Economic management of the ill-fitting denture: The hard-soft double reline
Ian Shuman, DDS, MAGD, AFAAID
There are many reasons for relining a denture. A common need is often due to “gradual physiologic changes of the soft tissues, as well as resorption of the underlying osseous structure (that) can cause the denture to lose its original stability and retention.”1 In the past, laboratory-processed denture liners exhibited superior polymerization due to processing pressures and temperatures. However, current chairside reline materials have demonstrated properties that rival lab-processed relines.
Denture relining is a service that can be a profit center for the dental practice. But with allowable insurance fees, materials, and lab costs, denture relines can also be a loss, with practices actually subsidizing this service for their patients. To sustain profitability and provide patients with an excellent denture reline, the chairside reline is essential.
In the past, this procedure was met with derision. The available materials were inadequate, and the amount of time required to perform a chairside reline was excessive. Consequently, the preferred protocol for many practices was laboratory fabrication and processing for relines. This additional step was a drawback for patients who had to wait for lab processing of the relined denture and be without their dentures for several days or longer. In addition to lab fees, adjunct supplies needed for the procedure, such as impression material and bite registration, simply added to the expense.
Accuracy
Perhaps one of the most accurate techniques for denture relining is done chairside. The selection of materials is critical and cannot be emphasized enough. There are a variety of materials that are ideal for the short-term, such as tissue conditioners that include methyl methacrylate and others for long-term care; i.e., acrylic and silicone that include methyl methacrylate, ethyl methacrylate and silicone, among others.
Cost control
Providing the chairside denture reline can be a huge savings for clinicians (table 1), often reducing overhead costs by up to 90%. The only requirement is time and skill; increasing the skill decreases time, and a proficient clinician can effectively complete a denture reline rapidly and easily, provided the proper material is selected.
Product waste is a very real problem for dentists. Running a practice is akin to managing a mini-hospital. Practice overhead must be managed and material waste significantly reduced or eliminated. A dental budget should ideally include dental supplies at 5%.2 This figure can remain stable provided that the inventory is under control. One way to manage this is by limiting the inventory needed per procedure, including direct denture reline materials. By reducing product waste, overhead is also reduced. In addition, with the correct reline system, fewer alternative materials are required.
Table 1: Economic benefits of ideal hard-soft double reline
• Single appointment |
• Increase in referrals |
• Elimination of lab fee |
• Reduced product overhead |
• Minimal degradation |
• Less material waste with proper mixing tip |
To provide an example, the average cost for the denture reline, including adjunct materials, is between $200 and $300 per unit. In comparison, the maximum cost for a chairside hard denture reline should be $10 per unit, with a chairside soft denture reline $40 per unit.
Resiliency
Reline materials must be tear- and/or chip-resistant, designed to provide long-lasting relief, have outstanding durability, superb stain- and odor-resistance, and excellent adhesion to the denture. With a simple procedure, the entire denture-relining process can be completed in only one appointment and offer several years of satisfaction with minimal degradation. Savings are gained when less material is used, and even mixing tip size can have a direct effect on material use and waste. Materials should also resist contamination and odor buildup with long-lasting surface smoothness that prevents bacteria buildup. The proper reline material means less tearing and peeling due to strong adhesion.
Clinical benefits
Selecting the correct denture reline materials offers many clinical benefits (table 2). Clinically speaking, denture reline materials must be easy to handle and contamination-resistant, thus eliminating odor buildup. The materials should match the denture base color and offer long-term wear resistance. This is especially true with soft reline materials where it is important for the surface to retain long-lasting smoothness and avoid bacterial buildup. Adhesion of the liner to the acrylic denture base must be strong and tear/peel-resistant. In the end, a well-fitting denture will provide an improved masticatory efficiency and mucosal health, and relief from sharp ridges, tori pain, and sore spots.
Table 2: Clinical benefits of ideal hard-soft double reline
• Contamination-resistant |
• Elimination of odor buildup |
• Exceptional esthetics |
• Long-term wear resistance |
• Easy handling |
• Long-lasting surface smoothness |
• Exceptional polishability |
• Strong adhesion |
• Tear-resistant |
• No peeling |
• Improved masticatory efficiency |
• Improved mucosal health |
• Relief for sharp ridges and tori |
• Relief from pain, discomfort, and sore spots |
• Superior to tissue conditioners, which harden, discolor, |
Case report
A patient presented with an unstable, ill-fitting complete lower denture due to alveolar atrophy, and requested a soft liner for the lower denture. The goal was increased comfort and chewing ability, as well as improved fit to the lower jaw. Following a comprehensive examination, the tissue-bearing surface of the mandible was found to be tender to palpation in various areas.
