Why do dental implants fail?
In this monthly feature,
Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Q: I started practicing dentistry about 30 years ago, as root-form dental implants began to be commonplace. At that time, there was skepticism about the new form of implants, because some previous forms had shown significant failure before the titanium root-form implants emerged. Slowly, the new titanium implants began to prove themselves. Most of us were using the original Brånemark design for edentulous patients, which called for six implants in each arch anterior to the mental foramen and anterior to the maxillary sinus.
Now, 30 years later, I see many implants of numerous brands failing, while the natural teeth serving around them are healthy and stable. How do you explain what is happening to the implant success rate? What is the cause of so many of these implant failures?
A: Thanks for briefly tracing the early history of titanium root-form implants. As a prosthodontist, I have been placing root-form implants since they were initially introduced, and I share your opinions about the growing concern related to implant failure.
A recent Swedish clinical study of 588 patients who had received implants nine years prior revealed some frustrating results.1 The large majority of the implants were Astra Tech, Nobel Biocare, Straumann, and a few miscellaneous brands. After nine years of implant service, 45% percent of the patients had peri-implantitis with bone loss greater than 0.5 mm accompanied by bleeding on probing/suppuration.1 Moderate to severe peri-implantitis and bone loss greater than 2 mm was present in 14.5% of the patients.1 Patients with periodontitis and with more than four implants exhibited higher odds for moderate to severe peri-implantitis.1
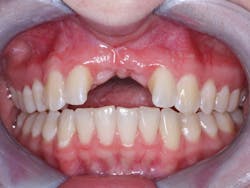
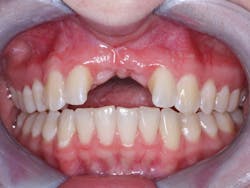
Figure 1: This image shows a 19-year-old patient who had a bone graft placed planning for subsequent implant placement. The expensive graft failed. The same surgical specialist suggested another bone graft. The family sought other treatment options.
This study shows results comparable to other previously published studies. It seems appropriate to reassess the status of implant success and reconsider the comparison of implant-supported treatment with conventional tooth-supported treatment.
Potential reasons for implant failure
Factors that may be contributing to implant failure need to be considered and remedies suggested for overcoming them. Following are some of the factors that contribute to dental implant failure.
Lack of education about implants in dental schools
Most graduates from US dental schools have had minimal education about dental implants, and few have had the opportunity to place implants themselves while in school. During the hundreds of continuing education courses I deliver annually, I often ask the audiences about their placement and restoration of implants. From their answers, it is obvious that most general practitioners are restoring implants, but only a small percentage of them are placing implants.
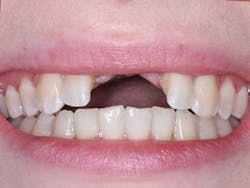
Figure 2: The patient’s highest natural smile shows no display of the bony void.
Having been a full-time dental faculty member in three schools, I fully understand the struggles for curriculum time. Yet, as a freelance educator, I am highly frustrated to see that most dentists who desire to place implants must seek education primarily through continuing education—some of which is excellent and some of which is not.
Since implants are growing in use and implant failure has now been shown in many studies, it is time for dental school educators to make time for at least introductory courses on dental implant placement and restoration.
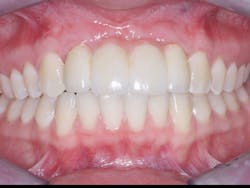
Figure 3: A four-unit fixed prosthesis was placed on long, stable lateral incisors. Gingiva-colored ceramic was fired onto the apical portions of the prosthesis. This treatment satisfied the patient’s esthetic and functional needs adequately.
Lack of integration and communication between specialists and General dentists
Currently, graduate programs in oral surgery, periodontics, prosthodontics, and endodontics include education and training on implant placement. With the exception of prosthodontics, which includes both placement and restoration of implants, some new specialists have only rudimentary predoctoral dental school education about diagnosis and treatment planning for restoring implants. Fortunately, most continuing education programs in implant dentistry are integrating both implant placement and restoration.
