The dangers of being numb
by Fred S. Margolis, DDS, FICD, FACD, FADI, FADPD
For more on this topic, go to www.dentaleconomics.com and search using the following key words: anesthesia, numb, anesthetic, pediatric dentistry, oral tissue, Dr. Fred S. Margolis.
all of us have either children, special needs, and/or geriatric patients in our dental practices. Many children, developmentally delayed teenagers, and cognitively impaired adult patients do not understand the dangers of chewing on the soft tissues subsequent to the use of topical or local anesthesia. In Gerald Wright’s book, “Managing Children’s Behavior in the Dental Office,” he states, “Young children are prone to lip or cheek biting” (Fig. 1).
Our geriatric patients may have cognitive disabilities such that they also are not aware of the dangers of chewing or picking on their anesthetized oral tissues.
This category includes the following:
- The patient with whom communication is not possible because of physical or mental health or cognitive understanding problems.
- The patient who is not aware of the dangers of biting or picking at the oral tissues after a topical or local anesthetic is used.
Can we provide local anesthesia in a painless manner and in such a way that the child does not have anesthesia to the lip, tongue, and cheek? The answer to these questions is unequivacably yes, and the author will discuss several techniques for providing dental anesthesia without the postoperative numbing effects of mandibular blocks and maxillary infiltrations.
Intrasulcular injection technique — the periodontal syringe
Several dental manufacturers offer periodontal ligament injection syringes. The periodontal ligament syringe has the benefit of enabling the dentist to anesthetize one or several teeth without the use of block anesthesia. For example, a periodontal syringe can be used to anesthetize a primary molar or bicuspid by placing the needle into the sulcus and injecting slowly when the tip of the needle is at the crestal bone.
This provides anesthesia without going into the periodontal ligament space, which prevents postoperative pain. In using this technique for more than 15 years, I have found that it can anesthetize an individual tooth in less than one minute without concomitant numbing of the lip, tongue, and cheek.
The use of a plastic-hubbed, 30-gauge needle will hermetically seal the anesthetic solution without allowing it to drip into the mouth. The advantage of an enclosed anesthetic carpule is protection in case the glass carpule breaks under excessive pressure. In my practice, I use the Paroject® (Septodont, New Castle, Del.) (Fig. 2).
Intraligamentary anesthesia — STA system
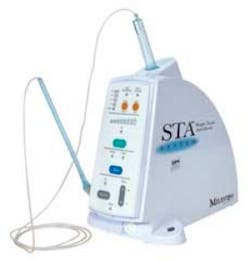
Milestone Scientific Corporation (Livingston, N.J.) has a new single–tooth anesthesia device, STA®, that has remarkable benefits for dentists and patients. My patients describe the injection as a “slight pressure;” however, they also report no numbness of the lip, tongue, or cheek (Figs. 3 and 4).
Here are some advantages:
- Computerized control of the flow rate of anesthetic delivery and the pressure applied when giving the injection.
- Computerized dosage of the amount of local anesthesia injected.
- Specially designed needle for the intraligamentary injection.
- Rapid onset of anesthesia.
- Only the tooth and surrounding gingiva are anesthetized.
- Can be used for AMSA and P–ASA block anesthesia, if desired.
- Less anesthesia is required, eliminating worries about toxicity.
- Multiple–quadrant dentistry saves time and increases production.
Erbium lasers
The erbium laser can be used to provide “conditioning” or laser analgesia. Erbium lasers can be used to perform the entire procedure: cavity preparation, caries removal, coagulation of the exposed pulp, and pulpotomy or pulpectomy, if needed. This makes it unique. These procedures can often be performed without the use of local anesthesia.
Several theories exist as to how the erbium laser provides analgesia to the tooth. The author has used the erbium laser for more than nine years and has achieved successful analgesia in more than 90% of my patients.
Fig. 4 — The STA® system
Injectable anesthetic reversal agent
OraVerse® (phentolamine mesylate) injection is a local anesthetic reversal agent that accelerates the return to normal sensation and function following dental procedures. OraVerse is indicated for the reversal of soft-tissue anesthesia; i.e., anesthesia of the lip and tongue resulting from an intraoral submucosal injection of a local anesthetic containing a vasoconstrictor.
According to the manufacturer, OraVerse is not recommended for use in children under age 6 or children weighing less than 33 pounds (15 kg).
Conclusion
Biting of the oral soft tissues following the use of local anesthesia is a common occurrence in dental practices. Many of our patients are either too young to understand or do not have the ability to understand the dental team’s message about not biting on the soft tissues of the lip, tongue, and cheek while “numb” after a dental procedure.
Several ways of providing anesthesia to teeth without the subsequent numb feeling, or shortening the time of the patient being numb were discussed in this article.
In 1931, Dr. Edmund Wuerpel, an orthodontist, wrote: “The mind of a child is as tender and as lovely as the petals of a full-blown rose. Beware how you touch it! Meet it with all the reverence of your being. Use it with gentle respect and fill it with the honey of love, the perfume of faith, and tenderness of tolerance. Thus shall you fulfill the mission of your life.”
Dr. Fred Margolis received his certificate in pediatric dentistry from the University of Illinois College of Dentistry. Dr. Margolis is a clinical instructor at Loyola University’s Oral Health Center and an adjunct clinical assistant professor at the University of Illinois College of Dentistry. He is co-author of the book, “Pediatric Laser Dentistry: A User’s Guide,” Quintessence, 2010. Dr. Margolis is in the full-time private practice of pediatric dentistry in Buffalo Grove, Ill. He can be reached at [email protected] or (847) 537-7695.