The economics of hygiene
Annette Ashley Linder, RDH, BS
During a break at a recent seminar I was presenting, a doctor said, "I am hemorrhaging in hygiene. My scheduling coordinator says there is no room for hygiene patients, yet I know we have openings every day. I am not sure how much hygiene time I really need, and I'd like to know what to do just to break even in hygiene."
The doctor went on to say that initially she thought it was just a seasonal slump, perhaps a slow period. Nevertheless, the situation had not improved and now she was worried because her own schedule had openings; she was struggling to keep her production levels. This doctor had been practicing more than 15 years in the same community. The practice was growing by 25 to 30 new patients each month. Does this sound familiar?
My consultation analysis of patient retention, or recall, and the hygiene department revealed the following:
1) The office lacked a clear, written patient-retention system.
2) No one was responsible or accountable for patient retention (recall).
3) Forty-eight percent of patient charts in the central file were overdue. (No one was aware of this.)
4) Ninety-two percent of hygiene revenues were generated for prophys.
5) Daily scheduling efficiencies were 86 percent in hygiene.
The health of the recall determines overall stability and health of the dental practice. Patient return rates are an essential part of office statistics, yet many doctors do not include this data in their business reviews. In addition, hygiene will never pay for itself, let alone be profitable, when preventive prophylaxis procedures account for 90 percent of revenue and when scheduling is deficient.
In the aforementioned case, the hygiene schedule "appeared to be full, most of the time." According to the staff, there wasn't "any room in the hygiene schedule" for patients to be seen, so the team thought they were on target. While recruitment of new patients was moving in the right direction, maintaining patients of record had fallen because the hygiene schedule appeared full. The analysis revealed that the office did not have enough hours to accommodate patients and it was understaffed in hygiene hours. Patients were coming in the front door, then falling into the land of overdue patients who are lost in the system. The result, which often takes six or more months before someone notices, is that when patients do not return for preventive and maintenance care, they do not return to see the dentist. When patient return rates fail, dentists ultimately slow down and productivity declines. The most ironic part is that many of the "overdue" patients are excellent, long-term patients of record who have had extensive dentistry in the past. They know you, trust you, have relationships with you and your team, and they accept your treatment recommendations. It has been suggested that 70 percent to 80 percent of dental treatment is generated at oral health care appointments. Dental hygiene appointments are primary sources for patient education, restorative and aesthetic case acceptance, and practice building. Today's competitive environment demands effective management principles and guidelines to monitor patient retention.
Smart business requires record keeping. What used to be difficult and time-consuming tasks are now easily managed by computer systems. Remember all those metal boxes filled up with ledger cards and lined up at the desk? Anyone remember the pegboard system? Thanks to technology and computers, this is no longer the case with today's dental management software systems. Retrieving information requires only a mouse click.
Start with the questions
• What is my active patient base?
• How many patients should we see annually in hygiene (recall) to maintain this base?
• How many hygiene days/hours do I need to meet my patient base and stay healthy?
• What is my target growth goal?
• Who is responsible, and is it a struggle to keep the hygiene schedule full?
• Is hygiene operating at full capacity? Is hygiene productive and efficient?
• If I do not have enough days, what strategy should I explore? Add a hygienist? Add a hygiene assistant working with two treatment rooms? Extend office hours to accommodate the patient volume? Bring in another dentist?
• Is the practice growing? If so, why? What are we doing right? Let's do more of it.
• Is the practice shrinking? Why, and what do we need to fix?
The patient retention formula in Table 1 provides answers. Use the formula to calculate your practice's numbers. The data will assist you in business planning for staffing needs, facility needs, equipment and supplies, practice growth, and development.
A closer look at the formula
1) Know your active-patient/core-patient base number. An "active patient" has been in within the last 18 to 24 months and has received regular care, prophy, or perio. He or she is not a patient who came in six years ago as an emergency, had a tooth extracted, and then never returned for a new-patient appointment.
