Wake up: Sleep could be making your patients sick
Ashley Spooner, DDS
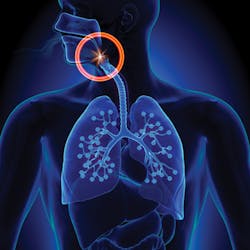
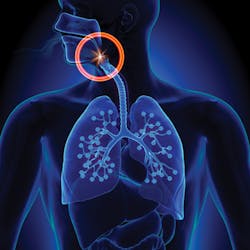
Sleep is essential for our bodies to survive. The consequences of sleep deprivation are serious and can be life-threatening when left untreated. Obstructive sleep apnea (OSA) affects an estimated 30 million Americans, and roughly 80% of cases remain undiagnosed.1 OSA is connected to numerous life-threatening health conditions, including high blood pressure, heart disease, diabetes, depression, insomnia, and asthma. As dentists, we can look for symptoms and risk factors that can help screen for this treatable condition. By understanding how we can support screening and treatment, we can better help our patients avoid these consequences.
© Decade3d | Dreamstime.com
Understanding OSA
OSA is a disease of the collapsibility of the upper airway. When the upper airway collapses during sleep, a partial or full obstruction may occur, causing a decrease in blood oxygen saturation because the person has stopped breathing, much as if holding his or her breath under water. Depending on the severity, a person may have multiple apneic events that each last seconds to over a minute. When this continues repeatedly throughout the night, the body is in a constant fight-or-flight mode trying to survive on the reduced oxygen it is receiving. Another concerning result is that the repetitive interruptions in breathing cause sleep fragmentation associated with hypoxia. This lack of oxygen provokes overnight hypertension and can lead to irregular heartbeat, heart attack, stroke, and even sudden death.2
Studies show that chronic restriction of sleep characterized by less than seven hours per night leads to significant cognitive dysfunction and can also have negative effects on hormone and metabolic function and inflammatory responses.3 This constant fight-or-flight mode causes a hormonal imbalance, which leads to an abundance of cortisol and a decrease in glucose tolerance. This results in inflammation, water retention, and fat storage. People may notice weight gain despite a good diet and exercise, and difficulty losing weight. Finally, the antibody activity in the body decreases because the body is putting its energy into keeping the tissues oxygenated. This can lead to getting sick more often and difficulty recovering.
Without a proper diagnosis, the body remains in a constant state of stress, affecting the condition of the heart and even leading to death.
Screening for OSA
Many factors are considered when screening patients for OSA. During the patient exam, we can look for a high palatal vault, narrow arches, crowded teeth, a large tongue that sits above the lower teeth, permanent teeth extractions for orthodontics, and how the back of the throat looks. For example, can we see past the tongue to where the tonsils are located? Are the tonsils large and inflamed? In children, we can also look for developmental factors regarding how their jaws relate and if they have any trouble with speech. Other factors to look for in children are whether they are underweight or underdeveloped. These physiological factors suggest that the space for air to flow is constricted, and if the patient has a collapsible airway as well, OSA may be present.
Once we see the physical signs of potential sleep-disordered breathing, we can ask the patient questions related to daytime sleepiness, headaches, night sweats, nighttime restroom use, bed wetting, and overall mood and feeling throughout the day. We can also ask adults if they sleep in the same room as their spouse or if snoring has become disruptive. Snoring is not always present in OSA but is one of the leading symptoms. When the patient’s responses are consistent with symptoms of OSA, we can recommend a sleep wellness exam for adults aged 18 and older and refer children to a sleep physician who specializes in pediatric care.
A sleep wellness exam consists of using a rhinometer and pharyngometer to test the airflow through both nostrils and the collapsibility of the airway. This is a simple test that only requires the patient to breathe. The data can be collected and the results can be compared to the parameters set forth by the American Academy of Sleep Medicine. If the patient meets these parameters, a sleep study is recommended to diagnose possible OSA. There are sleep study devices that can be sent home with the patient, or we can refer them to a sleep center. Once the sleep study is completed, it is read and diagnosed by a board-certified sleep physician.
Treating OSA
OSA is characterized as mild, moderate, or severe based upon how many apnea or hypopnea events the patient has per hour, known as the apnea-hypopnea index (AHI). Mild OSA is an AHI of 5–14, moderate OSA is 15–29, severe OSA is an AHI equal to 30 or more.4 Once the diagnosis is made, the board-certified sleep physician will prescribe the best treatment for each patient. Patients who have severe OSA are most often prescribed continuous positive airway pressure (CPAP), positive airway pressure (PAP), or auto-PAP machines. Some are continuous forced air, and some adjust throughout the night based on the needs of the patient. Although CPAP is the gold standard for OSA treatment, only 6% of those who have them are compliant.2 Patients report that CPAPs may be uncomfortable or difficult to travel with, or may experience other side effects.
For patients with mild to moderate OSA, oral appliance therapy is very effective and is proven to be more comfortable for patients, often resulting in greater compliance.2 Oral appliance therapy is also effective in cases of severe OSA where a patient cannot tolerate a CPAP. As dentists, we can support the treatment of OSA by creating an oral appliance that is worn at night to stabilize the collapsibility of the upper airway.
In children, treatment can be a little different. Children are still growing, so we can often impact the airway positively by removing adenoids, expanding the arches through orthodontics, and through occasional steroids if they have trouble breathing through their nose. Sometimes a nasal cannula or CPAP is recommended for children as well depending on the severity and root cause of the apnea.5
Everyone deserves a good night’s sleep. By understanding OSA, screening our patients, and offering oral appliance therapy where appropriate, we can help reduce the incidence of undiagnosed OSA and support our patients in living longer, healthier, and happier lives.
References
1. Hidden Health Crisis Costing America Billions: Underdiagnosing and Undertreating Sleep Apnea Draining Healthcare System. American Academy of Sleep Medicine website. https://aasm.org/advocacy/initiatives/economic-impact-obstructive-sleep-apnea/. Published 2016. Accessed February 5, 2019.
2. Van Haesendock G, Dietljens M, Kastoer C, et al. Cardiovascular benefits of oral appliance therapy. J Dent Sleep Med. 2015; 2(1):9-14.
3. Banks S, Dinges DF. Behavioral and physiological consequences of sleep restriction. J Clin Sleep Med. 2007;3(5):519-528.
4. Apnea: Understanding the Results. Division of Sleep Medicine at Harvard Medical School website. https://ca.edubirdie.com/blog/sleep-apnea-diagnosing-osa-understanding-results
5. Tan HL, Gozal D, Kheirandish-Gozal L. Obstructive sleep apnea in children: A critical update. Nat Sci Sleep. 2013;5:109-123.
Ashley Spooner, DDS, graduated from University of Colorado School of Dental Medicine and is a practice owner supported by Pacific Dental Services in Highlands Ranch, Colorado. She currently serves as faculty of the PDS University Institute of Dentistry.