Ask Dr. Christensen
by Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: patient information, dental treatment, teatment alternatives, implants, informed consent.
Q I have been told that the majority of lawsuits against dentists in the US are related to not informing patients about all of the treatment alternatives. What can I do to protect myself against this problem? How thoroughly should I inform patients?A Your information is correct. Many of the lawsuits against dentists are related to lack of "informed consent." Many dentists do not consider the need to educate patients before beginning treatment. They select the treatment plan which they feel is the most appropriate for the patient — and then perform the treatment — failing to provide the patient with other alternatives. If the treatment fails, they are highly liable for a lawsuit on the basis of lack of informed consent about the other alternatives.Informed consent
What is informed consent? Our legal consultants have provided us with defined informed consent criteria. If all of these informed consent characteristics are included in the patient's education before treatment, there is no need to worry. What follows is a discussion of the characteristics of adequate informed consent and some information about each of them.
1. Treatment Alternatives: Patients need to be informed about all of the treatment alternatives for their specific problem. As an example,the following are treatment alternatives for one missing upper lateral incisor tooth:
- A three-unit fixed partial denture
- A two-unit cantilever fixed-partial denture, supported by the canine, as a replacement for the lateral incisor.
- An implant, abutment, and a crown in the missing tooth area
- A metal-supported removable partial denture
- A nonmetal containing resin-removable partial denture
- An acid-etched, resin-cement retained, ceramic fixed partial denture bonded to the lingual of the canine and the central incisor
- An acid-etched, resin-cement retained, porcelain-fused-to-metal fixed partial denture bonded to the lingual surfaces of the canine and the central incisor
- Doing nothing at all
All of these treatments must be explained to the patient to satisfy informed consent. These alternatives can easily be shown to the patient using some of the patient education programs readily available through many sources, including my own organization.
2. Advantages of Each Alternative: There are known advantages to each alternative. Using the previous example, ask yourself what are the advantages of a crown supported by an implant?
- It is not necessary to remove tooth structure from the teeth adjacent to the missing tooth.
- The implant feels similar to the patient's own tooth after the surgery has healed.
- The crown placed on the implant looks, feels, and chews like a normal tooth.
Obviously, this choice will probably be the patient's preference if it can be done. The advantages of the other potential treatments need to be discussed also.
3. Disadvantages of Each Alternative: Continuing with the example, what are the disadvantages related to placing an implant-supported single crown? Surgical placement of the implant is required, which may or may not be painful. There also is the possibility of negative events occuring during and after the surgery. The procedure is expensive, and there are some surgical risks involved. There is a four-to-six-month osseointegration period required for some implants before the crown can be placed, during which time the patient wears some type of provisional restoration. The disadvantages of all of the other treatment possibilities must also be explained to the patient.
4. Risks of Each Alternative: The surgical risks of placement of an implant include the potential of short-term bruising of the external facial tissues; paresthesia for an indefinite time or even permanently; infection in the implant site; failure for the implant to osseointegrate, and others. These risks should be tactfully explained to the patient. The risks of all of the other alternatives also need to be explained.
5. Costs of Each Alternative: Many patients know nothing about the cost of oral procedures. The cost of each procedure must be stated in comparative terms. Currently, an average implant placement costs about $1,800. An average abutment cost is about $400, and the final crown costs about $1,000, for a total of approximately $3,200. Unless these costs are explained and compared to the costs of the other alternatives, a lawsuit may be imminent if the patient suffers a failure of the implant treatment.
6. Result of Doing Nothing at All: If you do not tell patients what will happen if they do not have any treatment done, you are being negligent. In the case of the missing anterior tooth, the adjacent teeth will collapse toward the edentulous space, the space between the teeth will become smaller, and the bone in the edentulous space will continue to resorb and shrink, making an implant difficult to place at a later time.
How, when, and where does all of this education take place? May I suggest that almost all of it can be accomplished by an educated, competent, motivated staff member using educational DVDs, slides, printed pieces, books, intraoral television, casts of the patient's mouth, digital photos, and other methods.
At the completion of the patient data collection and education appointment, the dentist should come into the operatory, listen to patient questions, summarize the information that the staff person has provided, and obtain a signed informed-consent document concerning the treatment to be performed and the education the patient has received.
