Ask Dr. Christensen
by Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e–mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: treatment plan, complex rehabilitation therapy, treatment, segments, diagnosis, dental benefits, occlusion, Dr. Gordon J. Christensen.
Q I have many patients who need comprehensive dentistry, but who cannot afford to have all of the treatment performed at one time. How can I accomplish complex rehabilitation therapy for patients who have significant financial resource limitations?A Your question is one of major importance, since the median income of typical American families is about $48,000 per year, and we often see treatment plans approaching that level. Such costs are obviously not feasible for many families. In fact, most typical patients cannot afford the cost of major oral rehabilitative therapy if it is done all at once.I have practiced in both affluent and low–to–moderate income locales where families have several children. The oral needs of many of these adult patients are frequently significant. When a high–cost treatment plan is presented to low– and middle–income adults with children, their immediate response is to have their teeth extracted and artificial dentures placed in their mouths.
Incremental treatment is one of the affordable ways to treat these patients and maximize the third–party payment benefits. Dividing oral rehabilitation treatment during a period of years can be the solution for many patients to receive adequate care.
The following information will tell you how to perform complex comprehensive therapy in segments:
1) Diagnosis and treatment plan: Accomplish a complete diagnosis and treatment plan. Not doing this results in the dentist making a less–than–adequate plan which compromises the eventual treatment. I usually have a staff person perform these tasks after I have introduced myself to the patient and before I discuss the alternative treatment plans. Educated, motivated staff members can easily collect this data. Dental hygienists or dental assistants can be trained and educated to legally do the diagnostic data collection.
The tasks included in this staff–oriented diagnostic appointment are:
- Filling out informational forms
- Taking panoramic radiographs
- Taking bitewing radiographs
- Taking periapical radiographs
- Making diagnostic casts on the first appointment
- Providing education about all aspects of the patient's needs
- Using an intraoral TV demonstration to show all areas of the patient's mouth
- Charting all periodontal pockets of 3 mm or more
- Recording blood pressure
- Charting of previous restorations or endodontic therapy
- Charting of obvious carious lesions
- Vitalometer testing of suspect teeth
- Performing examination for soft–tissue lesions
- Determination of the presence of any occlusal disease
- Charting missing teeth
- Observing and noting any other oral pathosis
- Determining patient's desires for treatment
After completing the data collection and discussing it with the staff person who collected it, I usually spend about 10 or 15 minutes analyzing the data and explaining the treatment plans to the patient.
2) Discussion of the patient's ability to pay — I suggest being candid, yet empathetic, about the cost of oral therapy and the need to have adequate financial ability to pay for extensive oral care.
3) Discussion of the patient's dental benefit plan — About 70% of American dental patients have at least some dental benefits provided by their employers. The amount these third–party companies pay for oral therapy is low and does not approach our standard and customary fees; however, these benefits do represent a token amount toward the total payment for therapy. They also can be spread across a period of years to maximize their effect.
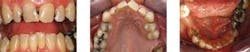
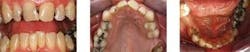
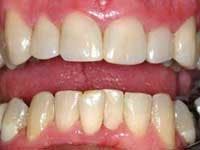
4) Determination of the patient's ability to get a loan for the services — Some patients with good credit ratings are willing to get a loan, pay the interest on it, and have the treatment performed as soon as possible. This is the ideal situation, but let's assume the patient cannot or will not get a loan. Such a patient is shown in Figs. 1, 2, and 3.
5) Help the patient decide which treatment plan he or she prefers. I usually say something like, "If I were you and had the financial ability to pay for these services, I would probably do this plan." At this point — after considering all aspects of the agreed–upon plan — I suggest segmenting the treatment into several logical categories such as:
Year one: Removal of any condemned teeth, periodontal therapy, placement of provisional restorations in any deeply carious teeth, bleaching teeth if desired, placement of temporary removable partial dentures (flippers) to replace any esthetically compromised areas, endodontic therapy as needed anywhere in the mouth, treatment of at least the six upper anterior teeth, and placement of the patient on an appropriate preventive regimen.
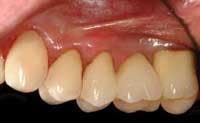
This amount of treatment may be more than the patient can afford in one year, even when using any third–party benefit that is present. If so, segment the first portion into more piecemeal treatment, doing only the mandatory therapy first. As an example, if a significant amount of therapy has been needed before treating the six anterior teeth, these teeth may be treated in the second year. However, I prefer treating the upper anterior teeth in the first year if possible. Often, the anterior teeth can be treated conservatively rather than using crowns, to provide even more motivation for the patient to continue with the therapy. (See Fig. 4.)
Year two: Select the most debilitated quadrant of posterior teeth, and do whatever needs to be done in that quadrant. This treatment will probably amount to anything up to four crowns, or some implants and implant–supported prostheses. (See Fig. 5.)
Years three, four, and five: Treat each remaining quadrant, selecting the worst areas first. At the completion of each segment, a thorough analysis of occlusion should be made and appropriate occlusal equilibration accomplished.
6) Third–party payment: Using the concepts we have discussed over each of the five or more years, patients receive the maximum benefits from their third–party plans. Of course, the treatment could be extended further than the five plus years, but, in my experience, most patients can afford the cost of segmenting the treatment into the sequence we have suggested.
7) Opening the vertical dimension of occlusion: The previous treatment sequence is best suited for patients with most of their teeth still salvageable and who do not need the vertical dimension of occlusion opened. More radical treatment requires a different treatment plan, including the use of interim occlusal splints.
8) Patient satisfaction with segmented treatment: I have accomplished many full–mouth rehabilitations using the sequence described in this article. Using this treatment concept, patients who could not afford therapy have been able to do so. They become very confident about your abilities after working with you over an extended period of time, and they become good sources of referrals. Occlusion is stabilized better than if you performed the treatment all at one time. Preventive therapy can be observed and modified if necessary.
PRACTICAL CLINICAL COURSES (PCC) will soon have a one–hour live patient DVD available, showing a full–arch rehabilitation from start to finish. Ask for Video No. 1934, "Complex Oral Rehabilitation." Call (800) 223–6569 or visit www.pccdental.com for details on the video.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing–education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.