Polyphosphazene-based resilient denture liners: A definitive solution for edentulous patients
Joseph Massad, DDS
Russel A. Wicks, DDS, MS
Swati Ahuja, MDS, BDS
It is both emotionally and financially rewarding to treat edentulous patients. However, their treatment may be challenging due to loss of osseous structures, knife-edge ridges, sensitive mucosa, deep undercuts, bony exostoses and protuberances, constant soreness, and deteriorating health. All these conditions, in addition to the hardness and rigidity of denture base resins, make it difficult for patients to continue wearing their existing dentures.1-5 A number of resilient lining materials have been developed and used on the intaglio surface of acrylic denture bases to overcome these problems.6
Resilient liners provide shock absorption, improve the retention of the prosthesis, and decrease the masticatory loads on denture-bearing surfaces of the maxilla and mandible.7,8 Additional benefits include improvement of masticatory efficiency,9 chewing strokes, and chewing time; and maximization of the occlusal force.10,11 They also aid in improvement of speech, stability of the prostheses, reduction of pain, and increase psychological comfort and longer denture-wearing times.12–14 Based on their chemical composition, conventional resilient lining materials can be classified as either acrylic based or silicone based.5 However, both these materials are best considered as temporary expedients since they must be replaced every six to nine months. Acrylic-based liners lose their viscoelastic properties due to leaching of plasticizers, and silicone-based liners fail due to fungal contamination.15 Frequent replacement of resilient liners is time consuming and places a chronic financial burden on patients.
The research to develop a resilient liner that has improved strength, permanent resiliency, improved adhesion to denture bases, the ability to inhibit growth of microorganisms, biocompatibility, and chemical stability has been ongoing. Existing lining materials have been periodically treated with antimicrobial agents and surface coatings to prevent fungal contamination16 and to restrict the migration of toxic plasticizers, respectively.15 But all these procedures still have not resulted in the production of a liner that will last for as long as the life of a denture.
A polyphosphazene-based material (Novus, White Square Chemical) that was used from the late 1980s until 1995 was reintroduced in 2011. This material is FDA approved, has a five-year warranty, shore hardness of 45 units, and unlimited shelf life if kept frozen.17 Clinical studies have proven that this material resists the growth of Candida albicans in almost all patients, thus requiring no periodic antimicrobial treatments, unlike the silicone materials that frequently become contaminated with subsurface and surface fungus after only a few months of use.18,19 Patient satisfaction has also been reported as high with this material.20 It is composed of polymer chains of rubber (70% by weight) that are mixed with several polymer chains of acrylics to improve its hardness, tensile strength, bond strength, and water sorption properties.21 Due to the absence of plasticizers, it does not require periodic surface coating, remaining soft with excellent durability. The polymer chains of acrylics permit the achievement of a chemical bond to the denture base, holding the material very tightly together and keeping it intact.22
The advantages of using this material include color stability; radiopacity (it can be identified if any parts or pieces are accidentally ingested or inhaled by the patient); excellent shock absorption, with no rebound; durability due to lack of plasticizers; and decreased porosity.6,17,22 This material meets the American Dental Association requirements of solubility,23 is temperature insensitive,24 demonstrates excellent clinical performance despite increased water sorption,25 and is readily wettable. Use of the polyphosphazene-based liner aids in conservation of the osseous structures, as it engages bony undercuts, and precludes the need of surgical removal. It is introduced in the denture through a technique similar to that used for introducing heat-polymerized silicone liners (standard compression molding laboratory processes); hence, conventional laboratory equipment and materials can be used.17,22 Additionally, it is easy to adjust, finish, and polish with conventional rotary intrumentation.17,22 There is no waste when using this material; any excess that oozes out during packing can be recovered and used in areas where there isn’t any excess or saved for the next denture. It is available as a single component paste, so no mixing is required during its usage.
