Direct composite veneers for esthetic reconstruction
Case presentation by Ross W. Nash, DDS
Practice management considerations by Debra Engelhardt-Nash
Composite resin has become a versatile dental restorative. There are many good materials on the market today. Some have dentin, enamel, and incisal shades, while others have more limited shades. Some are microfill resins that can be highly polished, and some are hybrids or even nanohybrids with high filler content and high strength. Final results are less dependent on the particular material than they are the placement technique and artistic skill of the clinician. As an educator, I have had the opportunity to use many composite resins and found that nearly all of them can provide excellent results. Placed well in the proper clinical situations, I believe composite resin anterior restorations can be expected to last a minimum of five years and up to 10 years or more.
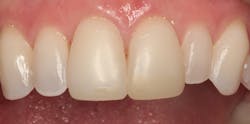
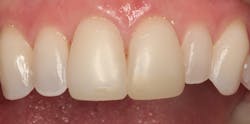
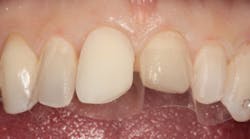
Figure 1: Direct composite resin veneers for Nos. 8 and 9 at 11 years
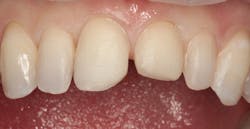
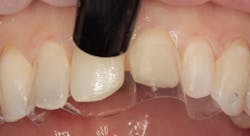
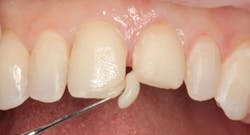
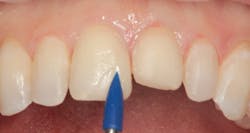
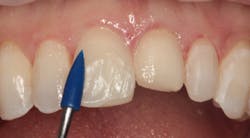
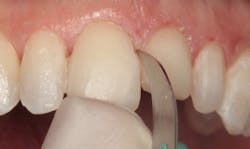
Figure 2: Maxillary central and lateral incisors prepared for new direct composite resin veneers
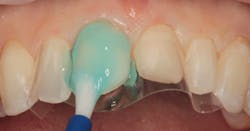
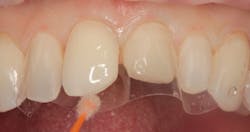
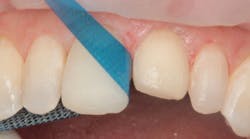
Figure 3: Etching gel applied to enamel
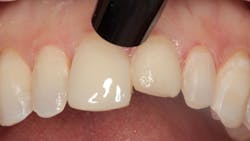
Figure 4: Etched tooth surface
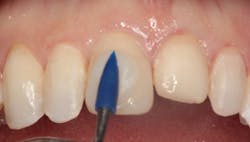
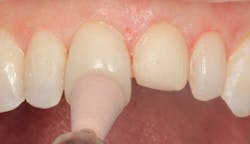
Figure 5: Bonding agent applied
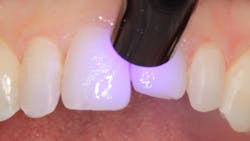
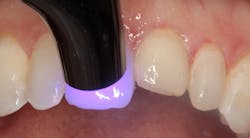
Figure 6: Bonding agent light cured
Clinical case
In Figure 1 you can see an image of a patient with direct composite veneers on her maxillary central incisors that I placed 11 years earlier. The material used was Four Seasons, a hybrid composite by Ivoclar Vivadent. The patient was a teenager who had broken her incisors. I wanted to provide a minimally invasive repair to last through her growth stage.
She recently wished to have them updated and direct veneers added on the lateral incisors. This time I chose Empress Direct, a nanohybrid composite also by Ivoclar Vivadent.
Clinical technique
Figure 2 shows the prepared teeth after the previous composite restorations were removed and the four teeth were prepared. The right central incisor was isolated with a celluloid strip and an etching gel was applied for 10 seconds (figure 3). The tooth was thoroughly rinsed with water from an air/water syringe and air dried. The etched surface can be seen in Figure 4. A universal bonding agent (Excite, Ivoclar Vivadent) was applied liberally (figure 5), thinned with air, and light-cured for 10 seconds with an LED curing light (figure 6).
Figure 7: Application of dentin shade
Figure 8: Contouring of dentin shade
Figure 9: Dentin shade light cured
Figure 10: Application of enamel shade
Figure 11: Enamel shade light cured
Figure 12: Application of incisal side
Composite application
A dentin shade was chosen to replace the chipped areas and diastema due to its more opacious nature, leaving room for an enamel shade with more translucency. Figure 7 shows the dentin shade being placed with a composite instrument. In Figure 8, a composite instrument is shown contouring the dentin shade. This layer was cured for 20 seconds with an LED curing light (figure 9). Then an enamel shade of composite was added to the entire facial surface (figure 10). This layer was light-cured for 20 seconds (figure 11). Finally, an incisal layer was added to the incisal third of the facial surface (figure 12). This layer was again light-cured for 20 seconds (figure 13).
