Solving zirconia occlusion challenges
Each month, Dr. Gordon Christensen answers a question from readers about everyday dentistry.
Q: Since zirconia indirect restorations have become the most frequently placed crown type, I have had significant challenges with occlusion. Most of the zirconia crowns I receive from several labs are made of “esthetic” zirconia, and I understand these crowns are weaker than the original zirconia formulation that was introduced into dentistry. Additionally, all of them have a layer of ceramic on the external surfaces that provides the color I have prescribed. However, if occlusion must be adjusted, the occlusal ceramic must be removed, resulting in a marked color change. Smoothing and polishing the zirconia is also a difficult task with often unacceptable outcomes. Do you have some suggestions?
Dr. Christensen: All dentists who place zirconia crowns are having the same challenges as you are. I have some potential solutions. As you probably know, the original zirconia formulation brought into dentistry about 12 years ago was previously used for many industrial purposes to replace steel. These ZrO2 materials contained 3 molar percent yttrium oxide Y2O3, (yttria), the normal oxide of the element yttrium. This addition creates a toughening mechanism that enhances the fracture properties of ZrO2, called transformational toughening. This property is especially important in zirconia crowns as it limits the propagation of cracks.
More about zirconia ... Solving challenges with zirconia and lithium disilicate crowns
The addition of more yttria also increases the translucency of the crowns. Since one of dentists’ main desires is increased translucency in crowns, manufacturers have added more yttria to form “esthetic” zirconia. However, there is a potential problem related to adding more yttria—the strength and transformational toughening of the zirconia are significantly reduced.
Clinical challenges with zirconia
In addition to the challenges you described, these are my conclusions on the clinical challenges with zirconia after observing its various formulations through the years.
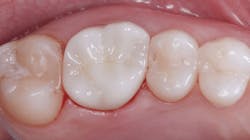
- Labs currently space occlusal contact of restorations, and the restorations usually are not in proper occlusal contact when we receive them (figure 1). Many restorations do not contact the opposing arch, requiring extrusion of the restored or opposing teeth to provide occlusal contact.
- Labs space restorations on the intaglio surfaces to allow the crown to seat without modification. This causes instability when attempting to seat restorations as well as potential improper seating, open contacts, and open margins. Margin fit of zirconia crowns is often open to normal vision.
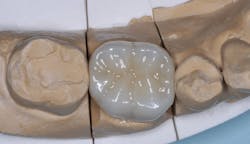
- The occlusal anatomy of restorations, which has been milled to the ideal characteristics of a milling library, often does not have desired anatomical contact with the opposing arch (figure 2).
- When the superficially placed stain and glaze are removed to adjust occlusion or anatomy, the underlying zirconia is usually mismatched with the superficial layer. This situation usually causes an unacceptable result in esthetic areas.
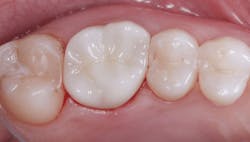
- The contact areas with adjacent teeth are often irregular or rough, causing food traps or difficulties with flossing. This necessitates finishing and polishing the zirconia, potentially causing an open contact (figure 3).
- Zirconia is very difficult to finish and polish. Even the slightest lack of occlusal harmony is difficult to adjust and smooth properly.
How do we reduce these challenges?
Unfortunately, most of the challenges we have identified are the standard with zirconia restorations. These problems are unlikely to change unless dentists and labs make efforts to correct them. I suggest that you contact your lab and discuss the challenges you’re having, because the lab may be able to reduce or eliminate some of those issues. It’s difficult because the crowns are made by computer milling and not by human hands. The changes we need will require more human involvement from both dentists and lab technicians to make good preps and impressions, and to use more thought when using computers and customizing settings to specific situations.
More about zirconia ... Successful cementing of zirconia crowns: Still a problem
Here are some suggestions as to how some of these challenges with zirconia can be reduced.
- More interaction and communication by dentists and technicians. Both groups can do better if they discuss the challenges, considering the understanding and viewpoints of each.
- More accurate soft-tissue management and scanning by clinical dentists, allowing clear display of margins and more precise scanning of elastomer impressions by techs, which will improve margin fit.
