Bonding to lithium disilicate
John Nosti, DMD, FACE, FAGD, FICOI
Open any dental publication and you will be greeted with advertisements for the latest and greatest in all-ceramic dentistry. Manufacturers continue to unveil materials that claim superiority in wear compatibility, esthetics, strength, and ease of cementation. Still, the most frequent questions I hear from my colleagues are: Which material is best for my particular case? Which “cement” do I use? Are self-adhesive cements considered bonding?
When dealing with cases that combine esthetic and functional challenges, my material of choice for 12 years has been lithium disilicate (IPS e.max, Ivoclar Vivadent). Lithium disilicate remains one of the most versatile materials in all-ceramic dentistry and is perhaps the best-studied of any all-ceramic indirect restorative material. It offers a combination of durability and beauty, as well as the ability to bond at higher strengths.1–3 Additionally, it can be fabricated with a micro–cut back in anterior teeth.4 This allows for an esthetic result of a cut back and layered restoration, while the lingual of the restoration can be kept in its monolithic form. The result is the lingual/palatal side of the anterior restoration provides a flexural strength of 500 MPa. This design is helpful in restoring patients with signs of anterior attrition in which the doctor is seeking an esthetic result while still maintaining strength.
While translucent zirconia has been advertised heavily to doctors as an alternative to lithium disilicate in esthetic and strength properties, studies have shown that as zirconia becomes more translucent, its strength is decreased significantly.5–7 With translucent zirconia having a strength similar to IPS e.max and marginal esthetics, and with long-term bond tests lacking, it has not proven to be the material of choice to date. It is important to understand that in cut-back and layered form, all materials, regardless of the choice of core material (zirconia, metal, or ceramic), all have a flexural strength similar to one another at 150–185 MPa.8,9
The advantage of using lithium disilicate is that the material can be pressed to 0.5 mm thick (for veneers)and still have a flexural strength of 500 MPa. Plus there will be enhanced chemical bonding to the tooth. This is crucial in situations with limited mechanical retention, such as is the case with veneers. It allows the doctor to make minimal preparations, conserve more tooth structure, and still have an esthetic, strong result.10
Lithium disilicate must have an occlusal restorative thickness of 1.5 mm in order for self-adhesive or conventional cements to be used. Self-adhesive cements have the following advantages:
- Ease of use—A one-step delivery system eliminates the need for an etch-and-bond technique.
- Dual-cured—Excess cement can be briefly light-cured to aid in cleanup.
The disadvantages of self-adhesive cements include the following:
- Color instability—Many self-adhesive cements are not color stable. If a cement does not claim color stability, it might not be color stable with time.
- Lower bond strengths—There are significantly lower bond strengths to all types of tooth structure compared to those of adhesive cements with an etch-and-bond technique. Contrary to some beliefs, using a self-adhesive resin cement is not considered “bonding.”
- Contraindications—Self-adhesive cements are contraindicated where mechanical retention is compromised, such as with veneers.
- Limited working time—This is due to their dual-cure nature. In cases of multiple units, cementation technique and limited working time can increase the difficulty in seating restorations.
- Radiopacity—Not all self-adhesive cements are radiopaque. This can be an issue where cement is not fully removed interproximally during cleanup and goes undetected on radiographs.
There are also total-etch and self-etch adhesive resin cements available. As with bonding composite resins, a total-etch technique requires a separate step of applying phosphoric etch to tooth surfaces, either selectively etching the enamel only or etching enamel and dentin. A prime-and-bonding agent is then applied to the tooth. The self-etching technique incorporates etching, priming, and bonding of the tooth surfaces into a single agent. The benefits of using either of these over self-adhesive cements include:
- Increased bond strengths to the teeth and ceramic;
- Increased working time when placing multiple restorations;
- The ability to use try-in pastes that mimic the appearance of the cement; and
- Long-term color stability.
Case study
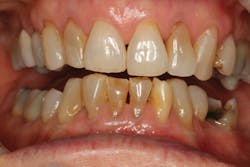
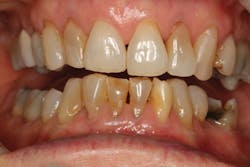
A 70-year-old patient presented with anterior and posterior wear from attrition. In addition, her posterior teeth had large direct restorations with fractures present (figure 1a–1c). The patient elected to undergo a staged reconstruction that restored her maxillary anterior 10 teeth, mandibular anterior six teeth, and the mandibular left premolar and molar due to fractures. (The patient had first premolars extracted due to orthodontic treatment.)
