Vaping and oral health: It’s worse than you think
Scott Froum, DDS
Alisa Neymark, DDS
The use of electronic cigarettes (e-cigarettes) represents a significant and increasing proportion of tobacco consumption, posing a tremendous threat to oral health. This article will look at the following aspects of e-cigarettes:
• Overview of e-cigarette usage
• Statistics on the current prevalence of e-cigarettes
• Three chemicals contained in e-cigarettes and their effects on oral health
When compared to traditional tobacco use, an argument that e-cigarette use may be as dangerous to oral health—if not more dangerous—can be made.
Overview
Using e-cigarettes, referred to as vaping, works by heating a liquid to generate an aerosol that the user inhales. The liquid in the e-cigarette, called e-liquid, usually consists of propylene glycol, glycerin, flavorings, water, and nicotine, although some users will substitute THC for nicotine. In practice, e-cigarette users tend to reach lower blood nicotine concentrations than tobacco smokers, although it is difficult to make a direct comparison because nicotinee-cigarette concentrations vary widely.
Reasons individuals vape include:
• Smoking cessation
• The thought that vaping is less harmful than cigarettes
• Circumvention of smoke-free areas
• Recreational enjoyment1
Prevalence
Researchers and antitobacco advocates are especially concerned that irresponsible marketing has made e-cigarettes appeal to the segment of the young population that had no history of tobacco usage and never intended to start smoking. Because of the known dangerous effects of traditional tobacco methods, use among middle and high school students has been steadily decreasing since 2014. However, since the introduction of the e-cigarette, that number is now increasing, and it is estimated that one in five high school students may now be using tobacco products.2
E-cigarette use from 2017 to 2018 increased 78% among high school students and 48% among middle school students.3
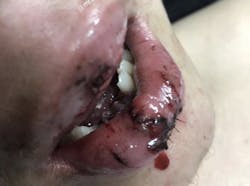
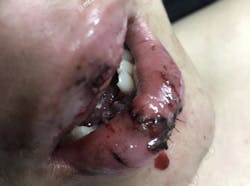
Figure 1: Oral soft-tissue injuries due to e-cigarette explosion (photo courtesy of Nicole Angemi)
Propylene glycol
The first danger of e-cigarettes is associated with the carrier product known as propylene glycol (PG). PG is primarily used in the production of polymers and in food processing. It can be found in various edible items, such as liquid sweeteners, ice cream, and whipped dairy products. It can also act as a carrier for various inhalant pharmaceutical products, including nicotine. PG is a viscous, colorless liquid that possesses a faintly sweet taste and is one of the major ingredients of the e-liquid used in e-cigarettes. When used orally, the breakdown products of PG include acetic acid, lactic acid, and propionaldehyde, which are all toxic to enamel and soft tissue.4 In addition, PG is a hygroscopic product, which means water molecules in saliva and oral tissue will bond to the PG molecules, leading to tissue desiccation.5 The result of this is xerostomia, or “dry mouth,” which has been shown to lead to an increase in cavities, gum disease, and other oral health issues.
Vegetable glycerin and flavorings
The second danger of e-cigarettes is due to other major components of e-liquid: glycerin and flavorings. Vegetable glycerin (VG) is a colorless, odorless, viscous, and sweet-tasting liquid. It has a myriad of applications, including medical, pharmaceutical, and personal care. In the food industry, it serves as a humectant, solvent, and sweetener. It is 60% as sweet as sucrose and is not metabolized by cariogenic bacteria, and is, therefore, not thought to cause cavities. However, studies have shown that the combination of VG with flavorings produces a fourfold increase in microbial adhesion to enamel and a twofold increase in biofilm formation.6 In addition, a 27% decrease in enamel hardness was demonstrated when flavorings were added to e-liquid as compared to unflavored controls. The viscosity of the e-liquid also allowed Streptococcus mutans to adhere to pits and fissures. In other words, e-liquid allows more cavity-causing bacteria to stick to a softer tooth and can lead to rampant decay.
Nicotine
Another danger associated with e-cigarettes has to do with nicotine. Although the percentage of nicotine is much lower (0.3%–1.8%) than in traditional tobacco products, one electronic cartridge (200–400 puffs) can equal the smoking of two to three packs of regular cigarettes. The dangerous effects of nicotine on gum tissue are well known. The literature suggests that nicotine affects gingival blood flow as it is a vasoconstrictor. It also affects cytokine production, neutrophil function, and other immune cell function.7 In addition, nicotine decreases connective tissue turnover. All of this results in a much higher chance of developing gum disease and tooth loss.
Figure 2: Effects of e-cigarette usage
Lithium batteries
Recently, a 24-year-old man from Texas was killed when his vape pen exploded, and part of the device wound up severing his jugular vein.8 Although these types of sensationalized deaths are rare with e-cigarettes and vaping pens (only two reported to date), the explosions of these pens are not. The problem lies within the vape pen and the lithium batteries overheating and exploding. These explosions are usually attributed to improper charging of the device or have been linked to a type of device called a mechanical mod that has no internal safety and can overheat and explode.
One report found that 195 of these adverse events occurred between the years of 2009 and 2016.9 However, Dennis Thombs, dean of the School of Public Health at UNT Health Science Center, published a study that concluded the number of vape explosions in the US were most likely underestimated. Thombs estimated that there were 2,035 e-cigarette explosions and burn injuries in the US between 2015 and 2017—more than 40 times the initial estimate by the US government.8 These injuries are serious and often lead to disfigurement of oral soft tissue (figure 1).