If all of these steps are taken before any treatment is started, you have satisfied the informed consent criteria. Now it is up to you to provide adequate therapy.
There are many patient education aids available in the profession. Among them is our own avoiding malpractice package. The Practical Clinical Courses package includes everything necessary to satisfy informed consent. It contains:
- A DVD with 14 separate, short, descriptive presentations on it.
- A book titled "Consumers Guide to Dentistry."
- A booklet that includes many pages of dental documents to educate patients.
- A video on avoiding malpractice suits.
Any or all of these items are available to assist you. Please contact Practical Clinical Courses at (800) 223-6569 for more information or go to our Web site at www.pccdental.com.
Q Enamel bonding values are always reported to be lower than dentin bonding values. Is this difference significant? What is a predictable bonding technique to produce the best enamel and dentin bonds?A The value differences are not clinically significant. Actually, enamel bonds are far longer lasting than dentin bonds.I have two nearly foolproof techniques that will eliminate the worry about postoperative tooth sensitivity and enamel and dentin bonding for resin-based composite restorations. Both techniques are predictable, effective, and simple to accomplish.
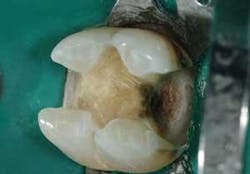
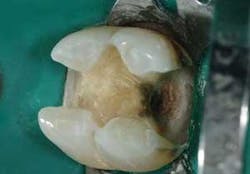
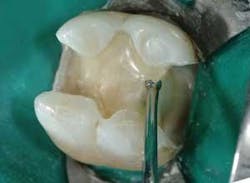
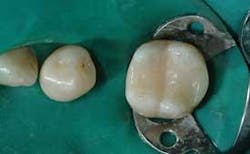
Technique 1 (see Figures 1, 2, and 3). This is my personal favorite technique.
- Etch the enamel margins with a phosphoric acid gel.
- After the appropriate etch time, wash off the acid gel rapidly to avoid getting the acid on the dentin of the tooth preparation.
- Place a desensitizing/disinfecting solution such as GLUMA (Heraeus Kulzer) on the tooth preparation.
- Place a thin layer (0.5 to 0.75 mm) of resin-modified glass ionomer (RMGI) on the deepest dentin areas of the tooth preparation. (Vitrebond™ Plus from 3M ESPE or Fuji Lining LC from GC).
- Cure the RMGI, remembering that it will not have its full strength until the glass ionomer portion of the RMGI completes its chemical set many hours later.
- Use a self-etching primer over the entire tooth preparation. Research shows that the previous acid etch of the enamel is not adversely influenced by the self-etch primer application. The most popular self-etch primer is Clearfil SE Bond from Kuraray, but many other bonds are very acceptable also.
- Place the restorative resin in increments of no more than 2 mm at a time, curing each increment after placement.
- Finish the restoration.
Technique 2 (This is the most popular technique)
- Etch the enamel margins with a phosphoric acid gel.
- After the appropriate etch time, wash off the acid gel rapidly to avoid getting the acid on the dentin portion of the tooth preparation.
- Place a desensitizing/disinfecting solution such as GLUMA (Heraeus Kulzer).
- Place a self-etching bonding agent of your choice. The most popular brand is Clearfil SE from Kuraray, but many other bonds are very acceptable also.
- Test your flowable resin to see if it is highly radiopaque. If it is not highly radiopaque, get another brand. Among the most radiopaque brands is Tetric Flow from Ivoclar Vivadent.
- Place a thin layer of a radiopaque flowable resin.
- Cure the flowable resin.
- Place another layer of flowable and cure it.
- Place the restorative resin in increments of no more than 2 mm at a time, curing each after placement.
- Finish the restoration.
Either of these two techniques will produce sensitivity-free restorations with an optimum bond to enamel and dentin. However, many other techniques will also produce very acceptable restorations.
Our video, V3519 "Predictable, Nonsensitive, Resin-Based Composite Restorations," demonstrates each of these techniques. Please contact Practical Clinical Courses at (800) 223-6569 for more information or go to our Web site at www.pccdental.com.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and Dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.