HOW TO PROFIT FROM... implants
Working with insurers for reimbursement
Rose Nierman, RDH
Many people are demanding better dental care, saying in effect, "Save my teeth! My grandparents took their teeth out and I don`t want mine to be removable." Implants are a high-quality, viable choice to restore patients closer to natural chewing function. The investment for implants can range from a few thousand to $25,000 or more. How can we help patients receive these very special treatments when dental insurance is not likely to reimburse for implants or covers only a fraction of the cost? One option is to consider medical insurance as a reimbursement option.
Medical necessity
Many procedures performed in the dental office, including implants, may qualify for medical insurance. Medical insurers may reimburse for implants if oral disease complicates or causes other medical problems. For example, severe atrophy of bone affecting mastication with resultant digestive or nutritional problems, neoplasms and oral defects may all be considered as a medical necessity.
Dentists have a right to file on a patient`s insurance. Every state has an insurance statute specifying that medical insurers cannot deny a claim based solely on a practitioner`s degree if the treatment is medically necessary. The term "physician" refers to an appropriate provider when the treatment is within the scope of the provider`s license.
Dentists and certain other health-care providers who are not licensed as MDs can file for medical services. This is not to say that routine dental procedures should be filed through medical insurance. The National Association of Insurance Commissioners established a 1994 directive stating, "If an individual claimant has both a dental and medical plan, routine dental procedures must not trigger medical benefits first."
The ADA Council on Dental Care Programs does not define implants as routine dental care in their "Dental Benefit Plan Design Suggestions." Since implants are not routine dental care, file implant claims with medical first, if the prevailing diagnosis is medical in nature. We`re seeing many states passing laws that do not allow jawbone and/or jaw joint treatment to be excluded if bones and joints in other parts of the body are covered.
Although medical insurance is an option for implant surgery, the restorative phase is most often submitted to the dental carrier. More on this later.
Codes, forms and documents that conform to the medical arena are central to successful reimbursement. CPT (current procedural terminology) lists procedure codes that are used in conjunction with ICD medical-diagnosis codes such as Code 525.2, atrophy of jaw; Code 528.0, recurrent and multiple stomatitis; and Code V41.5, masticatory dysfunction. Use a standard medical-claim form (HCFA 1500) for medical-claims submissions. They are available through the American Medical Association.
Diagnostic acumen and precise documentation skills are key components to risk management and establishing medical need. A sound diagnosis by the dental physician will determine dental or medical necessity.
Poorly fitting dentures and alveolar atrophy can lead to nerve pain when chewing, difficulty masticating and subsequent digestive and nutritional problems. Congenital disorders, metabolic diseases, tumor surgery, traumatic injuries and facial-muscle atrophy are diagnoses frequently considered for reimbursement through medical insurers. Medical carriers may not consider a single-tooth replacement as a valid medical necessity. However, the medical insurers frequently consider implants for larger areas of restoration.
In the September 1997 issue of Dental Economics, insurance columnist Carol Tekavec, RDH, points out that the American Academy of Periodontology recommends that claims to medical plans only be considered when the patient has a condition caused or complicated by a medical problem or accident. The American Academy of Oral and Maxillofacial Surgeons cites difficulty in speaking, swallowing, pains and masticatory with associated digestive disorders as valid problems following alveolar resorption when the residual bone becomes inadequate to support a functional prosthesis.
A thorough medical history-taking is essential to diagnosis, treatment-planning and reimbursement success. Proper recordkeeping starts with the patient`s chief complaint(s) in the patient`s handwriting. An updated medical history form might include, "Has your oral condition affected your general health in any way?"
Consider a special section for patients with missing teeth or for those who wear partials or dentures. Ask about chronic mouth sores, facial pain, tissue or jawbone pain upon pressure, etc. Many patients have oral conditions that affect their general health and do not think to mention these problems to the dentist. Remember to remind your patients that the oral cavity is the first stage of digestion. By taking a more comprehensive medical history, we participate more fully in the patient`s overall heath in relationship to oral disease.
Once a diagnosis is established, a review of the insurance contracts will reveal if oral implants are a benefit or specifically excluded. Specific exclusions for oral implants can be determined by calling the carrier, sending a written preauthorization or reviewing the patient`s benefits booklet.
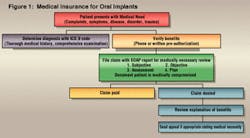
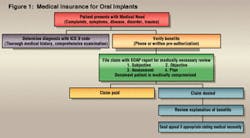
Because implant procedures are subject to review for medical necessity, all implant claims (or preauthorizations) should be accompanied by a narrative report. Reports should answer the question, "Why is this treatment needed?" The standard for narrative reports is the SOAP format as it provides necessity for treatment information very well:
S = Subjective Complaints
O = Objective findings
A = Assessment
P = Plan
Subjective data includes the patient`s subjective story including symptoms, chief complaints and past and current medical history.
Objective findings are the observations and findings revealed during clinical examination and from diagnostic tests such as X-rays, laboratory tests and physical findings.
Assessment refers to the working or final diagnosis, prognosis, restrictions, causation and other factors influencing the status of the patient. It also includes the severity of the patient`s problem(s).
Plan for each problem. Pro-cedures for initial treatment should be explicitly defined including plans for collecting information for further diagnosis. Include referrals to other providers.
A note about Medicare
Medicare (coverage for patients over 65 years of age) generally only provides reimbursement for implants if the patient is severely traumatized or compromised. Examples of instances in which Medicare may pay include reconstruction due to cancer or radiation therapy.
