New clinical entity emerges ...
For more on this topic, go to www.dentaleconomics.com and search using the following key words: oral cancer, lesions, early detection technologies, adjunctive oral cancer screening instruments.
Users of adjunctive oral cancer screening technologies are observing subtle tissue changes not obvious under white light for which there is no published clinical term, which may be considered pre–neoplasia. The potential of these early discoveries to convert to dysplasia is unknown. Until a consensus is reached about how to manage pre–neoplasias, appropriate management is unclear.
Although the prevalence and genetic conversion statistics of leukoplakia, erythroplakia, and mixed dysplasias are well–covered in scientific literature, there is a group of lesions that may appear normal under white light examination and that likely have a very low probability of ever becoming a clinically visible entity. This category of potential pathology should not be ignored. Although at this point my suggestion that pre–neoplasias exist may be heretical, the following stories prove otherwise.
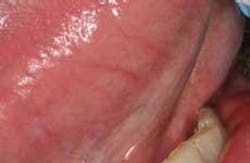
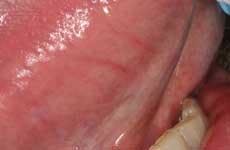
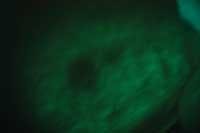
Last year, an Amish gentleman presented to my practice complaining of a fractured cusp of a mandibular molar. On the buccal mucosa adjacent to the fractured tooth, there was clearly a minor traumatic ulceration in a sea of healthy pink mucosa — or so I thought. Since my staff was excited about our new VELscope®, my assistant had it ready for me and insisted that I practice using it despite my original dismissal of using it because everything looked normal. A large, dark area surrounding the retromolar pad and extending into the retromylohyoid space appeared. According to accepted protocols, I had the patient come back in two weeks for follow–up.
The area still looked absolutely normal clinically, but was still dark under direct tissue fluorescence. Still doubtful, I collected a brush cytology specimen. The result suggested abnormal cells, so I took a small wedge of tissue from the area of lost fluorescence. The diagnosis was “mild dysplasia,” and the oral pathologist suggested that if the lesion persisted it should be removed. To make a long story short, the case was successfully treated nonsurgically, and the patient's tissues look fantastic 18 months later. (Huff, KD, et. al. A novel, minimally invasive approach to managing mild epithelial dysplasia. General Dentistry. In Press, 2009.)
About two years ago, a nurse presented to my office for hygiene recall. My hygienist discovered a very early lesion on the floor of the patient's mouth with adjunctive technology. Since the area appeared clinically normal to me, I dismissed my hygienist's findings as a variation in normal appearance. The patient insisted that I do something to find out what my hygienist had observed. Still skeptical, I performed brush cytology. The results were: “Atypical, warranting further investigation.” I then performed an excisional biopsy of the area, which came back as “mild dysplasia, premalignancy potential uncertain.” More than two years later, the patient's tissues appear healthy clinically and under conventional lighting. She has referred more patients to me directly and indirectly than I can track.
Neither of these lesions hinted at any abnormality clinically. Although both of these cases proved that there were clinically abnormal entities present, neither case was cancer. Some would argue that these were false positives, but they weren't because I had no assumption that they were cancer. Over the years, I have come to trust early cancer technology for what it is — a way to take a closer look at what may be lurking around the corner.
I have no disagreement with those who claim that early detection technologies may stimulate overtreatment. The same argument has been made about breast biopsies. However, I would much rather have something removed from my mouth that “might become” something rather than wait for it to become cancer. From what I've heard, I know my patients would too.
Kevin D. Huff, DDS, MAGD, is a practicing general dentist in rural Ohio, a private researcher, author, and dental educator. A clinical instructor at the Case School of Dental Medicine, he lectures nationally about oral cancer screening and biopsy techniques. Contact him at [email protected], or visit www.doctorhuff.net.