It was decided that the best course of action would be to stabilize the denture base with a hard reline, followed by a selectively placed soft liner. Fresh resin was exposed by abrading the intaglio surface of the denture using a lab bur. Following this, the prosthesis was rinsed, dried, and a reline adhesive (Tokuso Rebase II Adhesive, Tokuyama Dental) was applied in two coats to all areas of the denture to be relined. Once dry, a separating medium, such as petroleum jelly, was applied to all areas where reline adhesion was not desired. Once completed, the hard denture reline powder and liquid were mixed (Tokuyama Rebase II, Tokuyama Dental) and dispensed onto the denture intaglio.
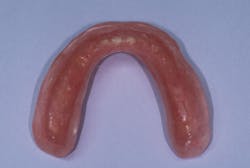
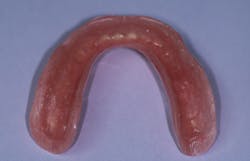
The denture was then inserted against the lower arch, and the patient was instructed to gently bite until the correct vertical dimension of occlusion was reached. As the resin began to harden, border molding was accomplished. Once initially set, the denture was removed from the patient’s mouth and excess material was trimmed. The denture was then inserted into the patient’s mouth until final hardening was complete. Once cured, remaining flash was removed and the flanges contoured and polished (figure 1). This first step in the procedure is complete following the evaluation of fit and stability, esthetics, phonetics, and occlusion.
Figure 1: Flanges contoured and polished
In order to gain additional adhesion and comfort, a soft reline was used. One of the most common types of failure with soft relines is the adhesion between the silicone reline and the denture acrylic. In a study published by the Journal of Applied Oral Science, it was determined that the use of a specialized primer (Sofreliner Tough Primer, Tokuyama Dental) increased the bond strength between the acrylic resin denture base and the silicone reline material.3 Another area of concern is the tear strength of silicone liners. Santawisuk et al. studied the dynamic viscoelastic properties of experimental silicone soft-lining materials.4
Results showed that the silicone elastomers demonstrated acceptable dynamic viscoelastic properties to be used as denture soft-lining materials. The resiliency of soft reline materials is also of concern, especially since patients tend to use denture cleansers on a daily basis. However, this had no effect on the hardness of the resilient denture liners evaluated after two years of in vivo simulated conditions of hygiene. Sofreliner Tough was the smoothest material before and after all treatments.
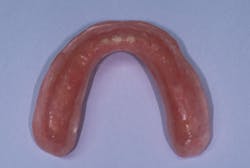
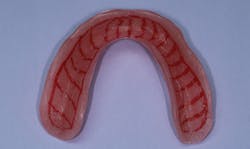
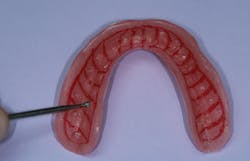
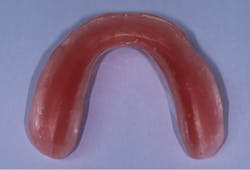
Approximately 2 mm of acrylic was removed from the tissue-bearing surface of the lower denture along the occlusal aspect of the alveolar ridge (figures 2 and 3). This provides the soft reline with sufficient thickness to prevent tearing and peeling, and allows enhanced comfort against the edentulous ridge. The prosthesis was rinsed, dried, and a soft reline primer (adhesive) (Sofreliner Tough Primer) was applied in multiple coats to the newly exposed acrylic. (Sofreliner Tough M, Tokuyama Dental) (figure 4). Once dry, the Sofreliner was injected onto all adhesive surfaces, and the denture was inserted against the lower arch. The patient was instructed to bite until the material was set (figure 5), followed by occlusal adjustment and denture delivery.
Figure 2: Lower denture
Figure 3: Acrylic reduced by 2 mm
Figure 4: Soft reline primer applied
Figure 5: Patient bit until material set
References
1. Leinfelder KF, Terry DA, Connelly ME. The art of denture relining. Inside Dentistry. 2007;3(5).
2. Blatchford B. Percentage of overhead is a choice. Dental Economics website. http://www.dentaleconomics.com/articles/print/volume-99/issue-1/departments/flourishing-in-changing-times/percentage-of-overhead-is-a-choice.html. Published January 2009. Accessed August 25, 2017.
3. Haddad MF, Goiato MC, dos Santos DM, Crepaldi NdM, Pesqueira AA, Bannwart LC. Bond strength between acrylic resin and maxillofacial silicone. J Appl Oral Sci. 2012;20(6):649-654.
4. Santawisuk W, Kanchanavasita W, Sirisinha C, Harnirattisai C. Dynamic viscoelastic properties of experimental silicone soft lining materials. Dent Mater J. 2010;29(4);454-460.
Ian Shuman, DDS, MAGD, AFAAID, maintains a full-time general, reconstructive, and esthetic dental practice in Pasadena, Maryland. Since 1995 Dr. Shuman has lectured and published on advanced, minimally invasive techniques. He has taught these procedures to thousands of dentists and developed many of the methods. Dr. Shuman has published numerous articles on topics including adhesive resin dentistry, minimally invasive restorative dentistry, cosmetic dentistry, and implant dentistry. He is a fellow of the Pierre Fauchard Academy.