Outcomes-based Practice..Part 5
By David W. Chambers, EdM, MBA, PhD
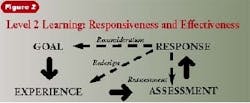
Level 2 Learning focuses on reconsideration, redesign, and reassessment - techniques used to change the system itself.
Practitioners who don't pay attention to their outcomes don't learn from their experiences; they just react. Such doctors are easy to identify. They are always complaining about uncooperative patients, intrusive insurance companies, lazy staff, and gouging suppliers. They are right - somebody else is running their practices.
Level 1 Learning, quality assurance, uses practice outcomes, but in a limited fashion. The operative question is, "Can I get by if I find and eliminate enough of the bad outcomes that somehow seem to crop up?" While it is important not to turn bad examples loose on the public, Level 1 Learning is expensive, because inspection and correction become institutionalized, dooming the practice to repeating the same mistakes continually.
The focus on efficiency characteristic of Level 1 Learning also produces psychological damage. Closed systems, where the goal is perfection measured against a fixed ideal, are a setup for boredom and burnout. Initial successes that drive out gross inefficiency are fun in the beginning. But once a system has eliminated all but the random variation inherent in it, no further efforts at improvement produce predictable results. This leads to the frustrating situation where additional effort produces no gain and surprises remain. Ask any golfer what I'm talking about. When better results are no longer possible, the effort turns to minimizing input, cutting costs, and turning performance over to habit. The passion is gone. The goal of efficiency, preached so successfully by consultants, has stolen the heart of the profession.
Some authors claim that efficiency improves the level of performance and its speed. There is just enough truth in this observation to make it dangerous. Most of the improvement brought about by efficiency comes from reducing the wide swings of variation in poorly standardized systems. As shown in Figure 1, System A and System B both have the same average level of performance. System A, however, has only the variation logically inherent in that system. System B has system variation plus the variation caused by inefficiency. If we assume that any performance below the horizontal line produces a defective result, System B will cause more problems, even though, on average, it is the same as System A.
The same peculiar relationship exists with regard to speed. Expert clinicians are not faster than novices; they are more efficient. I have videotaped dentists of varying skill levels and recorded the duration of each movement with a stop watch to satisfy myself on this point.
Fifteen years ago, a psychologist named Genter studied novice and expert typists. He found that novices actually were faster than the experts when asked to strike the same key over and over again. What made the expert typists so good was the fact that while their left small finger was typing the letter "a," their right little finger was positioning itself over the "p," and their mind already was looking for the "u."
Skill at the procedural level of dentistry is actually a function of expertise at the higher practice level. Successful practices are determined by yet a higher level of professional development. The details of a practice are controlled by larger patterns grounded in the dentist's values. We will explore this finding later in some detail.
To escape the trap of efficiency, it is necessary to move to Level 2 Learning. In Level 2 Learning, a new range of responses to outcomes is available. Level 1 Learning focuses on rejecting and reworking the results of the system. Level 2 Learning focuses on reconsideration, redesign, and reassessment, techniques used to change the system itself. (See Figure 2.)
Reconsideration means changing the purpose of the procedure or the practice. Out-comes from work in cariology have changed the meaning of "watching" a white spot on an incipient lesion. Formerly, "watch" meant wait for an optimal time to restore the lesion; now, the response in some offices is to trigger intervention designed to reverse the carious process. Such thinking is available in literature and in courses, but across the nation, dentists are exploring these alternatives on their own. On a more massive scale, dentistry is redefining itself to include elective procedures to enhance the appearance of patients, invisible adult orthodontics, and whitening procedures. No national conference or set of evidence-based papers triggered this reconsideration of the goals of dentistry. It is the result of many thousands of dentists experimenting in their own practices.
Requirements for good goals include the following:
- The goals of one level in the practice must be consistent with the goals at higher levels and, ultimately, with the personal values of the dentist.
- The goals must be written - they need not be expressed in terms of numbers, but the dentist must commit to their achievement.
- The goals must be justifiable - this does not mean you can always convince everyone that they should have the same goals you do, but you should not be ashamed to explain the reasons behind the goals you have chosen.
- The goals should be stable over time - the higher the goal, the longer it should be operative.
Redesign of experiences is an obvious way to improve a dental practice. This means switching to a new impression material, increasing the number of days of hygiene, dedicating two minutes of each appointment to conversation with patients, etc. Redesign is the preferred alternative to reject and rework, because it reduces the number of defective results and the cost of managing them. Redesign focuses on effectiveness; reject and rework emphasize efficiency.
The rules for redesign include:
- Establish reasonable efficiency before pursuing effectiveness. It is a waste of time to improve a practice that isn't under control.
- Improve those things that matter most.
- Use testing cycles guided by goals and assess ment for continuous improvement.
- Manage the reactions to change as well as the change itself.
- Verify that changes really have resulted in improvements.
The third response in Level 2 Learning is reassessment. The use of outcomes to improve a practice requires that the results of experience be compared against the goal. Human nature is notoriously subject to self-confirming perceptions; the more one believes in the method used and depends on its success, the less likely one is to assess results. Outcomes-based practice is not about determining success or failure - a different mindset is needed. Assessment drives continuous improvement rather than blame. There is no right or wrong, only better. Assessment often is dodged on the grounds of cost. Many naturally occurring events in practice can be recorded easily without adding to expenses. The number of procedures redone is always recorded in the charts. So is the number of preauthorizations returned, treatment plans accepted, materials used, and so forth. The real expense comes in collecting and analyzing the data. Computers will help in this regard, but every method I will present for outcomes-based practice can be accomplished with paper and pencil.
The basic rule is that the expected cost of assessment should never exceed the expected cost of practice improvements that result from using it. Normally, the largest cost for assessment is psychological. There is a fear of finding that something really does need to be changed or discovering that the solution is something other than pushing harder. Remember the old admonition: "As you climb the ladder of success, pause from time to time to make certain the ladder is positioned against the correct wall."
Reassessment is a good option when there is a sense that practice goals are not being effectively measured. It is a terrible waste to measure the number of new patients entering your practice when you should be measuring the number of new treatment plans accepted. The waste comes both from the hours spent collecting numbers and the lost opportunity for improvement. Good assessment that balances goals and experiences requires ingenuity and honesty. Practices commonly espouse the goal of putting a patient's interest first and measuring it by the bottom line. There also is a common confusion between dentistry and oral health. The measures of the decayed, missing, and filled teeth or surfaces (DMF) is highest (worst health) for women in the United States, precisely the group that goes to the dentist most often.
The requirements for good assessment include:
- Assessment must be representative of the goals - not a comprehensive definition of each goal, but something others would recognize as essential to or a major part of the goals.
- Assessment must be tracked over time. The method for measurement and its interpretation should not be changed from one assessment to the next.
- The range of possible results should be in the middle. Assessment should not crowd at the top or bottom.
- Assessment must be cost-effective; it must add net value to the practice to engage in assessment.
But remember, all assessment systems are cost-ineffective for dentists who have no stomach for making changes.