"Speed bump" or not, take a complete health history!
The statement, "The complete health history isn't needed until major treatment begins" in Dr. Blatchford's article, "Eliminate the speed bumps!" (August 2002 Dental Economics), is a misstatement. If you do not take a complete health history, you will be opening the door to a malpractice lawsuit. I do not know what Dr. Blatchford considers "major treatment," but even periodontal probing on a patient who has a severe heart murmur requiring premedication — which would be unknown without a health history — can lead to severe medical and legal problems.
"Speed bump" or not, you must take a complete health history prior to diagnosing and treating a patient. An occlusal restoration on a mandibular molar requiring an inferior alveolar block on a patient taking coumadin, or even a daily aspirin, could result in obvious severe problems if you do not know the patient's medical history.
As an expert witness and a practice-management consultant, I know of many situations that can lead to severe medical and legal problems for dentists who do not take a complete health history prior to treating a patient.
You cannot build a trusting relationship with patients if you don't care about their medical health. Almost all patients appreciate my inquiry into their health history, because it shows I truly care about their health and not just their teeth.
Let's move out of the era of "tooth fixers" and become true health-care providers who care for a patient as a person, not just another mouth.
Joseph P. Graskemper, DDS, JD, FAGD, FAES, FICOI, FASO
Bellport, N.Y.
Don't lecture us
I have just finished reading Dr. Sweet's Viewpoint, "Rush to Judgment" (August 2002 Dental Economics), regarding dentists' rush to judgment that posterior composites do not work, but when done properly, they do.
Although I appreciate the point that Dr. Sweet is trying to get across, I think that amalgam gets a bad rap. The point is made in the article that we should not be using a hazardous material in the mouth. I agree. However, until we find a suitable, predictable, long-last
ing substitute, I will continue to use amalgam in restorations that I know will fail with a composite resin.
My question regarding composite resin has always been that if it is such a wonderful material, why does the oral cavity work so hard to reject it? Just because something is white and pretty does not make it the solution. I have gone to lecture after lecture to learn how to master the technique for posterior resin placement. These lectures are always full, because we are all looking for the answer. I have etched long and etched short; I have overdried the tooth and left it wet; I have placed no liner and have placed liner; I have placed a lot of bonding agent and a little; I have cured in increments and cured in bulk; I have cured right over the restoration and cured from the sides; I have done direct and done indirect ... and the list goes on. No matter what I have done, I do not get the same predictability that I do with amalgam. I do not consistently get the same margins or contacts that I do with amalgam.
As far as the fractures, we are told repeatedly by the anti-amalgam crusade that they are caused by amalgam. I am not denying that this can be true. However, invariably we are talking about teeth that had deep decay and restorations that were done years ago. The teeth have weak walls and they fracture. I have seen this happen with large composite restorations as well. Let's also see how well these large resin restorations do over a 30-year period, like amalgams, before we lead the cheers about posterior composite resins preventing fractures. In fact, it is now becoming better known that whereas amalgam causes fractures due to its expansion over time, resins cause fractures by shrinking over time, thereby pulling those walls in.
I probably do about 70 percent of my posterior restorations with composite resin. But I just do not think it is fair that Dr. Sweet and others justify their claims by implying that if I do an amalgam on a patient, I am not looking out for his best interests. Sometimes amalgam is the best material of choice. I, for one, do not look down on another dentist because he does amalgams and does not appreciate the use of posterior resins, because I can empathize with him.
I am a good dentist and am always striving to improve. There is a learning curve with any technique, but the learning curve for posterior composites is huge. It still has a long way to go. Until we all are able to place a restorative material that is nontoxic, predictable, reliable, easy-to-use, and long-lasting, please don't lecture that those of us who still do amalgams are doing a disservice. Which is the better service: To place a composite restoration that is so sensitive that the patient ends up getting root canal treatment? Or to place an amalgam with a nice IRM base that sedates the tooth and works immediately?
Michael F. Cronin, DDS
Leominster, Mass.
Dropping Delta is a good decision!
I read Dr. William Hsiang's Viewpoint (September 2002 Dental Economics) regarding him dropping Delta Dental insurance. Good decision! We mailed our "drop Delta letter" today! We have been members for 16 years, and it took five years to finally drop it. It is a difficult decision, but the correct one to make.
Dentists must evaluate whether maintaining a relationship with Delta is a good dental business decision or not. Delta does not seem to have the best interests of the patient or the dentist in mind. Dropping Delta is a good business decision for our office. We are relieved to be free from their restrictions, loopholes, and low fees.
Being independent of PPOs is an excellent decision for dentists, patients, and the future of dentistry.
Dr. Ginny Murtaugh
Laguna Niguel, Calif.
Clarification
With the September 2002 issue of Dental Economics, a supplement about the CEREC Symposium 2002 was attached. One of the articles published in the supplement was titled, "The Clinical Efficacy of CEREC Restorations" and was written by Dr. Dennis Fasbinder.
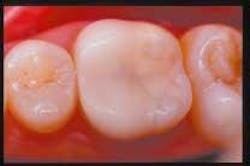
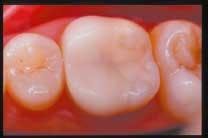
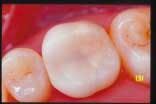
On page nine, the article offered readers a view of a Vita Mark II onlay at the one-year, two-year, and three-year recall appointments.
Unfortunately, in the printed supplement, the photograph of the one-year recall appeared for all three years. Below, the three photos appear in the correct sequence.
For readers who missed receiving the supplement with their September issues, copies are still available by calling (732) 935-2988.