Ask Dr. Christensen
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: bonding agents, etch and rinse, self-etch, bond to dentin, bond to enamel, bonding techniques, Dr. Gordon Christensen.- The types (generations) of bonding agents available
- Differences among the types
- Clinical significance of the differences among types
- Suggested clinical techniques and products
Identifiable generations of bonding agents
There are currently seven — and some companies even claim eight — generations of dentin bonding agents.The first three generations, introduced up to 50 years ago, are now of only historical significance.
The fourth generation bonding agents were introduced in the early 1990s. The fifth generation was introduced in the mid-1990s. These two generations included the first products in the total-etch concept, now called “etch and rinse” by some. Using the total-etch technique, the tooth structure, enamel, and dentin are etched, removing the smear layer completely, then washed, primed with a second priming “wetting” constituent, and sealed with an unfilled bonding resin.
In the fifth generation, the prime and bond constituents were placed together. The fourth and fifth generations are still considered to be the so-called “gold standard” for tooth-bonding by many researchers because the techniques removed all of the debris (smear layer) on the tooth, and, when done correctly, sealed and desensitized the tooth.
This concept was excellent if used correctly. A representative three-constituent product that most dentists will remember is 3M ESPE Scotchbond Multi-Purpose. An example of a fifth generation two-bottle product with combined primer and bond is DENTSPLY Caulk Prime & Bond® NT™. Both of these products are currently used by some dentists.
Challenges and positives of etch and rinse
The challenge with the etch and rinse concept is that since the dentin canals are opened and debrided completely by the acid etch, the acid, primer, and unfilled bond have to be used meticulously or postoperative tooth sensitivity can occur. Our research has shown two times the postoperative tooth sensitivity in typical, busy practices using the etch and rinse concept vs. the self-etch concept. However, I can verify that if the technique is done well, there is minimal or no postoperative tooth sensitivity.
What are the potentially positive aspects of the etch and rinse technique?
Research shows that the bond to enamel produced by the etch and rinse technique is usually better than the bond produced by some of the self-etch bonding products we will discuss later. Is this greater bond clinically significant?
That is a moot point. For generations, dentists have successfully placed long-lasting restorations without anyFig. 4 — Examples of resin-modified glass ionomers.
If you want to use the etch and rinse generations — as many dentists do — please carry out the clinical procedure meticulously, and you will have optimum success.
Self-etching products
The sixth and seventh generations are the products being used by the majority of U.S. dentists today. These are the “self-etching” products. The sixth generation has two ingredients — one being an acidic primer and wetting agent and the other being an unfilled bonding agent. Most sixth generation bonding agents have a relatively thick film of about 40 microns (the approximate thickness of a human hair).
The seventh generation bonding agents are usually composed of only one ingredient, with all of theWhy have so many dentists selected self-etching types of bonding agents?
The previously described etch and rinse systems were excellent if used properly; however, the unpredictable, frustrating, and patient-upsetting postoperative tooth sensitivity frequently produced by etch and rinse systems led to the change to self-etch systems. Research from many locations, especially dental schools, has produced varying reports on self-etch products. Generally, they report decreased postoperative tooth sensitivity and similar, measurable bonds to dentin as those produced using the etch and rinse systems.
The only potentially negative characteristic of self-etch products is the previously mentioned reduced bond toIn summary, both etch and rinse and self-etch bonding agents have been reported to produce similar bonds to dentin, although some brands of self-etch products have received reports of somewhat reduced bonds to cut and uncut self-etched enamel.
Dentin vs. enamel bonding
Is the bond to dentin reported for these etch and rinse or self-etch products a long-term one, as is known to be the case with enamel?
Summarizing the available reports, combined with the clinical observations of “real world” dentists in their practices, enamel bonding is strong when done properly and it remains indefinitely, while dentin bonding is less predictable and reliable.
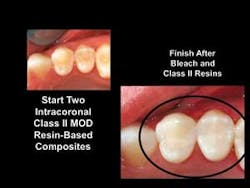
Any dentist who has removed ceramic veneers from “dentin-bonded” teeth knows that the ceramic can easilyFig. 7 — An example of the excellent and predictable results to be obtained with current bonding agents and resin-based composites.
I am pleased to have the significant tooth desensitization provided by dentin bonding agents, but I consider the less predictable dentin bond provided by these agents to be a bonus when present, not an expectation.
