Clinical case studies: Restoring posterior caries lesions on high-caries-risk patients with a glass-hybrid restorative material
Ideally, restoring caries lesions should not be different from managing dental caries. It starts at the person level with behavioral modification of risk factors and chemotherapeutic interventions targeted at modifying biofilm and promoting chemistry to support remineralization. Glass ionomer restoratives and sealants are used to manage caries lesions chemically at the tooth level. These case studies focus on use of a glass-hybrid restorative material as a long-term posterior restoration in high-risk caries populations.
Newer glass-based restoratives
Currently, glass ionomer cement (GIC) is the only restorative material that is water based and has a significant anticaries effect.1-3 As with the other dental materials, glass ionomer restoratives and sealants have continued to evolve since their introduction. A more recent category of glass-based materials is called glass-hybrid, marketed as Equia Forte HT. The hybrid term refers to the mixture of different sizes of glass particles, which improves handling and mechanical properties as compared to conventional glass ionomers.4 Equia Forte HT can be used as a long-term restorative for stress-bearing and nonstress-bearing restorations in adults and children.
GI restoratives, sealants for high-caries-risk patients
GIC is hydrophilic and chemically bonds to the tooth5 in contrast to composite, which is hydrophobic and micromechanically retained. GIC is biocompatible, has thermal expansion like enamel and dentin, and is compatible with a moist environment. A key benefit of using GIC in high-caries-risk patients is the long-term release of fluoride and other ions that support remineralization, resulting in acid-resistant fluorapatite.6,7 Studies have demonstrated less recurrent decay at the margins8,9 and adjacent surfaces.10,11 As fluoride ions are released from the GIC, the GIC is able to be “recharged” by fluoride ions from other sources, such as fluoride toothpaste and other fluoride-containing products.12 The resulting anticaries properties of GIC restorations are confirmed in a 2016 systematic review by Mickenautsch.3
Mitigating composite resin shrinkage in restorative dentistry
Reducing composite resin failures
Chemical changes also occur under the restoration at the tooth-restorative material interphase. The chemical bond to tooth mineral is a result of transfer of ions between GI and tooth.5,13 This interface is sometimes called the “chemically fused” zone.13-15 Ngo demonstrated that the chemically fused zone was actually remineralized fluorapatite and termed this “internal remineralization.” Thus, GIC creates a remineralized marginal seal that is acid protected.13
The chemical seal of GIC at the margins is ideal to pair with selective caries removal techniques. In selective caries removal, the carious tissue is removed from the perimeter of the lesion, while the deeper areas of the lesion are not excavated. This prevents mechanical pulp exposure and preserves the health of an asymptomatic vital pulp.16-18 By establishing a seal at the perimeter margins, GIC prevents a nutrient source from reaching any remaining bacteria. This halts further acid production and demineralization, resulting in lesion arrest.16,17
Use of bulk-fill conventional glass ionomer restoratives and sealants is fast and economical because multiple teeth can be restored or sealed on high-risk patients without time-consuming layering and light-curing or use of a rubber dam, often with little to no local anesthesia. For all these reasons, GIC is the most logical restorative material for patients with active caries lesions.
Glass-hybrid in posterior restorations
With the decreased use of amalgam, there is a current need for a high-strength restorative material to use with high-risk, caries-active individuals. Equia Forte HT is an improved version of glass-based materials. HT stands for “high translucency,” which delivers improved esthetics. Glass-hybrids improve the conventional glass matrix by adding reinforced ultrafine, highly reactive glass particles and a high-molecular-weight polyacrylic acid resulting in stronger cross-linking and improved mechanical properties.19
In a pivotal long-term randomized controlled trial, Gurgan et al. compared the durability of Equia restorations to microfilled composite resin in class I and II caries lesions over a 10-year period. The study concluded that both restorative materials showed an acceptable success rate in the restoration of class I and class II caries lesions during the 10-year follow-up.20
In a different multicenter randomized controlled trial published in 2020, Ivana et al. compared Equia Forte to a nanohybrid resin composite using a split-mouth design. The glass-hybrid restorative system and nanohybrid resin composite both showed good clinical performance in moderate-to-large two-surface class II restorations.21
These two randomized controlled trials should dispel any myths that glass-based materials will not hold up in the stress-bearing areas and should only be used as a temporary restoration. The following cases demonstrate the use of Equia Forte HT in minimally invasive preparations, utilizing selective caries removal to preserve tooth structure and pulp integrity.