Private and group carriers and even medical HMOs and PPOs may provide reimbursement for implants. For PPOs, check to see what it takes for the patient to see a nonprovider. Many patients will gladly pay a higher copayment to see the dentist of his or her choice.
The dental claim
The implant restoration or prosthetic is more likely to be paid through dental than medical insurance. Special circumstances, including accidents, are submitted through the appropriate accident broker or medical carrier.
There are no special dental codes for implant prosthetics, so submit the usual dental code for the restorative procedure such as Code 02750, porcelain fused to high-noble metal crown; Code 06240, porcelain fused to high-noble metal pontic; or Code 05860, overdenture.
If the insurance contract does not allow for bridges and overdentures, ask for an alternative benefit for the amount the carrier normally would reimburse for a partial denture or whatever is allowed. Submitting an alternative-benefit claim may allow the patient to receive money the dental carrier would have applied to a partial to help with the implants. This is done with the insurer`s full knowledge that the patient is choosing the implants and not the partial denture.
JoAnn Majors, a practice-development consultant and dental manager stamps the claim as follows: "Our patient has requested consideration of an alternative benefit. The code for the alternative procedure for your insured is ..."
When requesting or filing an appeal for an alternative benefit, it is helpful to send a narrative stating the benefits of the higher-quality alternative to the patient. Your letter should illustrate the condition of the patient and complaints, failure of conventional methods, recommended treatment and the long-term prognosis without treatment. (See the sample letter included with this article.)
During review, the insurance consultant sets out to determine if the claim is medically/dentally necessary. According to the Health Care Financing Administration, "medical necessity" constitutes the following:
- The service provided is the most appropriate.
- The diagnosis is consistent with the symptoms.
- The treatment is consistent with the diagnosis.
- Treatment is not primarily for the convenience of the patient or provider.
- The treatment is good medical [dental] practice.
Claims that come back
We are all too familiar with claims that come back to your office for more information or with a rejection stamp. There are several reasons a claim will be sent back to your office:
4 Risk-management issue - Don`t unbundle implant claims. In other words, an implant submission does not require two separate codes. Use of a surgical code to prepare for the implant and an implant code is "unbundling" or "fragmenting." However, if you are performing another surgical procedure such as a full graft during the same operative session, special modifier codes are used to report a second procedure performed during the same operative session.
4 The patient was not precertified - Some insurance contracts insist on a phone or written precertification. On occasion, claims are not paid or are paid at only 50 percent (what would normally have been 80 percent) because precertification was not obtained. Carefully check the patient`s insurance card for precertification requirements.
4 Denials - Take immediate action on a claim that is returned to your office for any reason other than the contract exclusions. Persistence pays off. A government study of the insurance industry found that fully two-thirds of claims that are denied are reversed with one appeal letter.
Recordkeeping
Keep records consistent and accurate for medical and dental implants claims by incorporating the following:
o All patient visits should include the date, chief complaint, clinical findings, diagnosis or impression, tests and medications ordered, procedures performed, instructions given to the patient and the provider name. Entries should clearly document the need for the services.
o X-rays and other diagnostic tests should be thoroughly recorded. Copies of radiographs usually are not required for medical insurance, but recommended for dental.
o Consistently document consultations with other health providers and advice given to patients by telephone. In dental recordkeeping, if it isn`t written down, it doesn`t exist.
The key ingredients to successful implant reimbursement are:
* Training the dental team in complex dental claims and the use of medical insurance in dentistry.
* Presenting a diagnosis that represents a true need.
* Having an insurance contract which does not specifically exclude medically-necessary implants.
* Providing adequate documentation of need and sending appeals
Involve the patient as an active participant in seeking entitled benefits from insurance. The validity of a claim will depend on the extent that a patient is medically compromised and the specific benefits offered by a policy. Your skills in coding and documentation will result in appreciative and satisfied patients, as well as an increased percentage of paid claims.
Cross-coding for implants
Procedure / Dental Code / Medical Codes
--------------------------------------------------------------------
Endosteal Implants / 06010 / 21248 (3 or less) 21249 (4 or more)
Subperiosteal Implants / 06040 / 21245 (1/2 arch) 21246 (complete)
Implant Removal / 06100 / 20670 (superficial) 20670 (deep)
Implant Maintenance (in addition to prophylaxis code) / 06080 / No medical code applies. It is suggested Code 99213, Eval. & Mgmt. be used under special circumstances only.
Implant abutment (another dentist only) * / 06020 / No medical code applies.
The above procedure codes should be associated with ICD diagnostic code(s).
* The table shows an implant-abutment code for dental insurance used only if another dentist places the abutment. The implant surgery and abutment are reported with one code if the same dental provider places both.
Sample letter for alternative benefit
The above-named patient has missing teeth #s (list). Masticatory dysfunction has led to impaired first-stage digestion with frequent dental- and medical-office visits to alleviate soft-tissue and facial pain. Mrs. Patient has had four partial dentures, which she cannot wear due to diminished alveolar bone loss. There is concern about Mrs. Patient not being able to wear her partial, including extrusion of the opposing teeth making these teeth susceptible to fracture as well as potential damage to the jaw joints. We are recommending dental implants in conjunction with fixed partial dentures (implant-supported bridges).
If Mrs. Patient`s policy does not contain benefits for dental implants and an implant-supported fixed prosthetic, please consider an alternative benefit. The estimated fee for a partial denture is $1,285. Mrs. Patient has requested application of a $1,250 credit toward the implant/fix prosthetic.
We are looking forward to your prompt response. If you have any questions, please contact our office.