Revisiting glass ionomer as a restorative material
In recent years, there have been significant developments in restorative dental materials. The dental profession has seen the introduction of two main types of esthetic direct-restorative materials: glass ionomers and adhesive-based resin composites. Some writers argue that there may no longer be a need for a reliance on glass ionomers, since nowadays composites offer so many advantages - such as excellent esthetics, wear resistance, and strength - and are so much improved over what they were like in the past.1-4 Their arguments are understandable, as conventional glass ionomer cements tended to exhibit poor physicomechanical properties, making them more susceptible to wear. They also had slow self-setting reactions, such that preliminary finishing could not be done for 10 minutes, and final finishing could not be done for 24 hours or more.5
However, new glass ionomers have demonstrated significant improvements. They now have better physical and optical properties, and therefore complement restorative dentistry with special characteristics - ones that seem to guarantee them a continued place in our profession. New glass ionomers offer unique clinical benefits, such as fluoride release, recharging of fluoride, possible dentin remineralization within preparations, moisture tolerance, and chemical self-adhesion, so that clinicians are likely to continue to rely upon them for the foreseeable future.6
Some of the improvements in glass ionomers can be attributed to enhancements in resin-modified glass ionomer restorative chemistry, which involves the addition of water-soluble photopolymerizable resin monomers, 2-hydroxyethylmethacrylate (HEMA) to the acidic cement liquid. For powder-liquid resin-modified glass ionomers, some manufacturers have developed proprietary resin formulations. These enhancements allow them to be dual cured - self-setting and light cured. When compared to conventional glass ionomers, these resin-modified glass ionomers display improved physicomechanical properties, resistance to early contamination by moisture, less microleakage, improved adhesion to enamel and dentin, and significant improvement in esthetic properties.
Additionally, glass ionomers are recognized for their good adhesive bond properties to tooth structure, which allow them to form tight seals between the internal structures of the tooth and the surrounding environment. Glass ionomers release fluoride, which prevents further enamel demineralization and promotes remineralization. This release of fluoride can also hinder bacterial growth by inhibiting metabolic enzymes within the bacteria, reducing the acid produced during the bacteria’s digestion of food, and thereby reducing pH and preventing the formation of secondary caries.7-9
Indications for next-generation glass ionomers
In our practices, we utilize modern glass ionomer materials for the following procedures:
- restorations of non-occlusion-bearing Class I cavities
- semipermanent restorations of Class I and Class II cavities
- restorations of cervical lesions
- Class V cavities
- root caries
- restorations of Class III cavities
- restorations of deciduous teeth
They are also indicated for the following:
- use as a base/liner
- core buildup
- temporary restorations
- extended fissure sealing
Case report: Class V restoration
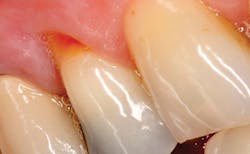
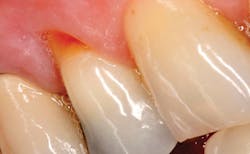
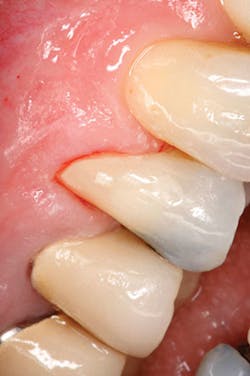
A 59-year-old male presented with a Class V carious lesion (figure 1). Based upon the patient’s risk assessment, it was determined that the best treatment plan was to restore the lesion with a glass ionomer restorative material such as IonoStar Plus (Voco), due to its handling characteristics, esthetics, and fluoride release. The nonsticky, composite-like handling and immediate packability of the material were desirable characteristics for treating the lesion. The material had the added benefit of a new direct-activation application capsule without the need for an adhesive, reducing the chair time required. The finished restoration (figure 2) provided desirable esthetics as well as a reduction in caries susceptibility.
Class II restorations
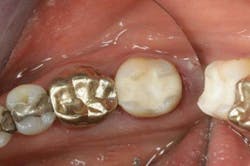
Figure 3 shows a well-sealed Class II restoration using IonoStar Plus. IonoStar Plus features ease of placement, along with the benefit of a two-stage consistency, which allows for packability. It has high compressive strength and wear resistance, making it well suited in the posterior region of the mouth.
Conclusion
In recent years, there has been much progress in the development of new restorative adhesive materials, including both resin composites and glass ionomers. While some writers have argued that resin composites have advanced sufficiently such that there is no longer a need to use glass ionomers, the dental profession has seen recent developments in glass ionomers that call that view into question. A defining characteristic of new glass ionomer restorative materials is the chemical composition, which is beneficial for patients with high caries susceptibility.
References
1. Niederman R. Glass ionomer and resin-based fissure sealants - equally effective? Evid Based Dent. 2010;11(1):10.
2. Mickenautsch S, Yengopal V. Caries-preventive effect of glass ionomer and resin-based fissure sealants on permanent teeth: An update of systematic review evidence. BMC Res Notes. 2011;4:22.
3. Mickenautsch S, Yengopal V. Caries-preventive effect of high-viscosity glass ionomer and resin-based fissure sealants on permanent teeth: A systematic review of clinical trials. PLoS One. 2016;11(1). https://doi.org/10.1371/journal.pone.0146512. Accessed June 30, 2017.
4. Baroudi K, Rodrigues JC. Flowable resin composites: A systematic review and clinical considerations. J Clin Diagn Res. 2015;9(6):ZE18-ZE24.
5. Strassler HE. Glass ionomers for direct placement restorations. Dental Academy of CE website. http://www.ineedce.com/courses/2052/PDF/1104cei_glassionomer_web.pdf. Published 2011. Accessed June 30, 2017.
6. Graham L. Glass ionomers in modern clinical practice. Dentistry Today website. http://www.dentistrytoday.com/restorative-134/10272-glass-ionomers-in-modern-clincial-practice. Published February 28, 2017. Accessed June 30, 2017.
7. Anusavice KJ. Phillips’ Science of Dental Materials. United Kingdom: Elsevier Health Sciences; 2003:471-472.
8. Ahovuo-Saloranta A, Forss H, Walsh T, et al. Sealants for preventing dental decay in the permanent teeth (review). Cochrane Database Syst Rev. 2013;(3): CD001830. http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD001830.pub4/full. Accessed June 30, 2017.
9. Ngo HC, Mount G, McIntyre J, Tuisuva J, Von Dousse RJ. Chemical exchange between glass-ionomer restorations and residual carious dentine in permanent molars: an in vivo study. J Dent. 2006;34(8):608-613.
Steven Eisen, DMD, has worked 28 years in private practice. His interests include dental materials and educational research. Dr. Eisen has been published in the Journal of Dental Education, the Journal of Cosmetic Dentistry, and Compendium. He is a reviewer forthe Journal of Dental Education and has authored research abstracts with the International Association of Dental Research.
Gerard Kugel, DMD, PhD, MS, is a reviewer for the New England Journal of Medicine, the Journal of the American Dental Association, the Journal of Esthetic and Restorative Dentistry, and Clinicians Report. Dr. Kugel has his doctorate in dental materials and an executive certificate in management and leadership from the Massachusetts Institute of Technology Sloan School of Management.