Case 1: Caries lesion approaching the pulp
Figure 1 shows a large radiolucency on the mesial and a small radiolucency on the occlusal of tooth 31. Figure 2 shows an initial caries lesion on the distal pit and a leaking occlusal composite. Tooth 31 was sensitive to cold but normal to chewing, bite, and heat. Selective caries removal was used to prevent pulp exposure and preserve the marginal ridge.
A glass-hybrid (Equia Forte HT) was chosen due to its strength and similar coefficient of thermal expansion. The coefficient of thermal expansion did not stress the marginal ridge, and the remineralization characteristics of glass-hybrid prevented the need for root canal therapy.
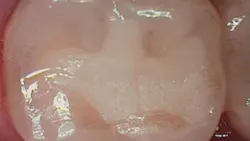
Figure 3 shows the final restoration immediately after placement. Figure 4 shows the final restoration of an initial caries lesion on the buccal. The clinician anticipated maturation of the glass-hybrid in choosing a lighter shade of A2, which initially appeared much too light. A slightly darker shade may have been more appropriate.
Figure 5 is a 36-month follow-up bitewing radiograph demonstrating excellent support of the significantly undermined enamel and deposition of secondary dentin in the mesial pulp horns. Figures 6 and 7 show the occlusal and facial restorations respectively after 18 months. Notice the improvement in shade.
Case 2: Replacing amalgam, fractured tooth, undermined enamel
What began as a routine replacement of a fractured amalgam restoration (figure 8) developed into a larger restoration of a fractured tooth (figure 9). It is often difficult to know how much dentin remains when replacing old restorations. The amalgam restoration preparation undermined the buccal cusp enamel, resulting in asymptomatic vertical fractures of the pulpal floor (figure 9). Undermined enamel is not a concern when using glass ionomer restoratives, because there is no contraction shrinkage; the chemically fused zone is strongly bound and re-supports the enamel. A glass-hybrid (Equia Forte HT) was chosen due to its strength and similar coefficient of thermal expansion as well as the need to re-support the undermined enamel without causing “craze lines” often occurring in traditional light-cured composite restorations.
Figure 10 shows the final restoration. The ionic chemical bond of glass-hybrid (the chemically fused zone) to tooth structure will strengthen the tooth more than the previous mechanically retained amalgam.
Summary
Glass-hybrid restorations have unique physical characteristics that support their use in class I and II restorations. Chemical ionic bonding to enamel and dentin, development of fluorapatite, caries-resistant enamel margins, and re-supporting weakened tooth structures of extremely deep caries lesions all support use of glass-hybrid in posterior restorations. Mastering these techniques opens the door to faster, more economical, and perhaps better restorations for high-caries-risk patients.
Disclosure: The authors received honoraria from GC America.
Editor's note: This article appeared in the January 2023 print edition of Dental Economics magazine. Dentists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Ngo HC, Mount G, Mc Intyre J, Tuisuva J, Von Doussa RJ. Chemical exchange between glass-ionomer restorations and residual carious dentine in permanent molars: an in vivo study.
J Dent. 2006;34(8):608-613. doi:10.1016/j.jdent.2005.12.012 - Smales RJ, Ngo HC, Yip KHK, Yu C. Clinical effects of glass ionomer restorations on residual carious dentin in primary molars. Am J Dent. 2005;18(3):188-193.
- Mickenautsch S, Yengopal V. Caries-preventive effect of high-viscosity glass ionomer and resin-based fissure sealants on permanent teeth: a systematic review of clinical trials. PLoS One. 2016;11(1):e0146512. doi:10.1371/journal.pone.0146512
- Joshi G, Heiss M. Glass-hybrid technology for long-term restorations. Compend Contin Educ Dent. 2021;42(Suppl 1):2-5.