Figure 13: Incisal shade light cured
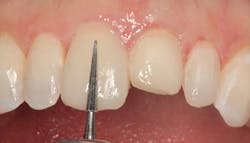
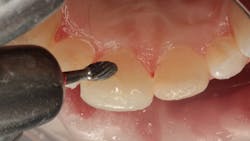
Figure 14: Facial contouring with flame-shaped carbide finishing bur
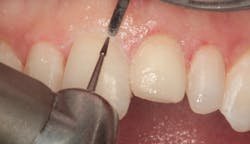
Figure 15: Margins are shaped with small carbide finishing bur
Figure 16: Lingual contouring using a pear-shaped carbide finishing bur
Figure 17: No. 12 surgical blade used to contour interproximal margin
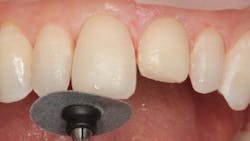
Figure 18: Aluminum oxide disc used to shape incisal edge and lingual angles
Figure 19: Aluminum oxide strips used to polish proximal surfaces
Figure 20: Composite polishing cup for high gloss
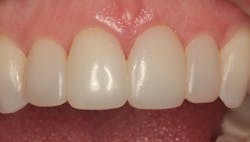
Figure 21: Final result at placement
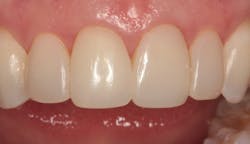
Figure 22: Five-year follow-up
Contouring
Though freehand sculpting was used to create basic anatomy, final contouring was needed. In Figure 14, a carbide finishing bur is shown contouring the facial surface to create the proper line angles and shape. The gingival margins are thinned and shaped with a small carbide finishing bur, and the gingival tissue was protected with a composite instrument (figure 15). Excess lingual composite was removed with a pear-shaped carbide finishing bur (figure 16). A No. 12 surgical blade was used to refine the proximal/gingival margins as seen in Figure 17. Incisal and proximal line angles were refined using an aluminum oxide disc (figure 18). Proximal surfaces were polished using aluminum oxide strips (figure 19). The final step was to polish the surfaces with composite polishing cups (figure 20).
Final result
In Figure 21, you can see the final result. Though the patient had her recare appointments provided by her local dentist, she returned in five years for a requested follow-up appointment. Figure 22 is an image of her restorations as they appeared at this appointment. As you can see, they are holding up well. I predict a life of at least 10 years as long as the patient continues to maintain her oral health as she has previously done.
Conclusion
Composite resin can be an excellent choice for minimally invasive and esthetic treatments. There are many choices for composite resins. In this case, I used Empress Esthetic and layered dentin, enamel, and incisal shades to achieve a realistic appearance with a nanohybrid composite resin.
Ross W. Nash, DDS, maintains a private practice in Huntersville, North Carolina, where he focuses on esthetic and cosmetic dental treatment. He is an accredited fellow in the American Academy of Cosmetic Dentistry. Dr. Nash lectures internationally on subjects in esthetic dentistry and has authored chapters in two dental textbooks. He is cofounder of the Nash Institute for Dental Learning in Huntersville, North Carolina.
Debra Engelhardt-Nash is a trainer, author, consultant, and presenter. She is the president of the National Academy of Dental Management Consultants, where she is a founding member. She is on the board of the American Academy of Dental Practice, and has served as a contributing editor for Contemporary Esthetics and Restorative Practice and Contemporary Dental Assistant magazines.
Practice management considerations
Offering composite restorations provides a solution for patients who may not be ready to invest in a costlier alternative such as porcelain. It may also be the right material selection based on the age of the patient or the clinical situation.
The doctor needs to create total team awareness of all treatment options that are being offered in the practice. It is often the team—patient coordinator, receptionist, dental assistant, and hygienist—who are asked about treatment alternatives or have the opportunity to introduce treatment choices to new patients and existing patients.
The more the team is educated on treatment modalities, the better prepared they will be to speak to patients about them. An in-office training may be required to help everyone on the team understand the advantages of composite resin direct-bonded restorations, the necessary armamentarium, and the selection of materials. Include in this training the communication skills required to talk to patients about these treatment alternatives.
Find answers to these questions about the procedure to ensure proper integration into the practice:
• What are we trying to accomplish?
• Why are we offering this treatment to our patients?
• What will we need to modify in order to integrate this treatment? (scheduling, materials, armamentarium, etc.)
• How will we communicate about this procedure to the team?
• What information does the team need to feel comfortable discussing this care with patients?
• How will we communicate with patients about this?
• What information do we need to provide patients?
• How will we determine our effectiveness?
• What methods will we employ to monitor our progress?
Answering these types of questions can help increase the effectiveness of implementing all types of changes in your practice.
Creating awareness of this treatment alternative for cosmetic and esthetic solutions will attract patients seeking to change the appearance of their teeth or smile with conservative treatment options at a reduced cost. The myriad of social media and consumers’ use of internet-learning resources offer great opportunities to present these treatment options to existing and potential new patients.