The economic benefits of a single composite
Ian Shuman, DDS, MAGD, AFAAID
There are many direct composite materials available; however, few offer a majority of the characteristics sought by clinicians. Optimum composite restoratives are those that can be used in cases ranging from posterior Class Vs to anterior composite veneers. Having one type of composite resin offers economic benefits (i.e., a reduction in product overhead and waste) and adaptability in multiple restorative situations. It also means the clinician needs fewer shades on hand, and shades are less likely to expire before they are used or even opened.
There are composite resin systems with the clinical components and benefits sought by clinicians in a single product. One of those traits is sensitivity to photopolymerization. Some composites implement radical-amplified photopolymerization (RAP) initiator technology.1 This technology offers an increased working time under ambient light (90 seconds), with a decrease in curing time under halogen light (10 seconds).
Additionally, particle type, size, and shape have a direct effect on strength, durability, and polishability, among other attributes. For example, materials that contain a high percentage by weight of silica-zirconia filler show increased longevity and strength.2 Also, composites available in a multitude of shades in both syringes and preloaded tips are ideal.
Product waste is a very real problem for dentists. Running a practice is akin to managing a miniature hospital. Practice overhead must be managed, and material waste significantly reduced or eliminated. Ideally, 5% of a dental budget should be devoted to supplies.3 This figure can remain stable provided that inventory is under control. One way to manage the supply budget is by limiting the inventory needed per procedure, including direct composite restoration materials. By reducing product overhead, less waste is produced. In addition, with the right composite system, fewer shades are required—including rare shades that often expire prior to complete use or even use at all.
Case report No. 1
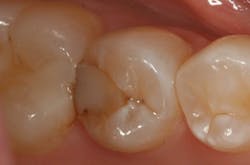
A failing disto-occlusal composite in the lower left second premolar was scheduled to be treated with a direct composite restoration (figure 1). After obtaining local anesthesia, the quadrant was isolated using a combined suction/retraction device. The existing restoration and caries were removed and a sectional matrix system used to restore the Class II cavity preparation.
Figure 1: The patient’s failing restoration
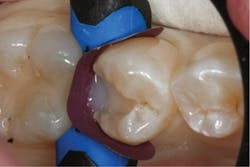
The cavity preparation was treated with a single-component light-cured dental adhesive (Bond Force, Tokuyama Dental). This was followed by restoring the base of the preparation with a universal supra-nano-filled flowable resin composite in shade A2 (Estelite Flow Quick, Tokuyama Dental; figure 2). Flowables are simply low-viscosity composites with less filler than universal (paste) composites. This gives flowables the ability to adapt to margins and preparation types that paste composites cannot. A study by Radhika et al. demonstrated that in the occlusal wall, packable composite showed significantly more marginal microleakage than the other groups. In the cervical wall, teeth restored with a flowable composite liner showed less marginal microleakage when compared to all other groups.4
Figure 2: Placement of flowable composite
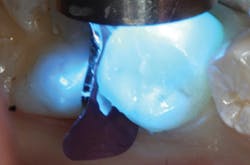
Figure 3: Curing final layers of composite
The remaining volume of the preparation was restored with a universal supra-nano-filled dental composite in shade A2 (Estelite Sigma Quick, Tokuyama Dental) using the oblique layering technique.
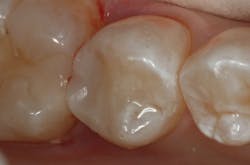
It has been shown that cuspal deflection resulting from polymerization shrinkage can be reduced by incremental filling techniques to obtain optimal clinical outcomes.1 In addition, since all composites shrink upon polymerization, the net effect of the directed shrinkage technique is to direct polymerization toward the tooth, improving adaptation to the preparation.1 Controlling the location of the curing light during initial curing accomplishes this (figure 3). The direct composite was completed by occlusal adjustment, and finishing and polishing of the restoration using silicone-impregnated rubber cups, points, and discs (figure 4).
Figure 4: The completed restoration
A clinical study over a five-year period evaluated over 2,800 Estelite Sigma Quick restorations for resistance to fracture and chipping, esthetics, resistance to marginal discoloration, wear resistance, and retention.2
According to the authors of the study, “Estelite Sigma Quick performed extremely well with regard to resistance to fracture and chipping.” 2.6% of the restorations had small chips, “but did not require replacement.” 1.2% of the restorations “fractured and were replaced. Many of the restorations replaced were large, and in several cases, the tooth fractured requiring the placement of a crown.”
The authors also stated that the “esthetics [were] excellent… the availability of many shades and opacities was extremely helpful in achieving long-lasting results.Most of the Estelite Sigma Quick restorations were bonded with sixth- or seventh-generation bonding agents. 97% of the restorations exhibited very slight or no microleakage at the margins at recall time. Estelite Sigma Quick maintained excellent wear resistance in both the anterior and posterior regions after five years in function. The wear on the opposing dentition was minimal. Retention was excellent. There were 33 debonds (2.2%) that involved facial/buccal surfaces. Debonding was more a function of the bonding agent and surface preparation and not the composite.”2
Case report No. 2
A patient presented with the chief complaint that her upper teeth were breaking (figure 5). This was due to a combination of medication-induced xerostomia, caries, and failing composite restorations. She had neglected to seek care due to the perceived financial expense. After reviewing possible treatment plans with the patient, it was decided that due to financial constraints, a direct restorative approach was the best option. After obtaining local anesthesia, the existing restorations and caries were removed (figure 6).
The cavity preparations were treated with Bond Force, a single component light-cured dental adhesive. This was followed by restoring the irregularities of the preparations using Estelite Flow Quick in dentin shade 0A2. The teeth were then individually restored using Estelite Sigma Quick in shade BW. These direct composite restorations were then completed by occlusal adjustment, and finished and polished using silicone impregnated rubber cups, points, and discs (figure 7).
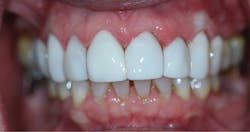
Figure 5: The patient’s breaking upper teeth
Figure 6: The patient’s upper teeth after removal of old restorations and caries
Figure 7: The completed restoration
References
1. Ilie N, Kreppel I, Durner J. Effect of radical amplified photopolymerization (RAP) in resin-based composites. Clin Oral Investig. 2014;18(4):1081-8.
2. Estelite Sigma Quick 5-year clinical performance report. The Dental Advisor. 2014.
3. Blatchford B. Percentage of overhead is a choice. Dental Economics website. http://www.dentaleconomics.com/articles/print/volume-99/issue-1/departments/flourishing-in-changing-times/percentage-of-overhead-is-a-choice.html. Accessed August 25, 2017.
4. Radhika M, Sajjan GS, Kumaraswamy BN, Mittal N. Effect of different placement techniques on marginal microleakage of deep class-II cavities restored with two composite resin formulations. J Conserv Dent. 2010; 13(1): 9-15.
Ian Shuman, DDS, MAGD, AFAAID, maintains a full-time general, reconstructive, and esthetic dental practice in Pasadena, Maryland. Since 1995 Dr. Shuman has lectured and published on advanced, minimally invasive techniques. He has taught these procedures to thousands of dentists and developed many of the methods. Dr. Shuman has published numerous articles on topics including adhesive resin dentistry, minimally invasive restorative dentistry, cosmetic dentistry, and implant dentistry. He is a fellow of the Pierre Fauchard Academy.
Editor’s note: This article is supported by Tokuyama Dental.