Ask Dr. Christensen
Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Resin-Modified Glass Ionomer vs. Flowable as a Liner or Base
Q I’m perplexed by the changing use of liners and bases under restorations, both direct and indirect. Some speakers and authors are promoting use of flowable resin-based composites as liners under composites. However, some advocate resin-modified glass ionomer (RMGI), some are using calcium hydroxide, and others are using some new regenerative materials. What is currently the best material to use when bases or liners are necessary?
A There are many choices for bases and liners, and it is interesting that most of them work well if placed correctly. However, dentists tell me that patients complain about postoperative tooth sensitivity related to placement of both direct and indirect resin and ceramic, as well as with amalgam.
There are various reasons for use of a base or liner for direct and indirect restorations. Among them are:
- Prevention of postoperative tooth sensitivity
- Capping a slight pulp exposure
- Stimulation of new dentin formation under the restoration (indirect pulp capping)
- Assisting putty viscosity, fully filled resin-based composite to go into undercuts and marginal areas when placing composite resin directly, especially in Class II box forms
As with any clinical procedure, many techniques will work. If you’re satisfied with the clinical results you’re experiencing with the base and liner techniques you’re using, I suggest not changing. On the other hand, if you’re experiencing challenges and failures with your current technique, I have some suggestions.
The most popular materials currently used for liners and bases are:
- Resin-modified glass ionomer (examples are 3M ESPE Vitrebond Plus, GC Fuji Lining Cement LC, and Southern Dental Industries Riva).
- Flowable resin-based composite (examples are available from every restorative resin company, and some well-proven and highly filled ones are GC America G-aenial and Shofu Beautifil Flow Plus).
- Calcium hydroxide (examples are Dentsply Caulk Dycal and Kerr Life).
- Bonding agents (examples are available from every restorative resin company, and popular brands include Kuraray Clearfil SE Protect Bond, 3M ESPE Scotchbond Universal, and Kerr OptiBond XTR).
- Inorganic chemicals (examples are Dentsply Caulk MTA paste and Bisco TheraCal).
Each of these types of liners or bases has its group of advocates, and all have reported success. In my answer, I will tell you my choice for liners or bases, primarily for directly placed resin-based composite, a technique I use for its placement, and the logic behind why I prefer that concept. Flowable resin-based composite and RMGI will be emphasized.
Using RMGI compared with flowable resin-based composite as a liner or base
Most flowable resins are resin rich versions of fully filled composite resins. They contain the same chemical and filler ingredients as fully filled composite resins; there is just more resin and less filler present than in restorative resins. The chemical constituents of flowable resin, with the exception of the inert filler, can be irritating to the dental pulp. Optimum sealing of the dentinal canals must be done before placing flowable resin as a base or liner. If bonding is done adequately, this type of base or liner works well. However, remember that desensitization of the tooth is related to closing (plugging) the dentinal canals by the bonding agent and not by the flowable resin. If closure of the dentinal canals is not accomplished with adequate use of the bonding agent, the same type of postoperative tooth sensitivity that occurs when using fully filled restorative resin will occur.
The advantages of using flowable resin as the base or liner are:
- It is very easy to use.
- The flowable resin color can match the tooth structure almost exactly without causing any disagreeable final color in the restoration.
- The very fluid flowable resin fills irregularities easily because of the flowable characteristics.
However, flowable resin used as a liner or base does not contain fluoride in clinically significant quantities for potential preventive effect, and it can irritate pulpal tissue if bonding agents are not used to an optimum level to occlude the dentinal canals.
RMGI has the following advantages:
- It bonds to dentin with a chemical chelation interaction and does not require use of a dentin bonding agent before placement.
- It has been shown to release fluoride ion during service with the potential preventive effect of this chemical.
- It is relatively easy to use.
The negative aspects of RMGI used as a liner or base are:
- Final set of the material requires many hours.
- On initial placement, it is not strong.
- Color of the material is not as close to tooth color as flowable resin.
- Placement of the material is somewhat more difficult than flowable resin.
On polling large groups of continuing education audiences, I concluded that near equal percentages of practitioners use RMGI and flowable resin as their primary material for liners or bases, and some use both. Obviously, both techniques work adequately when used properly. The technique I favor follows.
Use of resin-modified glass ionomer as a liner or base
The following technique is for use of RMGI as a liner or base for direct resin-based composite restorations using a self-etch bonding agent. Use of total-etch or selective-etch would be slightly different. Any of the three techniques works well if accomplished properly.