Set achievable goals. While setting a standard of 90 percent to 95 percent effective in the daily hygiene schedule is an achievable goal, anticipate a 10 percent to 15 percent normal attrition rate in overall patient retention. People move, die, change insurance, and change dentists because you "are not on the list," etc. No one retains 100 percent of patients, hence the 85 percent.
2) Understanding attrition reiterates the importance of gaining new patients. Every practice needs a steady flow of new patients. The number of new patients needed requires personal analysis, preferences, goals, and directions you wish to take your business, practice, and life.
The patient retention formula — or as the doctor asked, "How much hygiene do I need?" — must include a periodontal component. These are the patients who require active periodontal treatment and/or have received periodontal therapy and are now appropriately scheduled at three-month intervals for periodontal maintenance, 4910. Twenty-five percent is conservative and realistic. Translation — a quarter of hygiene patients are scheduled for codes 4341, 4342, 4355, 4910, 4381 — not prophys. Track this data with a procedures analysis computer report for the periodontal codes. If you come up short, discuss periodontal protocols with your hygiene team. Are you providing periodontal examinations and assessments routinely on all patients? Are your treatment plans current and customized with site-specific, individualized therapy based on patients' clinical and risk factors — health status, medications, smoking? The six-month cleaning and check-up is not a standard model for optimum oral health, particularly in light of the latest research demonstrating a link between systemic health and periodontal infection and inflammation.
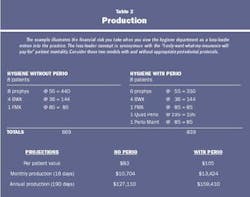
Many practices I work with have non-prophy rates of 30 percent to 45 percent. These teams have done great jobs educating and enrolling their patients in clinically appropriate care. Patients understand that the interval of time between appointments is based on their clinical and health requirements — not just what their insurance may dictate. Practices that implement non-surgical periodontal therapy protocols consistently report positive effects. They have healthier patients who are more educated and actively involved in periodontal and oral health. They ask about comprehensive dentistry and accept treatment plans for optimum oral health. Additionally, these practices experience significant increases in practice productivity. (See Table 2.)
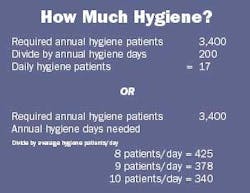
3) In this section, determine the recall-to-patient-retention ratio by dividing patients seen by the required number of patients. In this example, it is 1,620 divided by 3,480, or a 46.5 percent recall effectiveness rate.
4) This example is typical of U.S. dental practices: One hygienist accommodates eight to nine patients a day, 16 days a month, or 190 days a year.
The practice requirements for an 85 percent rate of patient retention is 3,400 annual patients. Total hygiene patients for the year equals 1,600, resulting in a shortfall deficit of more than 1,800 patients. Translation: Half of patients are lost in the system, sitting in the central file, overdue, and unnoticed. When I consult these practices, I typically find thousands of dollars of "unscheduled" dental treatment sitting in those same charts.
Based on that, here are two examples for calculating how much hygiene:
What to do
1 Review your office procedures for ongoing patient retention and reactivation of overdue patients. Document, set goals, revise, and designate the team member responsible. Use the patient retention monitor and establish the baseline. Review every quarter to determine if you are on target to meet practice requirements. Waiting until the end of the year means you have lost 12 months of good production capabilities. In addition, lost hygiene patients quickly slow down doctors' schedules. The result is fewer restorative patients seen, and the total practice production declines.
2 Perform a monthly review of daily hygiene scheduling rate with a target goal of 93 percent minimum. Calculate by dividing total units available by total units actually used (patients seen).
3 Perform a monthly analysis of hygiene procedures to assure periodontal/practice health. Good communication skills, sound management principles, and organized, clinically appropriate periodontal, preventive, and recall protocols will enable you to bring your hygiene department and the entire practice into clinical excellence and profitability.