Figure 1a–1c: Patient presentation
For these restorations, I elected to use Variolink Esthetic (Ivoclar Vivadent), which can be used with a total-etch or self-etch technique. This material is available in both LC (light-cure) and DC (dual-cure) forms. First, I inserted the restorations with a try-in paste to ensure marginal fit, contacts, occlusion, contour, and esthetics. Each restoration was then removed and treated with Ivoclean (Ivoclar Vivadent). Lithium disilicate is best pretreated with hydrofluoric acid to increase retention rates, which is usually completed in the lab. Unfortunately, saliva contaminates this interface. Ivoclean was placed in each restoration for 20 seconds, and rinsed to remove any surface contaminants. Monobond Plus (Ivoclar Vivadent), a silane agent, was then placed in each restoration with application time of 60 seconds, followed by air drying. Monobond Plus is shelf-stable and can be used for multiple ceramic materials, as well as as a primer for metal and zirconia. Each restoration was then loaded with the corresponding shade of Variolink Esthetic LC cement that was chosen for the try-in paste and placed in a light box.
Monobond Plus is shelf-stable and can be used for multiple ceramic materials, including metal and zirconia as a primer.
The teeth were isolated with a rubber dam and cleaned with Tubulicid Red (Temrex). Phosphoric acid was placed and rinsed. Telio CS Desensitizer (Ivoclar Vivadent) was placed on each preparation and blotted dry to prevent desiccation of the dentin tubules. Adhese Universal bonding agent (Ivoclar Vivadent) was placed, scrubbed for 20 seconds per tooth, air dried, and cured for 10 seconds. The restorations were placed from the midline moving posteriorly bilaterally and cured using the “tack and wave” technique. A special tack tip (Sure Dental) was initially used on a Bluephase curing light (Ivoclar Vivadent) for one second per tooth, and then the standard light stylus was used during the wave technique (2–4 seconds for the entire arch). Excess cement was removed, Liquid Strip (Ivoclar Vivadent) was placed, and the final cure was completed for 30 seconds per surface. The molars in this case were placed using the same technique with Variolink Esthetic DC.
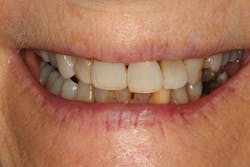
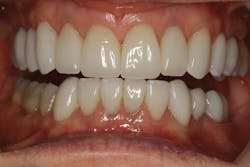
Lithium disilicate and proper bonding allowed me to provide conservative dentistry while achieving maximum strength and satisfying the patient’s esthetic requests (figure 2a–2c).
Figure 2a–2c: Final restorations
References
1. Guess PC, Zavanelli RA, Silva NR, Bonfante EA, Coelho PG, Thompson VP. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
2. Cortellini D, Canale A. Bonding lithium disilicate ceramic to feather-edge tooth preparations: a minimally invasive treatment concept. J Adhes Dent. 2012;14(1):7-10.
3. Tysowsky G. The science behind lithium disilicate: today’s surprisingly versatile, esthetic and durable metal-free alternative. Oral Health website. https://www.oralhealthgroup.com/features/the-science-behind-lithium-disilicate-today-s-surprisingly-versatile-esthetic-durable-metal-free-al/. Published March 1, 2009.
4. Culp L, McLaren EA. Lithium disilicate: The restorative material of multiple options. Compend Contin Ed Dent. 2010;31(9):716-720,722,724-725.
5. Bakitian F, Seweryniak P, Papia E, Larsson C, Vult Von Steyern P. Fracture resistance of translucent zirconium-dioxide crowns with different semi-monolithic designs. Dent Mater. 2017;33(1):e8-e9.
6. Carrabba M, Keeling AJ, Vichia A, Fonzara RF, Wood D, Ferraria M. Translucent zirconia in the ceramic scenario for monolithic restorations: A flexural strength and translucency comparison test. J Dent. 2017;60(5):70-76.
7. Flinn B, Raigrodski AJ, Mancl L, Toivola R, Kuykendall T. Influence of aging on flexural strength of translucent zirconia for monolithic restorations. J Prost Dent. 2017;117(2):303-309.
8. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Microtensile bond strength of different components of core veneered all-ceramic restorations. Part II: Zirconia veneering ceramics. Dent Mater. 2006;22(9):857-863.
9. Lin WS, Ercoli C, Feng C, Morton D. The effect of core material, veneering porcelain, and fabrication technique on the biaxial flexural strength and weibull analysis of selected dental ceramics. J Prost. 2012;21(5):353-362.
10. Xiaoping L. Effect of etching time and resin bond on the flexural strength of IPS e.max Press glass ceramic. Dent Mater. 2014;30(12):e330-e336.
John Nosti, DMD, FACE, FAGD, FICOI, practices full time in Mays Landing and Somers Point, New Jersey (drnosti.com). His practices are focused on functional cosmetic dentistry, full-mouth reconstruction, and temporomandibular joint dysfunction. He is the clinical director of the Clinical Mastery Series CE continuum (clinicalmastery.com).