Who needs models?
Redefining the dentist-laboratory relationship in the age of digital dentistry
Lee Culp, CDT
The arrival of the new millennium seemed to be the catalyst for change in digital dentistry-several different CAD/CAM systems have been introduced as restorative dentistry solutions since then, though it has taken slightly longer than anticipated to integrate this technology into daily practice.
Today's chairside and laboratory-based CAD/CAM systems are used to design and manufacture implant abutments, bars, zirconia restorations, all-ceramic and composite full-contour crowns, inlays, and veneers that may be stronger, better-fitting, and more esthetic than restorations fabricated using traditional methods.
As restorative dentistry evolves and incorporates digital imaging, computer design, and robot-created restorations, our perceptions and definitions of the dental laboratory must evolve as well. In order to fully understand these concepts, we must first define what a laboratory is. Initially, we might say that a laboratory is the place that a dentist sends impressions to be processed into restorations, which are then sent back for adjustment and delivery. This definition fits well with the traditional concept of a dentist-laboratory workflow. However, just as the Internet has forever changed the landscape of communication, electronic CAD/CAM restoration files catalyzed significant change in the way we view and structure the dentist- laboratory relationship.
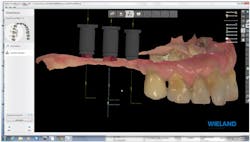
Figure 1: Intraoral scan uploaded into design software
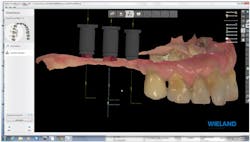
Figure 2: Manual alignment of implant scan flags
Let us imagine first that our laboratory is not a place, does not have walls, and exists only in the talents of the two partners in the restorative process-the dentist and technician. The equipment they use to create the restoration may be located next to the chair or in a dental laboratory. Their "laboratory" is actually nothing more than a workflow, which is flexible to the degree that abilities, access, and equipment allow. The primary decision is the timing of the hand-off from one partner to another. Moreover, a dentist who can use optical intraoral scans for impressions and who often chooses CAD/CAM restorations as the best patient treatment option has, I believe, more freedom in the timing of the hand-off to the technician partner. The laboratory is no longer a place; it is, to a large degree, a virtual and fluid entity.
In some instances, it makes sense for the dentist to independently prepare, design, and finish the restoration chairside during a single visit using the obvious advantages of a clinical CAD/CAM system. Other times, it is advantageous to engage the services of the restorative partner (i.e., a dental technician), because he or she possesses the skill and, perhaps more importantly, the time to create restorations that either demand more complex characterization or can be more efficiently created by someone other than the dentist.
In the conventional indirect restorative process, the procedure begins with the usual steps: The clinician prepares the case according to the appropriate guidelines, makes an impression, and sends these and other critical information to the laboratory. After the laboratory receives all the materials from the dentist, the impression is poured, the models mounted, and the dies trimmed. These models are then used to fabricate appropriate restorations-either layered, pressed, milled, cast, or combinations.
Even though this application offers many advantages to the dentist-technician team, it still requires taking intraoral impressions using conventional techniques, sending these impressions to the laboratory for the creation of stone models, and fabricating traditionally created dental restorations.
In this article, we would like to explore the next phase in the evolution of the dentist-technician working relationship. Our patient was in need of a restoration to replace the missing posterior in the maxillary right quadrant. We elected not to use a conventional workflow that would have required impressions, implant impression analogs, the creation of stone models to produce a laboratory-fabricated set of implant abutments and the final restoration. Instead, we chose a completely digital method that did not require the use of traditional impression materials or the fabrication of dental models.
Once the implants were deemed ready for the restorative phase, a digital impression was created using the 3Shape Trios intraoral scanner, the maxillary-mandibular arches were scanned, and the implant positions were virtually referenced with the use of "scan flags" that were placed into each implant and scanned to create our digital file. These were then sent to the laboratory through a communication portal (figure 1).
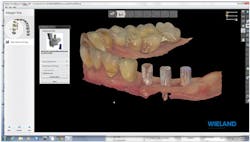
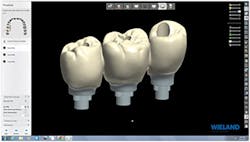
Figure 3: Design of custom implant abutments, Zenostar zirconia bridge, and screw access holes
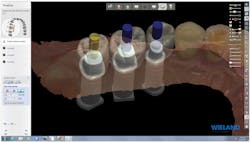
Figure 4: Completed design of abutments and restoration
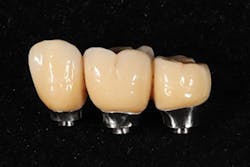
Figure 5: Completed screw-retained implant restoration
Upon the laboratory's receipt of the data file, the scans were uploaded into the design software, and the implants were identified for the correct implant type, size, and position (figure 2).
Using the 3Shape restorative design software, the implant abutments and final Zenostar zirconia restorations were designed simultaneously. This allowed their designs to be tailored to best create the proper function, esthetics, and emergence profile for optimum tissue health and esthetics. This restoration was also designed to be screw-retained for removal for follow-up inspection (figures 3-4).
Upon completion of the design work, the design file for the Zenostar zirconia restoration was sent to the in-laboratory milling center for fabrication, while the custom implant abutments were sent to a milling center that specializes in titanium milling. While the implant abutments were being fabricated, our team completed the Zenostar full-contour zirconia bridge. When the implant abutments were shipped back to the laboratory, we checked for fit accuracy, and then sent both the implant abutments and Zenostar zirconia restoration to the prescribing dentist (figure 5).
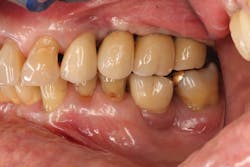
Figure 6: Facial view of final restoration
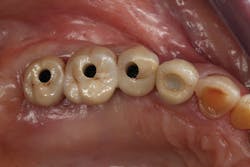
Figure 7: Occlusal view of final restoration
The screw-retained implant abutments and the final restoration were all created without the use of impression materials or the fabrication of dental models. The implant restoration was placed with very minimal adjustment to the occlusal surface; no adjustment was required to the interproximal contact (figures 6-7).
The dental profession currently regards CAD/CAM technology as just a machine that fabricates full-contour ceramic restorations or frameworks. Digital dentistry and the digital dental team represents a totally new way to diagnose, plan treatment, and create functional esthetic restorations in a more productive and efficient manner. CAD/CAM dentistry will only further enhance the dentist-assistant-technician relationship as we move together into this new era of patient care.
Photo credits:
Figures 1-4 are courtesy of Lee Culp; figures 5-7 are courtesy of Dr. Jonathan Ferencz.
Lee Culp, CDT, is the CEO of Sculpture Studios, a dental laboratory, education, research, and product development center specializing in new and innovative digital dental technologies and their applied applications to diagnostic, restorative, and surgical dentistry. He is a leading resource and inventor for many of the materials, products, and techniques used in dentistry today, and holds numerous patents for his ideas and products.
Jonathan Ferencz, DDS, is a clinical professor of postgraduate prosthodontics at New York University.