Bulk-fill resins: A viable option in dentistry’s armamentarium
Jeff Lineberry, DDS, AAACD, FAGD, FICOI
In dentistry, restorative materials—direct and indirect—have rapidly evolved over recent years and continue to change at an incredible rate. Looking further back at materials in the late 1700s and early 1800s, we had only gold and amalgam to choose from. Resin-based light-cured resins finally hit the market in the 1970s, over a hundred years later, and due to high patient demand and technology, have quickly grown into one of the largest and most widely used groups of restorative material today in less than half the time. And with technology, these materials are rapidly evolving to be more predictable and user friendly than ever.
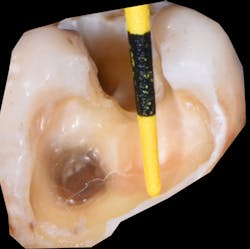
Figure 1: Proximal boxes in Class II restorations can be several millimeters deep.
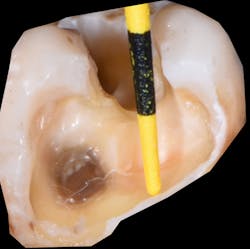
Historically, composite resins have been classified primarily based on the particle size in the filler: macrofill, microfill, hybrid, microhybrid, nanofill, and nanohybrid. And, depending on the amount of filler load, there are the standard “packable” or normal viscosity resin and flowable resins that are more fluid in nature. Typically, when placing resin into a cavity preparation, especially in Class I and Class II preparations, careful attention is needed in the overall placement, as many of these preparations can be several millimeters in depth (figure 1) and too deep for sufficient penetration of light (figure 2) and proper curing of the resin.
Figure 2: Curing lights can only penetrate a few millimeters before the intensity drops off quickly.
To overcome this issue, a technique was developed for placing composite resin in 2 mm increments. The other issue that arose when placing large amounts of composite resin was concern about polymerization shrinkage, leading to microgap formation and, ultimately, early failure of the restoration, especially in the gingival margin area.
Bulk-fill resins were developed to overcome some of these challenges with resin placement and to enable “bulk-fill” cavity preparations. Bulk-fill resins are not new to dentistry; they’ve actually been around for quite some time. With new technology, however, there is a renewed interest and growth in this area of restorative materials.
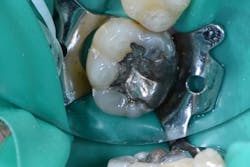
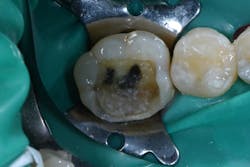
Figure 3: Existing No. 30 OL amalgam with recurrent decay
Benefits to bulk fills
With the light-curing depth restrictions on conventional resins, bulk-fill resins were developed primarily with the intention of overcoming these limitations and making placement quicker and more predictable. In general, bulk-fill resins can be cured to a depth of 4 mm (and in some cases, greater than 4 mm), allowing the dentist to place twice as much material and cure it in the same amount of time. Most manufacturers have accomplished this by creating more translucent materials. A recent article1 reviewing literature overall confirms that light penetration and adequate curing to 4 mm is possible in bulk fills, but it is essential to have an LED curing device with ≥1,000 mW/cm2 and 20 seconds of exposure time.
Potential concerns with bulk fills
Not all bulk-fill resins are the same when it comes to overall physical properties. Hence, it is wise to recognize when and where these materials come into play. Some of these materials are specifically designed as “liners” only and were not designed to withstand the occlusal stress and forces if placed in a stress-bearing area. It is important to be familiar with the manufacturer’s recommendation of use for its product.
When it comes to color matching and the ability of bulk-fill resins to blend with surrounding tooth structure, it is more challenging as they are typically more translucent in nature to allow greater light transmission for light curing. Since bulk fills were designed for restoring posterior teeth, this should not be an issue when used appropriately.
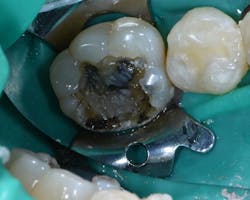
Figure 4: After initial amalgam removal. Note recurrent decay.
