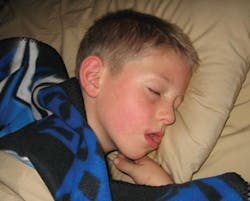
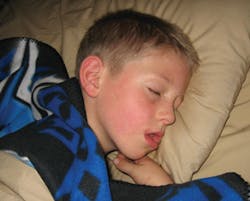
Childhood sleep apnea
Treating a Very Adult Problem for Our Youngest Patients
by Erin E. Elliott, DDS
One of the perks of working for me is that I have kids, so "I get it.” When Sarah, the front office team member, needed Jason and Jett to be dropped off at the office, I immediately said yes. Jett Ryder (yes, that's his real name as his father works on planes) and Jason are great kids. I usually sneak away to play video games with Jason in our kid's waiting area, and he almost always beats me. I call him Michael Jordan because his tongue is always sticking out when he plays.
Between 20% and 50% of the pediatric and adolescent population may have a sleep disorder, but because sleep disorders in this age group are hard to catch, they often go undiagnosed. These sleep disorders can include insomnia, periodic limb movement disorder, restless leg syndrome, and sleep related breathing disorder (SRBD), which includes obstructive sleep apnea. Unlike in adults, these present themselves differently in the younger population but can still have adverse health effects and lead to problems as adults.
Living in northern Idaho away from family and in-laws means we have to get on a plane to visit loved ones. In the past I tried to encourage sleep in my two boys for the long flight back East by giving them Benadryl. I was shocked to learn that Benadryl can actually cause hyperactivity instead of drowsiness. Ask me how I learned this. Because a child's nervous system is still undeveloped, they may not react the way you think, as symptoms of SRBD present differently in children as compared to adults. The chief complaint in adults is fatigue and snoring. Daytime symptoms of inadequate quality sleep in children can present as ADHD and ADD, hyperactivity, behavioral issues and irritability, neurocognitive impairment, and poor school performance. Notice I said "quality sleep.” Jason got nine to 10 hours of sleep a night and slept through the whole night. His mom told me he had no problems sleeping and fell asleep easily at night and didn't nap during the day. But as we dug a little deeper, we found that he was struggling to get oxygen, and therefore, proper sleep.
Thanks to my training in sleep apnea and dental sleep medicine, I realized that there was more to the story of Jason's tongue hanging out. Jason didn't just stick out his tongue when he was playing video games; he stuck it out all the time. I noticed he had his mouth hanging open, tongue out, a runny nose, a muffled voice, and "allergic shiners” or bags under his eyes. During his dental exam, I saw him in a whole new light for the first time. His palate was vaulted, he had a full maxillary/mandibular cross-bite, some acid erosion or pitting in the cusps of his molars, anterior gingivitis due to his mouth breathing, and huge tonsils! When I pointed this out to his mother, she told me he snored like a train but the pediatrician was never concerned because he didn't get sore throats. Who cares about sore throats? This boy can't breathe!
A new American Academy of Pediatrics (AAP) guideline recommends that children who snore be tested for obstructive sleep apnea. The clinical practice guideline, "Diagnosis and Management of Childhood Obstructive Sleep Apnea,” was published in the September 2012 issue of Pediatrics. The guideline recommends in-lab polysomnography for children with daytime learning problems, labored breathing during sleep, and disturbed sleep with frequent gasps, snorts, or pauses. The guidelines also call for children and adolescents to be screened for snoring as part of routine physician visits, but these guidelines are not always followed and many children's sleep issues goes unnoticed and undiagnosed.
The AAP recommends adenotonsillectomy as the first-line treatment for children with sleep apnea. Pediatricians may also recommend weight loss in obese patients or CPAP if surgery is ineffective or not conducted. Fortunately I work with some great ENT surgeons. We were able to refer Jason directly to an ENT who set him up for a tonsillectomy and adenoidectomy, and I was able to observe the surgery. In addition, we expanded Jason's palate orthodontically to reduce his nasal obstruction and improve tongue space.
He is now doing wonderfully. He's eating better because he can actually swallow food, growing because he's actually getting restful sleep, and going to sleepovers because he's no longer embarrassed.
If you know any kids like Jason, please educate the parents and get them help. As dentists, we may very well be the only exposure patients and parents have to learn about this.
Erin E. Elliott, DDS, is a partner at Post Falls Family Dental Center and Sleep Better Northwest in Post Falls, ID, where she practices family dentistry. She has a special interest in screening and treating people with sleep apnea and snoring. She's a member of the American Dental Association, American Academy of Sleep Medicine, and the American Academy of Dental Sleep Medicine. You can reach her at [email protected] or find more information at www.sleepbetternw.com.
Past DE Issues