Bonding and desensitizing procedures
The following successful bonding and desensitizing procedures are listed in order of etch and rinse and then self-etch. All of these techniques have been reported in the dental literature as successful clinical procedures when done correctly! I will provide my favorite procedure at the end of the list.
Comments about these techniques:
- The popular glutaraldehyde/HEMA solutions such as G5 (Clinician’s Choice); GLUMA (Heraeus Kulzer); Glu/Sense™ (Centrix), or MicroPrime G (Danville) will be noted as glutaraldehyde in the descriptions that follow. After significant scientific investigation by our own group, I prefer to use glutaraldehyde application in all of the techniques discussed in this article. You may differ with my conclusions and either exclude the glutaraldehyde completely from the techniques or substitute it with another desensitizer/disinfectant of your choice.
- Many research projects show that placement of two coats of bond are better in producing bond and reducing sensitivity than one coat. Below “bond” means two coats.
- Total-etch indicates etching enamel and dentin with a single solution, followed by primer and then bond or prime and bond together (the fourth or fifth generation of bonding agents).
- Self-etch indicates use of one of the sixth or seventh generation of bonding agents
- Primer and bond may be in separate containers or distributed combined in one container.
Techniques for dentin and enamel bonding
- Total-etch: Tooth preparation, etch and rinse entire preparation, glutaraldehyde, primer, bond, composite restorative
- Total-etch: Tooth preparation, etch and rinse, glutaraldehyde, primer, bond, thin flowable resin layer, composite restorative
- Total-etch:Tooth preparation, etch and rinse, glutaraldehyde, resin-modified glass ionomer on deepest dentin surfaces (3M ESPE VitreBond™ or GC Fuji LINING LC), primer, bond, composite restorative
- Self-etch: Tooth preparation, glutaraldehyde, self-etch primer, bond, composite restorative
- Self-etch: Tooth preparation, etch external enamel margins with gel resin and rinse rapidly, glutaraldehyde, self-etch primer, bond, composite restorative
- Self-etch: Tooth preparation, glutaraldehyde, self-etch primer, bond, thin layer of flowable resin, composite restorative
- Self-etch:Tooth preparation, etch external enamel margins with gel resin and rinse rapidly, glutaraldehyde, self-etch primer, bond, thin layer of flowable resin, composite restorative
- Self-etch: Tooth preparation, etch external enamel margins with gel resin and rinse rapidly, glutaraldehyde, resin-modified glass ionomer on deepest dentin surfaces (3M ESPE VitreBond or GC Fuji LINING LC), self-etch primer, bond, composite restorative
In summary, all of the preceding techniques when accomplished properly have been reported to be successful according to various dental publications; however, after combining this research with formal and informal surveys of practitioners, I prefer technique No. 8 for busy practices with the known challenge of predictably treating multiple patients. This technique offers high-quality restorations in minimal time. An explanation of my favorite technique (No. 8) follows:
- Gel-etch the enamel margins after the cavity preparation is complete. Doing this with a rapid, high-volume air-water spray ensures etch of the enamel. (Reports on some of the new self-etch primers are showing adequate bond to enamel without this step.)
- Glutaraldehyde/HEMA application encourages desensitization and disinfection of the tooth preparation.
- Resin-modified glass-ionomer liner bonds to the deep dentin areas, desensitizes, and releases fluoride.
- Self-etch primer and bond reduces or eliminates postoperative sensitivity.
- Adequately powerful curing lights and thin layers of restorative resin (up to 2 mm) help to reduce postoperative tooth sensitivity.
- This technique has proven clinical predictability and success.
If you prefer an etch and rinse technique, I prefer technique No. 3 over using resin-modified glass ionomer as a liner.
The bottom line is that any of the techniques listed will work when performed correctly. Speakers you have been listening to may have stated their personal preferences/opinions too strongly, thus confusing you.
Practical Clinical Courses provides a “bread-and-butter” hands-on course titled “Practical Esthetic Restorative Dentistry.” In it, we include the best bonding techniques, resins, veneers, ceramic restorations (indirect and milled in-office), and ceramic crowns, as well as including samples of the best and most predictable materials in all areas for you to take home with you.
If you are interested in our next date, May 20-21, please go online to register at www.pccdental.com or contact PCC at (800) 223-6569 for more information.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.