented with shaded zinc phosphate. Because of the cementation process, there was a high failure rate. Most of these early types of ceramics are no longer in use.
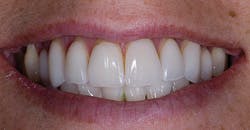
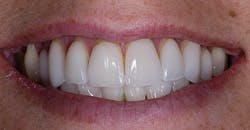
When porcelain systems with high-leucite containing ceramics such as Empress (Ivoclar) and OPC (Pentron) were introduced in the late '80s, the dynamics of dentistry started to change at a more rapid pace. These were the first pressable ceramics. Even with the lower flexural strength of 160 to 200 MPa, I placed numerous units for veneers and single crowns that are still functioning more than 15 years later. (See Figs. 1 and 2.)
Even though these restorations proved to be successful, the total-etch adhesive process impeded the application of these restorations for many general practitioners who feared tooth sensitivity or the failure of the restoration.
In the mid 1990s, Nobel Biocare introduced Procera AllCeram core. This was the first computer- designed CAD/CAM substructure. This new ceramic core allowed a little more forgiveness with the adhesive technique because Procera had a much higher flexural strength. The core was 99% alumina to a feldspathic ceramic layer. Initially, the fit and esthetics were a concern for this ceramic.
At the turn of the millennium, the use of CAD/CAM technology spurred a generation of zirconium dioxide materials. Several manufacturers (CERCON, DENTSPLY; Lava, 3M; and others) introduced crown and bridge frameworks milled from blocks of presintered yttrium-stabilized zirconia.
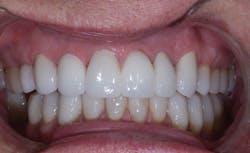
This type of system provided an excellent fit and a flexural strength that was 900 to 1,300 MPa. These materials more closely matched a PFM in strength. The clinician could now fabricate long- span, metal-free bridges. (See Figs. 3 and 4.) This technology also carried over into implant abutments.
In 2006, lithium disilicate e.max (Ivoclar) reemerged as pressable ingot. A milling block was available as an additional option. The flexural strength of this material was found to be more than 170% greater than any leucite-reinforced ceramic Empress used at the time. This ceramic material could be milled or waxed and then pressed to full contour and stained if needed. Additionally, it could be cut back and layered for a higher esthetic need.
In the last several years, full-contour (monolithic) zirconia has grown in popularity due to its strength. There is no layering to this type of zirconia, so the fracture rate has been reduced. Monolithic zirconia can be indicated for single posterior crowns, bridges, implant crowns, and implant abutments. Even though the shading is progressing, it is still a concern for use on the single anterior crown.
In today's market, about 50% of the crowns fabricated are metal free. Two items have enhanced the growth of this market.
The first is that precious metal costs continue to rise, making a porcelain-to-metal restoration more costly to produce. Second, the PPO dental insurance reimbursement rates are declining for indirect restorations. The lower cost of the newer zirconia technology is more attractive for the general practitioner.
As these dental ceramics continue to progress with better esthetics, fit, and flexural strength, the adhesive market has evolved to create an ideal clinical situation that should only get better with time. The dramatic increase in flexural strength of these ceramics has given the clinician a broader range of cement options.
For the zirconia with layered porcelain and monolithic zirconia restorations, the clinician can now use everything from resin-modified glass ionomer cements to self-adhesive cements, or still use the total-etch technique to place the restoration.
One of the inherent weaknesses of zirconia is the bond strength between the resin cement and the crown. Ceramic primers such as Z Bond Plus (Bisco) can significantly enhance the bond strength between the zirconia and the resin luting cement. Placement of e.max (lithium disilicate) can be accomplished through total-etch with resin luting cements or self-adhesive cements.
In this new age of dentistry, the use of metal-free crown and bridgework allows the clinician to offer better esthetics, a more precise fit, and a conservative, biocompatible restoration. As digital scanners become more prevalent in the dental office, the dentist will be able to exceed the expectations of the patient in a more efficient time frame.
It is exciting to see just how far the dental industry has evolved during the last 30 years. The positive direction the profession has taken is impressive.
Stephen D. Poss, DDS, maintains a cosmetic-oriented restorative practice in Brentwood, Tenn. Dr. Poss lectures internationally on esthetic dentistry, sleep apnea, and TMD. He is a consultant to several dental manufacturers on new product development and refinement. Contact Dr. Poss at [email protected].
Past DE Issues