Bottom line
The bottom line is vaping can be just as dangerous, if not more dangerous, when compared with smoking. The problem is that vaping is thought to be a safer alternative to traditional tobacco products, and companies are adding flavoring products to attract younger generations. According to a 2013–2014 survey, 81% of current youth e-cigarette users cited the availability of appealing flavors as the primary reason for use.10
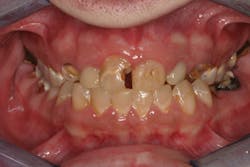
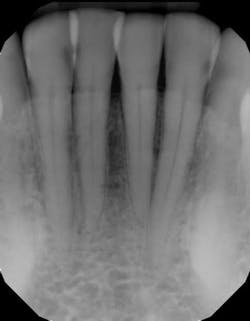
For example, one patient of a general dental practice had a caries-free history for 35 years. He ceased smoking traditional cigarettes and decided to vape as he thought this was a healthier alternative. Within a year, cervical enamel demineralization and interproximal lesions were present on the mandibular anterior sextant, consistent with the primary point of contact of the e-liquid aerosol (figure 2).
Figure 3: Effects of e-cigarettes
In another example, a young patient had been using e-cigarettes for five years. He started vaping as a method to quit smoking traditional tobacco products thinking vaping was a healthy alternative. Because of its ease of use, he smoked a cartridge of one of the more popular vaping products a day. Admittedly, he also drank energy drinks (high sugar content), stating that his mouth was often dry after vaping. This combination led to rampant decay with smooth-surface lesions and future tooth loss (figure 3).
Many advocates of vaping claim that e-cigarette use and vaping poses 5% the health risks of traditional tobacco smoking and claim its use to be helpful in getting people to quit.11 This particular use does have merit and has helped many individuals quit smoking. Unfortunately, these studies have only analyzed e-cigarette use in former smokers using vaping as a way to stop smoking. The studies have not looked at the health effects of nonsmokers who start vaping because of the perceived innocuous health effects and because it “tastes yummy.” In addition, these studies have not looked at vaping in middle school and high school individuals, the group where e-cigarette use is increasing the most in percentage of use. Because of this, a tidal wave of oral health problems is heading our way.
References
1. Tsai J, Walton K, Coleman BN, et al. Reasons for electronic cigarette use among middle and high school students—National Youth Tobacco Survey, United States, 2016. MMWR Morb Mortal Wkly Rep. 2018;67(6):196-200. doi:10.15585/mmwr.mm6706a5.
2. Wang TW, Gentzke A, Sharapova S, Cullen KA, Ambrose BK, Jamal A. Tobacco product use among middle and high school students—United States, 2011–2017. MMWR Morb Mortal Wkly Rep. 2018;67(22):629-633. doi: 10.15585/mmwr.mm6722a3.
3. Cullen KA, Ambrose BK, Gentzke AS, Apelberg BJ, Jamal A, King BA. Notes from the field: use of electronic cigarettes and any tobacco product among middle and high school students—United States, 2011–2018. MMWR Morb Mortal Wkly Rep. 2018;67(45):1276-1277. doi:0.15585/mmwr.mm6745a5.
4. Ruddick JA. Toxicology, metabolism, and biochemistry of 1,2-propanediol. Toxicol Appl Pharmacol. 1972;21(1):102-111.
5. American Medical Association. AMA Department of Drugs. AMA Drug Evaluations. 3rd ed. Littleton, MA: PSG Publishing Co., Inc.; 1977:656.
6. Kim SA, Smith S, Beauchamp C, et al. Cariogenic potential of sweet flavors in electronic-cigarette liquids. PLoS One. 2018;13(9):e0203717. doi: 10.1371/journal.pone.0203717.
7. Malhotra R, Kapoor A, Grover V, Kaushal S. Nicotine and periodontal tissues. J Indian Soc Periodontol. 2010;14(1):72-79. doi:10.4103/0972-124X.65442.
8. E-cigarette explosion kills Texas man. Beasley Allen Law Firm website. https://www.beasleyallen.com/news/e-cigarette-explosion-kills-texas-man/. Published February 5, 2019.
9. Electronic cigarette fires and explosions in the United States 2009–2016. Lawrence A. McKenna Jr. Research Group. National Data Fire Center. United States Fire Administration. U.S. Department of Homeland Security. https://www.usfa.fema.gov/downloads/pdf/publications/electronic_cigarettes.pdf. Published July 2017.
10. Villanti AC, Johnson AL, Ambrose BK, et al. Flavored tobacco product use in youth and adults: findings from the first wave of the PATH Study (2013-2014). Am J Prev Med. 2017;53(2):139-151. doi:10.1016/j.amepre.2017.01.026.
11. Nicotine without smoke: Tobacco harm reduction. Royal College of Physicians website. https://www.rcplondon.ac.uk/projects/outputs/nicotine-without-smoke-tobacco-harm-reduction-0. Published April 28, 2016.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a newsletter for dentists and hygienists that focuses on periodontal- and implant-related issues. Perio-Implant Advisory is part of the Dental Economics and DentistryIQ network. To read more articles, visit perioimplantadvisory.com, or to subscribe, visit dentistryiq.com/subscribe.
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of the American Board of Periodontology, is a clinical associate professor at SUNY Stony Brook School of Dental Medicine in the Department of Periodontology. He serves on the board of editorial consultants for the Academy of Osseointegration’s Academy News. Contact him through his website at drscottfroum.com or (212) 751-8530.
Alisa Neymark, DDS, graduated with a Bachelor of Arts in anthropology and biology from Amherst College, and then pursued her dental degree at Stony Brook School of Dental Medicine. Upon completion of a two-year residency at Long Island Jewish Medical Center, she has been in private practice both on Long Island and in Brooklyn. Dr. Neymark practices with an emphasis on cosmetic dentistry and restoring implants.