Endodontic treatment planning: Reading the signs
by Richard Mounce, DDS
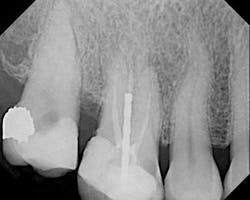
The female patient whose radiographic image appears in Figure 1 presented with a clinical history that is instructive with regard to endodontic diagnosis, treatment planning, and emergency management.
The patient said that the root canal in No. 3 was performed nine years ago. Approximately one month before she came to my office, she had increasing pain in the upper right that her general practitioner diagnosed as irreversible pulpitis in No. 2. Access was made at that time. The patient continued to have pain that became localized to No. 3. She also reported that the pulpotomy for No. 2 took approximately three hours and that the dentist had also seen other patients during the process. The patient found another general dentist who referred her to me.
Among other findings, No. 3 was sensitive to percussion and palpation. The tooth was not mobile and probing was approximately a six at the distal. The tooth had never been crowned. There was significant uncleaned and unfilled space in the root canal system, especially in the palatal and mesiobuccal roots. Recurrent decay was present at the mesial.
No. 2 had an access made through the occlusal and no discernable canals were visible in this or any of the radiographic angles. No. 2 was asymptomatic upon my examination. The patient’s medical history was noncontributory.
While much could be written of this clinical case, several observations can be made:
1) No. 2 is clinically a very difficult root canal due to the calcification and location of the tooth. For me, as an endodontist, this would have been a challenging case. A surgical operating microscope (SOM) would have been required to ideally determine the location of all canals (Global Surgical, St. Louis, Mo.). Significant time with hand files would have been required to gain patency once the canals were located. Rotary nickel titanium (RNT) files would have been contraindicated in this case until all the canals had at least a minimum No. 15 hand file diameter. After this minimal diameter was created, adroit RNT use would be required. Forcefully and rapidly inserting RNT files into this tooth without the required minimal diameter or even with it, likely would have led to iatrogenic outcomes.
2) No. 3 could either have been retreated or extracted. The post does not represent an obstacle to retreatment; it could have been easily removed with a Ruddle Post kit (SybronEndo, Orange, Calif.). It is unknown if the apex of the palatal and MB roots were blocked with debris. The treating clinician would have to be very careful not to propel debris down the canal system and accentuate any possible pre-existing blockages or transportations. After the gutta percha was removed, a viscous EDTA gel like File-Eze would be required to hold any canal debris in suspension and lubricate the canal system during initial negotiation (Ultradent, South Jordan, Utah). It cannot be taken for granted that the material in the canals is gutta percha, it could be a paste and require specialized techniques for removal. Once the material was removed, negotiation of the previously untreated space would require pre-curved hand files. Optimal pre-curving could be accomplished with the EndoBender pliers (SybronEndo). If the material were gutta percha, it would ideally be removed under the rubber dam and SOM with the heat source of the Elements Obturation Unit (SybronEndo) or with an RNT orifice opener such as the K3 Shapers (SybronEndo).
3) There was no evidence of vertical root fracture on No. 3. That said, whenever bone loss is present around a post and endodontically treated tooth, the real possibility of vertical fracture must be ruled out. A fistula, swelling, furcal bone loss, advanced mobility, and vertical probing defect disproportionate to other probings on the tooth are all indications of a vertical root fracture.
4) All things being equal, this tooth may ideally have been referred before access was made. Even if the patient exaggerated the time taken to treat it, it was an ordeal for her. While much could be written about this, suffice it to say that using an SOM and seeing just one patient at a time with a dedicated focus on access could have significantly reduced the time taken to perform the service and may have kept her trust.
I welcome your feedback ...
Dr. Richard Mounce offers intensive customized endodontic single-day training programs for small groups of one to two doctors. For information, contact Dennis at (360) 891-9111 or write [email protected]. Dr. Mounce lectures globally and is widely published. He is in private practice in endodontics in Vancouver, Wash.