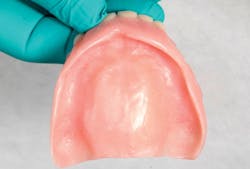
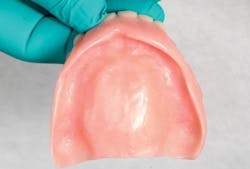
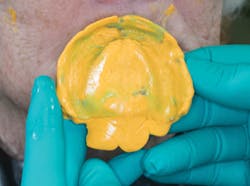
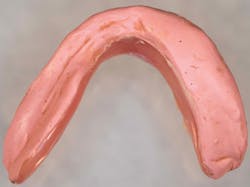
The clinical steps for introducing the liner include appropriately relieving the denture to provide adequate bulk for the impression material (figure 1) and then making a definitive impression using varying viscosities of vinyl polysiloxane impression (VPS; Aquasil, Dentsply Caulk) material, with the denture as the impression tray (figure 2).It is important to maintain the occlusal vertical dimension during the making of the definitive impression. The impressed denture along with detailed instructions are sent to the dental laboratory for indirectly introducing the liner in the prosthesis (figure 3). The liner can be adjusted with conventional rotary instruments.17,22
Figure 1: Denture relieved to provide adequate bulk of impression material
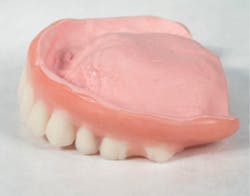
Figure 3: Polyphosphazene-based liner introduced in the denture
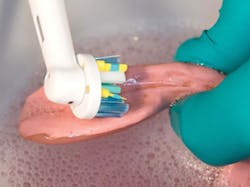
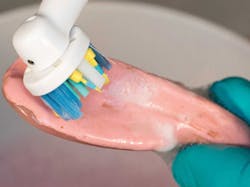
The polyphosphazene-based liner is easy to maintain and clean. One of our patients recently visited our clinic for a recall visit.6 The patient had a polyphosphazene-lined denture that was at least four to five years old and had a few stains. The patient told us that she was very comfortable with the liner and requested that it only be cleaned of the stains if possible, not replaced. On inspection of the oral cavity, the denture-bearing mucosa and the adjacent soft tissues appeared healthy. The denture and the liner were cleaned with an ultrasonic toothbrush and soapy water and delivered to the patient (figure 4).
Figure 4: Four- to five-year-old polyphosphazene-based liner cleaned with an ultrasonic toothbrush (Oral-B Genius) and soapy water
Conventional liners fail after a maximum of 12 months of use, leading to mucosal inflammation and soreness.21 However, we have followed up several patients with polyphosphazene-lined dentures and they are all very comfortable with their prostheses, even after several years of use.
References
1. Bulad K, Taylor RL, Verran J, McCord JF. Colonization and penetration of denture soft lining materials by Candida albicans. Dent Mater. 2004;20(2):167-175.
2. Mack PJ. Denture soft linings: Clinical indications. Aust Dent J. 1989;34(5):454-458.
3. El-Hadary A, Drummond JL. Comparative study of water sorption, solubility, and tensile bond strength of two soft lining materials. J Prosthet Dent. 2000;83(3):356-361.
4. Saber-Sheikh K, Clarke RL, Braden M. Viscoelastic properties of some soft lining materials. II—ageing characteristics. Biomaterials. 1999;20(21):2055-2062.
5. Chladek G, Żmudzki J, Kasperski J. Long-term soft denture lining materials. Materials (Basel). 2014;7(8):5816-5842.
6. Gettleman L. Novus Denture Liner: An innovative use of polyphosphazene in dentistry. Inside Dental Technology website. https://www.aegisdentalnetwork.com/idt/2011/04/novus-denture-liner-lang-dental. Published April 2011. Accessed February 19, 2018.
7. Parker HM. Impact reduction in complete and partial dentures, a pilot study. J Prosthet Dent. 1996;16(2):227-245.
8. Braden M, Wright PS, Parker S. Soft lining materials—a review. Eur J Prosthodont Restor Dent. 1995;3(4):163-174.
9. Takahashi Y. The effects of soft denture liners applied to complete dentures on masticatory functions. Kokubyo Gakkai Zasshi. 1997;64(4):518-533.
10. Murata H, Taguchi N, Hamada T, Kawamura M, McCabe JF. Dynamic viscoelasticity of soft liners and masticatory function. J Dent Res. 2002;81(2):123–128.
11. Hayakawa I, Hirano S, Takahashi Y, Keh ES. Changes in the masticatory function of complete denture wearers after relining the mandibular denture with a soft denture liner. Int J Prosthodont. 2000;13(3):227-231.