- Yoshida Y, Van Meerbeek B, Nakayama Y, et al. Evidence of chemical bonding at biomaterial-hard tissue interfaces. J Dent Res. 2000;79(2):709-714. doi:10.1177/00220345000790020301
- Gorton J, Featherstone JDB. In vivo inhibition of demineralization around orthodontic brackets. Am J Orthod Dentofacial Orthop. 2003;123(1):10-14. doi:10.1067/mod.2003.47
- Forsten L. Fluoride release and uptake by glass ionomers. Scand J Dent Res. 1991;99(3):241-245. doi:10.1111/j.1600-0722.1991.tb01891.x
- Mickenautsch S, Yengopal V, Leal SC, Oliveira LB, Bezerra AC, Bönecker M. Absence of carious lesions at margins of glass-ionomer and amalgam restorations: a meta-analysis. Eur J Paediatr Dent. 2009;10(1):41-46.
- Mandari GJ, Frencken JE, van’t Hof MA. Six-year success rates of occlusal amalgam and glass-ionomer restorations placed using three minimal intervention approaches. Caries Res. 2003;37(4):246-253. doi:10.1159/000070866
- Forsten L. Fluoride release of glass ionomers. J Esthet Dent. 1994;6(5):216-222. doi:10.1111/j.1708-8240.1994.tb00862.x
- Hicks J, Garcia-Godoy F, Donly K, Flaitz C. Fluoride-releasing restorative materials and secondary caries. J Calif Dent Assoc. 2003;31(3):229-245.
- Cranfield M, Kuhn AT, Winter GB. Factors relating to the rate of fluoride-ion release from glass-ionomer cement. J Dent. 1982;10(4):333-341. doi:10.1016/0300-5712(82)90028-8
- Ngo H, Ruben J, Arends J, et al. Electron probe microanalysis and transverse microradiography studies of artificial lesions in enamel and dentin: a comparative study. Adv Dent Res. 1997;11(4):426-432. doi:10.1177/08959374970110040801
- Sennou HE, Lebugle AA, Grégoire GL. X-ray photoelectron spectroscopy study of the dentin-glass ionomer cement interface. Dent Mater. 1999;15(4):229-237. doi:10.1016/s0109-5641(99)00036-6
- Ngo H, Mount GJ, Peters MC. A study of glass-ionomer cement and its interface with enamel and dentin using a low-temperature, high-resolution scanning electron microscopic technique. Quintessence Int. 1997;28(1):63-69.
- Thompson V, Craig RG, Curro FA, Green WS, Ship JA. Treatment of deep carious lesions by complete excavation or partial removal: a critical review. J Am Dent Assoc. 2008;139(6):705-712. doi:10.14219/jada.archive.2008.0252
- Ricketts DNJ, Kidd EAM, Innes N, Clarkson J. Complete or ultraconservative removal of decayed tissue in unfilled teeth. Cochrane Database Syst Rev. 2006;3:CD003808. doi:10.1002/14651858.CD003808.pub2
- Schwendicke F, Frencken JE, Bjørndal L, et al. Managing carious lesions: consensus recommendations on carious tissue removal. Adv Dent Res. 2016;28(2):58-67. doi:10.1177/0022034516639271
- Moshaverinia M, Navas A, Jahedmanesh N, Shah KC, Moshaverinia A, Ansari S. Comparative evaluation of the physical properties of a reinforced glass ionomer dental restorative material. J Prosthet Dent. 2019;122(2):154-159. doi:10.1016/j.prosdent.2019.03.012
- Gurgan S, Kutuk ZB, Yalcin Cakir F, Ergin E. A randomized controlled 10 years follow up of a glass ionomer restorative material in class I and class II cavities. J Dent. 2020;94:103175. doi:10.1016/j.jdent.2019.07.013
- Miletić I, Baraba A, Basso M, et al. Clinical performance of a glass-hybrid system compared with a resin composite in the posterior region: results of a 2-year multicenter study. J Adhes Dent. 2020;22(3):235-247. doi:10.3290/j.jad.a44547
About the Author

Douglas A. Young, DDS, EdD, MS, MBA
Douglas A. Young, DDS, EdD, MS, MBA, professor emeritus at the University of the Pacific, was one of the founders of the CAMBRA Coalition, American Dental Education Association Cariology Section, and the American Academy of Cariology. He is a cariology consultant for the ADA. A worldwide presenter and author on caries management using minimally invasive dentistry, he receives industry support from GC America, Elevate Oral Care, Oral BioTech, and others.
Updated January 3, 2023.