Other concerns with using bulk-fill resins are overall polymerization shrinkage and microgap formation. However, a recent benchtop study2 was completed, and it showed that gingival microleakage of bulk-fill resins and conventional composite resins was comparable. Another study3 suggests that shrinkage stress and overall elastic modulus is equal to or less than conventional composite resin, especially when placed in larger increments. Of course, these are benchtop studies, and there are limitations and relevance to clinical significance, but studies4,5 suggest bulk-fill resins have similar clinical performance and overall survivability.
Figure 5: After complete removal of decay to sound dentin
Case study
A 50-year-old male patient presented for restoration on tooth No. 30 that was found on a recent exam to have recurrent decay (figure 3). The patient’s medical history was unremarkable. He was having no pain or sensitivity. Although the existing restoration was large, and the possibility of indirect restorations was discussed, the patient was only interested in a direct resin restoration.
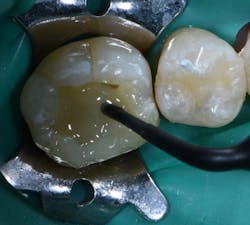
Figure 6: G-ænial Bulk Injectable (GC America) A2 being used to fill majority of preparation
The patient was anesthetized and tooth No. 30 was isolated with a rubber dam. The existing amalgam restoration was removed (figure 4) as well as all of the carious dentin (figure 5). A selective-etch technique was used, and the tooth was thoroughly rinsed. A copious amount of bonding agent was placed (G-Premio Bond, GC America) and lightly air dried and light cured. The lingual wall was built up using a regular-viscosity resin (G-ænial Sculpt, GC America) and light cured. The remaining portion of the cavity preparation was filled with G-ænial Bulk Injectable (GC America) within 1 mm of the occlusal margin and cured (figure 6). A final layer of G-ænial Sculpt was placed and cured. Initial polishing and shaping were completed prior to rubber dam removal, and then the occlusion and final polish were completed (figure 7).
Figure 7: Immediate post-op
Conclusion
Practitioners should continually evaluate products to help with overall efficiency in the office and also to improve overall patient care. Not only have bulk-fill resins been on the market for some time, but they are continually evolving and are proving to be a viable option for making posterior direct restorations more efficient and predictable for the doctor and the patient.
References
1. Lima RBW, Troconis CCM, Moreno MBP, Murillo-Gómez F, De Goes MF. Depth of cure of bulk fill resin composites: A systematic review. J Esthet Restor Dent. 2018;30(6):492-501. doi:10.1111/jerd.12394.
2. Behery H, El-Mowafy O, El-Badrawy W, Nabih S, Saleh B. Gingival microleakage of class II bulk-fill composite resin restorations. Dent Med Probl. 2018;55(4):383-388. doi:10.17219/dmp/99264.
3. Rizzante FAP, Mondelli RFL, Furuse AY, Borges AFS, Mendonça G, Ishikiriama SK. Shrinkage stress and elastic modulus assessment of bulk-fill composites. J Appl Oral Sci. 2019;27:e20180132. doi:10.1590/1678-7757-2018-0132.
4. Heck K, Manhart J, Hickel R, Diegritz C. Clinical evaluation of the bulk fill composite QuiXfil in molar class I and II cavities: 10-year results of a RCT. Dent Mater. 2018;34(6):e138-e147. doi:10.1016/j.dental.2018.03.023.
5. Veloso SRM, Lemos CAA, de Moraes SLD, do Egito Vasconcelos BC, Pellizzer EP, de Melo Monteiro GQ. Clinical performance of bulk-fill and conventional resin composite restorations in posterior teeth: a systematic review and meta-analysis. Clin Oral Investig. 2019;23(1):221-233. doi:10.1007/s00784-018-2429-7.
Jeff Lineberry, DDS, AAACD, FAGD, FICOI, is in private practice in Mooresville, North Carolina. He is an accredited member of the American Academy of Cosmetic Dentistry, a visiting faculty member and online contributor/author at Spear Education, a faculty assistant at the Pankey Institute, and a member of the Dental Products Report Editorial Advisory Board. He lectures on cosmetic and restorative dentistry, occlusion, TMD, and complex treatment planning. Email [email protected].