The two aspects of implant dentistry, surgery and prosthodontics, must be integrated in these specialty programs. Using a lay analogy, the construction person making a foundation for a house needs to know how the walls and roof relate to the foundation. Currently, I see some specialists who still need basic education in restorative dentistry and prosthodontics. Also, I suggest that all practitioners restoring but not placing implants should have combined educational experiences with the dentist placing the implants, and that they should have frequent treatment planning sessions together. An example is shown in Figures 1–4.
Figure 4: Patient’s highest unstrained smile satisfying the clinical need in three weeks with conventional dentistry. This example highlights the need for better surgical and prosthodontic consultation and more surgical specialist knowledge about prosthodontics. The previous graft, the graft failure, and the lack of patient and parent acceptance of another graft took years and cost a significant amount of money.
Loading too soon
Implants integrate with bone at different times depending on numerous factors, including bone density, occlusion, patient health, and other factors. Occasionally, I have been asked by patients to load their implants sooner than I feel comfortable because of upcoming family social events, esthetics, a geographic move, and other reasons. Unfortunately, some of these situations have led to implant failure, patient dissatisfaction, and significant loss of money. I prefer leaving any questionably stable implants for several months before loading.
The time for a typical titanium implant to integrate into bone varies, but most studies show a period of three to six months is adequate. It has been proven that stable implants can be successfully loaded before that time, but there is still controversy among clinicians on whether to wait for osseointegration or not. In my opinion, a longer wait time is better.
Placing implants too soon into sites where previous endodontically treated teeth have failed
A common practice has been to remove a failing endodontically treated tooth and place an implant on the same day. Some research questions this practice, stating that the organisms that caused the endodontic failure are still in the bone and could cause implant failure. Until further research is available on the subject, it appears that grafting the socket and waiting for bone maturity is a wise decision.
Overloading implants
The exact number of implants necessary for support of a specific prosthesis is a guess at best. Factors influencing this decision include bone density, implant diameter and length, as well as apparent intensity of occlusion. Overt bruxers can destroy any prosthesis as well as cause implant failure. I have seen many cases of apparently overloaded implants that are functioning well, as well as those that fail. A logical conclusion is that more implants are better than fewer. However, patient financial concerns often lead to clinical misjudgment and fewer implants.
Inadequate bone density
Placing implants in bone of questionable density, such as type IV or III bone, requires clinical experience and good judgment. Often, salvaging a stable tooth is a better, more predictable choice than removal of the tooth, grafting, and placing an implant.
When bone has questionable density and implant success may be compromised, patients should have complete informed consent about the clinical situation and the odds for success. Nonimplant-supported conventional treatment may be indicated instead of implants.
Summary
There are many reasons why implants fail, and many more are still to be determined. A few of the reasons were explained in this article, many of which can be avoided.
More interaction between surgeons and restoring dentists is necessary. I strongly suggest that specialists only placing implants communicate constantly with those general practitioners restoring the implants, and that treatment plans be agreed upon by both parties.
I further suggest that dentists placing implants, whether general dentists or specialists, should have enough continuing education to feel competent in the procedures and limit themselves to the level of clinical difficulty with which they feel competent.
Finally, I suggest that dental implants are the last resort, and that there is nothing like a stable, functioning tooth.
Author’s note: Additional educational resources are available from Practical Clinical Courses, some of which relate directly to this article:
Two-day courses in Utah
- Implant Surgery—Level 1 and Level 2 with Dr. Gordon Christensen
One-hour CE videos
- Diagnosis and Treatment of Failing Implants (Item No. V2391)
- Simple, Inexpensive Implant Solutions for Edentulous Mandibles
(Item No. V2388)
For more information about these educational products, call (800) 223-6569 or
visit pccdental.com.
Reference
1. Derks J, Schaller D, Håkansson J, Wennström JL, Tomasi C, Berglundh T. Effectiveness of implant therapy analyzed in a Swedish population: Prevalence of peri-implantitis. J Dent Res. 2016;95(1):43-49. doi: 10.1177/0022034515608832.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.