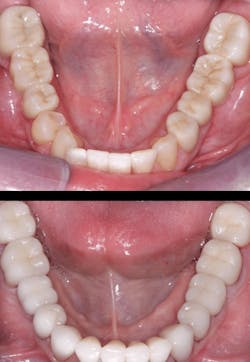
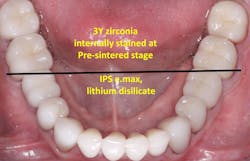
- Understand that different pucks of the same color of zirconia do not have the same color. For example, it’s easy to find different colors of “A2.” This makes elimination of superficial stain and glaze a problem. Internal staining of zirconia at the presintered stage needs to be simplified. More laboratory innovation is needed on how to simplify presintering internal staining of the stronger iterations of zirconia to require less need for external staining, which can be a somewhat temporary color in some situations (figure 4).
- More emphasis on labs to use the stronger version of zirconia (3Y, full-strength, LT, tetragonal) since research now shows the weaker iterations of “esthetic” (4Y, 5Y, cubic) zirconia have some breakage after only a few years (Clinicians Report Foundation TRAC in vivo research at six years). The same research shows no breakage of single 3Y full-strength zirconia at 11-plus years.
- Less spacing of crown occlusal and intaglio surfaces by laboratories can provide more firm and positive seating and ensure proper fit, tighter contact areas, and more accurate occlusion.
- Better adjustment and customization of crown occlusal anatomy by lab technicians to fit the specific anatomy of teeth on the opposing arch, and more adequate preps by dentists to allow this proper anatomy to be made.
- Better smoothing of contact areas by lab techs before sintering and smoothing contacts after placing stain and glaze. This probably requires slightly higher computer setting for tightness of contacts to allow for finishing and polishing.
- More education for both lab techs and dentists on how to finish and polish zirconia.
Finishing/polishing procedure for zirconia restorations
Since finishing and polishing zirconia seems to be a continuing problem for clinicians, I suggest the following relatively simple procedure. This procedure does not solve the esthetic problem encountered when removing superficial stain and polish, but it does provide a way to adjust occlusal surfaces of posterior teeth, which usually don’t have any problematic esthetic issues. This procedure can also be used for all surfaces of internally stained zirconia restorations since they aren’t required to have an external layer of stain and glaze.
This is only one of the successful methods you can use to finish and polish zirconia (figure 5). You may prefer a different procedure.
- Adjust only flat surfaces (not grooves and indentations) since no instrument can easily reach these areas.
- Use a fine diamond or worn diamond. Finish the surface tips of cusps, marginal ridges, facial and lingual surfaces (without stain or without esthetic impairment), or other relatively flat surfaces.
- Use emery discs to smooth the diamond scratches.
- Use garnet discs to smooth the scratches from emery discs.
- Use commercially available zirconia finishing kits. Examples: Jiffy Universal (Ultradent), All-Ceramic Polisher (Cosmedent), Dialite ZR Polishers (Brasseler), and others.
- Polish the zirconia. Example: Dialite wheels (Brasseler).
- Do a final polish. Example: DiaShine.
Summary
Currently, zirconia is the most frequently used indirect restoration in the US. It’s working well, but it isn’t without complications. I’ve identified some of the challenges we have with zirconia and offered suggestions for manufacturers, dental laboratories, and practicing clinicians that will help reduce or eliminate the issues.
Editor's note: This article appeared in the December 2023 print edition of Dental Economics magazine. Dentists in North America are eligible for a complimentary print subscription. Sign up here.
Author’s note: The following educational materials from Practical Clinical Courses offer further resources on this topic.
One-hour videos:
- Strong, Comfortable, Esthetic Rehabilitations with Zirconia (Item #V1942)
- Foolproof, Fast Single-Crown Restoration (Item #V1980)
Two-day hands-on courses in Utah:
- Faster, Easier, Higher Quality Dentistry with Dr. Gordon Christensen
- Restorative, Esthetic, Preventive Dentistry with Dr. Gordon Christensen
- Simplifying Complex Treatment with Dr. Gordon Christensen
For more information, visit Practical Clinical Courses or call (800) 223-6569.
Gordon J. Christensen, DDS, PhD, MSD, is a practicing prosthodontist in Provo, Utah. He is the founder and CEO of Practical Clinical Courses, an international continuing education organization founded in 1981 for dental professionals. Dr. Christensen is cofounder (with his wife, Rella Christensen, PhD, RDH) and CEO of Clinicians Report.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.