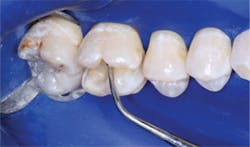
- Prepare the tooth to optimum characteristics.
- Remove any remaining carious material that is deeper than optimum level.
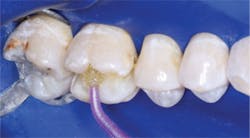
- Place glutaraldehyde solution (examples are Heraeus Kulzer Gluma, Danville MicroPrime, Clinician’s Choice G5, Centrix Glu/Sense). Optimum use according to microbiologic research at TRAC research, a nonprofit component of Clinicians Report (CR), is two 1-minute separate applications of glutaraldehyde solution, sucked off, NOT washed off. However, any use of glutaraldehyde is advantageous regardless of time of contact. Do not get the glutaraldehyde solution on the soft tissue. These solutions ARE NOT a problem when used before dentin bonding agents in spite of some companies that recommend not using them. Recent CR research has shown that glutaraldehyde solutions either do not alter the bonding values, or slightly improve the bond of bonding agents at placement and at six-month testing. More information is available in the August 2012 issue of Clinicians Report at www.cliniciansreport.org.
- Place resin-modified glass ionomer on the deepest areas of the tooth preparation, not on the margins. The material should be about 0.5 mm thick or slightly thicker. Cure it.
- Place the self-etch bonding agent of your choice. The bonding brands noted in this article have well-proven excellent results on dentin and enamel without total etching. Although when total-etch is done well it is successful, our research shows it creates significantly more unpredictable postoperative tooth sensitivity than self-etch techniques.
- Place the restorative resin in increments, starting with 0.5 mm in the deepest portion of the box form, increasing to 1.0 mm and finally to 2.0 mm increments. Clinicians Report research has shown that currently popular curing lights do not cure the entire depth of a typical box form at 7 mm.
- Finish and polish the restoration.
Tooth preparations for onlays or inlays
When making a tooth preparation for an indirect onlay or inlay, the liner or base technique is similar to the described direct technique up to the time when the tooth preparation is completed. At that time, either a provisional restoration is made, or if you’re using a CEREC or an E4D device, the digital impression is made and the restoration is milled or sent to the respective company laboratory. At the time of cementation of the restoration, the glutaraldehyde solution is again placed on the entire tooth preparation before the placement of any bonding agent or self-adhesive cement.
Filling holes or voids in full-crown preparations
When full-crown tooth preparations require holes or voids to be filled (examples are deep Class II box forms, or Class V’s that are deeper than the planned axial wall depth of the crown preparation), fillers for the holes are highly desirable. These fillers prevent the impression material from being distorted when pulled off the tooth preparation. Fillers are for small holes that are not considered large enough for typical bonded composite tooth buildups.
I prefer to use a different technique from the RMGI one for these small bases as follows:
- Make initial gross tooth preparation for the crown down to the gingival line, leaving the previous restorative material in place.
- Remove the remaining previous restorations or caries.
- Place glutaraldehyde on the entire tooth preparation. This solution is placed now and just before restoration cementation.
- Suction off glutaraldehyde; do not wash it off.
- Place self-etch bonding agent.
- Place compomer (example Dentsply Caulk Dyract eXtra).
- Complete tooth preparation for a crown.
- Make the impression.
- Make the indirect restoration by the in-office milling technique or have a dental lab make it.
- Clean the tooth preparation and place glutaraldehyde on the tooth preparation and suction it off.
- Seat the restoration, clean off the cement debris, and evaluate the occlusion.
Practical Clinical Courses (PCC) has a new one-hour DVD presentation that shows both the RMGI and the flowable materials used as liners/bases, as well as the proven best new composite materials, matrices, curing lights, and finishing concepts and materials for all aspects of the Class II resin-based composite procedure.
PCC has an excellent DVD that shows all aspects of the Class II technique — “Class II Composite Resins Can Be Predictable, Non-Sensitive, and Profitable” (Item # V3554). For more information, contact us at www.pccdental.com or 800-223-6569
To briefly summarize my answer, I’m convinced that use of resin-modified glass ionomer is advantageous and proven for use as a liner or base in the deep areas, nonmargins, for both direct and indirect restorations, and that it is currently the best procedure. However, there are always new concepts coming on the market, and this is certainly the case with liners and bases.
Gordon Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Dr. Rella Christensen) and CEO of CLINICIANS REPORT (formerly Clinical Research Associates).
Past DE Issues