12. Kimoto S, Kimoto K, Gunji A, et al. Clinical effects of acrylic resilient denture liners applied to mandibular complete dentures on the alveolar ridge. J Oral Rehabil. 2007;34(11):862-869.
13. Kimoto S, Kimoto K, Gunji A, et al. Effects of resilient denture liner in mandibular complete denture on the satisfaction ratings of patients at the first appointment following denture delivery. Nihon Hotetsu Shika Gakkai Zasshi. 2008;52(2):160-166.
14. Pisani MX, de Luna Malheiros-Segundo A, Balbino KL, de Freitas Souza R, de Freitas Oliveira Paranhos H, da Silva CHL. Oral health related quality of life of edentulous patients after denture relining with a silicone-based soft liner. Gerodontology. 2011;29:e474-e480.
15. Rodrigues S, Shenoy V, Shetty T. Resilient liners: A review. J Indian Prosthodont Soc. 2013;13(3):155-164.
16. Skupien JA, Valentini F, Boscato N, Pereira-Cenci T. Prevention and treatment of Candida colonization on denture liners: a systematic review. J Prosthet Dent. 2013;110(5):356-362.
17. Novus denture liner home page. http://novusliner.com. Accessed December 19, 2017.
18. Hazelrigg DE, Selvaraj R, Waters JC, Gettleman L. Polyphosphazene for maxillofacial prosthetics. J Dent Res. 1993;72(20):128.
19. Gettleman L, Fisher DL, Farris C. Self-sanitizing soft denture liners: Paradoxical results. J Biomed Mater Res. 1983;17(4):731-734.
20. Gettleman L, Guerra LR, Jameson LM. Clinical trial of Novus soft denture liner vs. Molloplast B: Final results and four year follow-up. J Dent Res. 1990;69:166.
21. Razavi R, Khan Z, Haeberle CB, Beam D. Clinical applications of a polyphosphazene-based resilient denture liner. J Pros. 1993;2(4):224-227.
22. Jesse J. Novus definitive resilient denture liner: Proprietary technology promotes healthy tissue and patient compliance. Inside Dentistry website. https://www.aegisdentalnetwork.com/id/2011/09/novus-definitive-resilient-denture-liner. Published September 2011. Accessed February 19, 2018.
23. Kawano F, Dootz ER, Koran A 3rd, Craig RG. Sorption and solubility of 12 soft denture liners. J Prosthet Dent. 1994;72(4):393-398.
24. Waters MG, Jagger RG, Polyzois GL. Wettability of silicone rubber maxillofacial prosthetic materials. J Prosthet Dent. 1999;81(4):439-443.
25. Sid K, Takamata T. Polymers in the Oral Environment: Novel Elastomers as Soft Liners. In: Wise DL, Trantolo DJ, Lewandrowski KU, Gresser JD, Cattaneo MV, eds. Biomaterials Engineering and Devices: Human Applications. Vol 2. Totowa, New Jersey: Humana Press; 2000:25-45.
Joseph Massad, DDS, is in private practice in Tulsa, Oklahoma. He is an honorary member of the American College of Prosthodontics. Currently, he holds faculty positions at Loma Linda University, is an associate professor in the Department of Prosthodontics at the University of Tennessee College of Dentistry, and is clinical assistant professor at the University of Oklahoma College of Dentistry. He is a recipient of Chicago Dental Society’s Gordon J. Christensen Recognition Lecturer Award.
Russell A. Wicks, DDS, MS, is professor and chairman at the Department of Prosthodontics at the University of Tennessee College of Dentistry. He has conducted prosthodontic research and directed the undergraduate curriculum in removable prosthodontics and dental implants. In 2000, Dr. Wicks was appointed to the Academy of Distinguished Teaching Professors. He has also received the Distinguished Dental Faculty Award from the College of Dentistry and has been elected to membership in the American College of Dentists.
Swati Ahuja, MDS, BDS, graduated with a bachelor of dental surgery from Nair Hospital Dental College in 2002, and master of dental surgery and certificate in prosthodontics from University of Tennessee in 2009, where she worked as an assistant professor for three years. She has lectured nationally and internationally and has multiple publications in peer-reviewed journals. She also the coauthor of Applications of the Neutral Zone in Prosthodontics. Currently, she has a private practice in Mumbai.