Simplifying posterior composite placement using bulk-fill technologies
Robert A. Lowe, DDS, FAGD, FICD, FADI, FACD
Few materials in dentistry have undergone as much study and development as direct composite resins. Restorative dentistry changed forever when successful bonding to dentin was achieved. Since then, the challenge has been to find a simple, predictable approach to the clinical placement of composite restorations.
Unlike dental amalgam, which is a technique-insensitive material that can be successfully placed in a sea of moisture and intraoral contaminants (e.g., blood), the placement of composite resin requires strict isolation, more clinical steps, and exacting technique. The process of adhesion, conditioning of the tooth surface, and application of primers and adhesives, followed by the layering of composite resins to complete the restorative process involves many independent steps that must be properly executed to ensure good clinical results.
When it comes to Class II posterior composites, many of those restorations are placed on blind faith using techniques and armamentaria designed for amalgam placement, not composite placement. There is no way to evaluate the quality of layering in a proximal preparation that is between the buccal and lingual (palatal) line angles and not visible clinically. Amalgam is a truly condensable material; composite is not. Using round amalgam pluggers to place composite in geometrically shaped proximal boxes with line angles and point angles makes it difficult to ensure that these areas of the cavity preparation will be properly filled without voids. Usually these potential voids are not clinically or radiographically detectable, but can lead to early clinical failure due to bacterial contamination and microleakage.
The search for bulk-fill technologies that could reduce or eliminate the standard layering required to place composite restorations, while better adapting to the geometry of a cavity preparation, has been “on the radar” for quite some time.
Incremental versus bulk-fill placement of composite resin
Clinical placement of composite resins is traditionally taught using an incremental placement technique. To offset the effect of polymerization shrinkage, as well as the inability to light cure composite materials beyond a certain depth, it has been recommended to place composite resin in increments of 2 mm or less, and to cure each increment prior to placing the next. Also, it has been recommended to place each increment diagonally, engaging only one vertical wall of the preparation at a time, to avoid pulling the cusps together during light curing.
The question is: With advances in polymer chemistry, photo activation, and curing-light technologies that we currently see with modern composite resin materials, are these old rules still true? Many studies, some published as early as 2001, have compared incremental versus bulk-fill placement of composite resins and show that there is no difference in cuspal deflection (pulling of cusps) or a decrease in marginal integrity (white lines) when comparing the two techniques of placement. The main clinical issue with bulk fill of composite resins is depth of cure. It is also important to mention, based on the studies, that directional curing from the buccal and lingual (palatal) aspects at the gingival embrasures after removal of the matrix increases the ability to cure composite at the gingival margin of the proximal box in a Class II restoration.1-4
A review of bulk-fill composite technologies
As mentioned, the placement of posterior composite restorations can be a demanding clinical procedure. In many instances, restoring a tooth with a posterior composite restoration may require more time than a dental amalgam due to the number of steps involved in placement. Therefore, the introduction of any dental material that can reduce the amount of time required to place a posterior composite restoration without a sacrifice in quality should be of great interest to the profession.
Bulk-fill flowable composite resins have been in use for several years and are traditionally designed to be used as a dentin replacement (up to 4 mm) for use in posterior composite resin restorations. Such use has been claimed to increase marginal adaptation in the gingival marginal area of Class II composite restorations, thereby reducing microleakage.5 These materials all require a placement of a nanohybrid composite as a capping layer (1 mm–1.5 mm thick) to give the restoration the physical properties needed to withstand posterior occlusal forces. It has also been claimed to help counter the polymerization shrinkage stress of overlying composite resins due to the more elastic nature of flowable composites.6 While neither of these perceived advantages have been validated, there is relatively broad consensus that the use of flowable composites does help achieve optimal adaptation of overlying composite to the intricacies of cavity preparations.
Bulk-fill packable composites are traditional materials that have been altered to achieve a greater depth of cure, thereby allowing placement in fewer increments. In the author’s opinion, these materials have the same challenges in placement as traditional composites and benefit from the use of a flowable composite as a liner to better adapt to the internal surface of the cavity preparation. Other than reducing the number of increments required, bulk-fill packables don’t really address the other clinical challenges of placing posterior composite restorations, such as condensing and adaptation to the cavity preparation. One exception is SonicFill (Kavo Kerr), which is a proprietary material that requires a specially designed handpiece to create sonic energy that lowers the viscosity of the composite at placement. SonicFill thereby adapts well to the geometry of a cavity preparation without the use of a flowable composite used as a liner.
The evolution of bulk-fill flowable resins
With the introduction of a new class of bulk-fill flowable composites, Estelite Bulk Fill Flow (Tokuyama Dental) is changing the way bulk-fill flowable composites are placed by eliminating the need for a traditional nanohybrid capping layer. According to the manufacturer, the spherical nature of the fillers used allows for an increase in physical properties and esthetics (particularly opacity), the main reason traditional flowable composites have been indicated for dentin replacement only. Estelite Bulk Fill Flow is more translucent at placement to allow for depth of cure up to 4 mm. During polymerization, the material becomes more opaque to better match the optical properties of the surrounding tooth structure (i.e., enamel). Another feature of the spherical fillers, whose average size is 200 nanometers (supra-nano) is the creation of an extremely smooth surface that polishes quickly and has very high luster.
Clinical case report: Class II posterior bulk-fill flowable composite
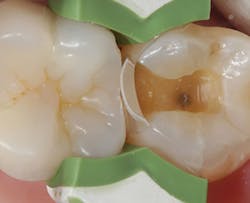
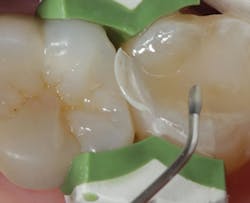
The Class II mesio-occlusal composite shown in tooth No. 2 has recurrent decay on the proximal surface, with an open margin at the junction of the occlusal and facial portions of the preparation, presumably due to a material fracture (figure 1). The old composite material and existing recurrent decay is removed and a sectional matrix (Biofit, Bioclear) and sectional ring (Composi-Tight 3D Fusion Wide Prep, Garrison Dental Products) are placed, and the quadrant is isolated with Isolite (Isolite Systems) and a DryTip saliva absorbent (Microbrush International) covering Stensen’s (parotid) duct.
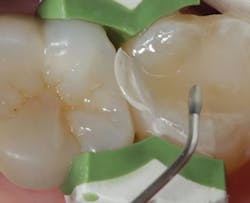
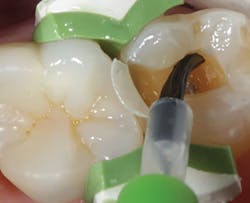
The existing restoration and recurrent decay are removed and a sectional matrix is placed on the mesial aspect of the tooth (figure 2). The preparation is selectively etched on the enamel periphery using 37% phosphoric acid for 15 seconds and then rinsed with water. The enamel is dried with air, then the bonding agent (Bond Force, Tokuyama Dental) is placed on both enamel and dentin with a microbrush (figure 3). After light curing the bonding agent for 20 seconds, the selected shade (A2) of bulk-fill flowable composite (Estelite Bulk Fill Flow, Tokumaya Dental) is placed into the cavity preparation (figure 4).
Figure 1: View of the compromised composite restoration
It is important to emphasize the importance of a properly fitted anatomic sectional matrix to limit any potential excess material as it is placed into the preparation. The goal should be to have as little rotary finishing and contouring as possible.
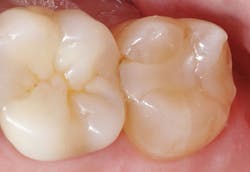
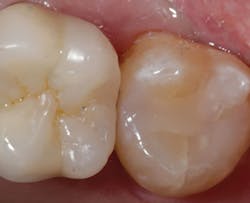
After light curing the composite per manufacturer’s instructions, the matrix and isolation are removed. The occlusal contacts are checked with articulating paper and adjusted as needed. Lastly, the restoration is polished using rubber composite polishing instruments (A.S.A.P. All Surface Access Polishers, Clinician’s Choice). Figure 5 shows a postoperative view of the completed restoration. Note the extremely high luster achieved and how nicely the restorative material blends into the tooth structure.
Figure 2: Tooth after removal of composite and placement of matrix
Figure 3: Placement of bonding agent with a microbrush
Figure 4: Placement of bulk-fill flowable composite
Figure 5: Postoperative view of completed restoration
Conclusion
Clinicians have long desired for composite restorative materials to have a more simplified, less technique-encumbered approach to placement. A bulk-fill flowable composite offers the benefit of precise adaptation to the cavity preparation, while at the same time eliminating incremental placement and condensation (plugging). Estelite Bulk Fill Flow goes one step further by eliminating the capping layer so that cavity preparations of 4 mm or less in depth can be filled entirely in one increment. That, combined with the high polishability due to the spherical filler, offers the clinician a high-quality restorative option for a variety of clinical applications.
References
1. Campodonico CE, Tantbirojn D, Olin PS, Versluis A. Cuspal deflection and depth of cure in resin-based composite restorations filled by using bulk, incremental and transtooth-illumination techniques. J Am Dent Assoc. 2011;142(10):1176-1182.
2. Rees JS, Jagger DC, Williams DR, Brown G, Duguid W. A reappraisal of the incremental packing technique for light cured composite resins. J Oral Rehabil. 2004;31(1):81-84.
3. Flury S, Hayoz S, Peutzfeldt A, Hüsler J, Lussi A. Depth of cure of resin composites: is the ISO 4049 method suitable for bulk fill materials? Dent Mater. 2012;28(5):521-8. doi: 10.1016/j.dental.2012.02.002.
4. El-Safty S, Silikas N, Akhtar R, Watts DC. Nanoindentation creep versus bulk compressive creep of dental resin-composites. Dent Mater. 2012;28(11):1171-1182. doi: 10.1016/j.dental.2012.08.012.
5. Ilie N, Bucuta S, Draenert M. Bulk-fill resin-based composites: an in vitro assessment of their mechanical performance. Oper Dent. 2013;38(6):618-625. doi: 10.2341/12-395-L.
6. Roggendorf MJ, Krämer N, Appelt A, Naumann M, Frankenberger R. Marginal quality of flowable 4-mm base vs. conventionally layered resin composite. J Dent. 2011;39(10):643-647.
Robert A. Lowe, DDS, FAGD, FICD, FADI, FACD, graduated magna cum laude from Loyola University School of Dentistry in 1982, where he was a clinical professor in restorative dentistry until 1993. He maintains a private practice in Charlotte, North Carolina, lectures internationally, and publishes on esthetic and restorative dentistry. In 2004, he received the Gordon Christensen Outstanding Lecturers Award, and in 2005, diplomat status on the American Board of Esthetic Dentistry. Dr. Lowe can be reached at [email protected].