The benefits of a soft–tissue laser
by David P. Reichwage
For more on this topic, go to www.dentaleconomics.com and search using the following key words: diode laser, soft–tissue laser, periodontology, periodontal surgery, gingival, gingiva, restorations, treatment–planning, Dr. David Reichwage.
We have incorporated a diode soft–tissue laser into our practice for the past eight years. We have found the benefits to be many and far–reaching for our patients. The laser enhances placement of contemporary restorative materials, as well as enables the soft–tissue corrections in form and symmetry. It also can be used as part of the armamentarium in conservative, nonsurgical periodontal treatment.
All ceramic bonded restorations using contemporary materials and techniques for esthetic enhancement of anterior teeth are very predictable in terms of function and appearance. The long–term success of bonded restorations depends on maximizing the health and integrity of the gingival tissues. The gingival symmetry that embraces the elements of smile design requires optimal soft–tissue health at the free gingival margin, absence of bleeding on probing or scaling, attached gingiva that is stippled and of normal color, and sulcus pocket depths of 1 mm to 3 mm.
These same principles apply to the natural dentition as well. They are guidelines to construct a "blueprint" to maximize soft–tissue esthetics, where harmony is created with the upper and lower lips, tooth position, size, and shape. These principles include golden proportion of maxillary anterior dentition, midline and arch alignment, axial inclination, incisal edge and lower–lip alignment, contact points of maxillary anterior dentition, arch form, graduation of teeth posteriorly, gingival symmetry, and gingival contour.
History
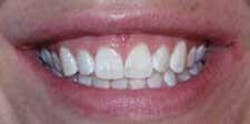
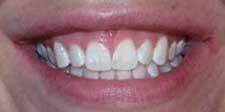
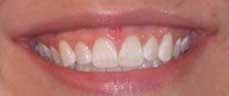
A 28–year–old female presented with the following concerns: she felt she had a gummy smile, and the soft–tissue height and contour did not complement her teeth. (see Fig. 1) She thought her teeth were too short and square and that the gum tissue appeared blunted and irregular. In addition, her maxillary frenum was very low and attached to the papilla between the central incisors.
Procedure
The objectives and goals for soft–tissue correction were presented to the patient. Periapical radiographs, periodontal charting, and models were used to develop the treatment plan. Radiographs showed excellent bone level, and pocket depths ranged between 3.0 mm to 3.5 mm. The width of the central incisors was 8 mm and the length was 8.5 mm. A marker was used on the soft tissue to simulate the amount of tissue reduction required to produce the length of teeth Nos. 6 through 11 in proportion to the width.
The golden proportion refers to the visual width of the maxillary anterior teeth. Measurements for the lateral incisors are divided into the measurements for centrals and cuspids. Ideally, the centrals relative to the laterals are 1.618, and to the cuspids, 0.618. The midline is the axis running down the center of the face.
The arch alignment should be perpendicular with the midline or parallel with the eyes. The axial inclination of the maxillary teeth has a vertical axis, which is inclined slightly to the mesial. The axis is a line drawn from the gingival apex to the center of the incisal edge.
In a natural smile, the incisal edges of the maxillary dentition should follow the contour of, but not contact, the lower lip. The interproximal contact points of the central incisors should be in close proximity to the incisal edge.
They gradually progress gingivally as they move posteriorly. The arch form of the maxillary teeth is determined by a line drawn between the tip of the canines — bisecting the incisive papilla. The graduation of the posterior teeth should be geometrically symmetrical. The teeth should appear shorter descending from canines to molars.
When the gingival tissue is exposed during a wide smile, the gingival height of corresponding teeth on each side should be symmetrical. This symmetry is critical as the midline is approached because the close proximity makes the factor obvious. The gingival apex of the lateral incisors is lower than that of the centrals and canines. This apex is 1 mm to 2 mm below a line drawn between the apex of the centrals and the canines.
The gingival zenith is the highest point of contour at the apex and should be just distal to the long axis of central and canines, but at the center for the laterals. Study model analysis showed the gingival zenith to be 0.75 mm to 1.5 mm, without violating the biological zone of attached tissue.
Emmela topical anesthetic was applied on the tissue from teeth Nos. 5 to 12, and lidocaine HCl 2% with epinephrine was administered with a 30–gauge needle.
The diode laser with 400 fiber was used for tissue reduction. The diode laser provides quick, very precise soft–tissue surgeries with minimal or no bleeding, swelling, or postoperative pain. Hemostasis is achieved and edema is prevented because capillaries and lymphatics are cauterized and sealed. In addition, tissue damage from the procedure is minimal.
Since tissue damage is related to the total energy delivered over time, the Touch Tips and fiber area are used in continuous, sweeping strokes and are kept moving during lasing. The 400 fiber was used with the diode laser on a setting of 1.8 watts continuous wave. The fiber was angled toward the incisal and the gingiva was contoured to the desired dimensions using a constantly moving stroke.
The maxillary frenum to be released was drawn tight by retracting the lip. The 400 fiber was used with the diode laser set at 1.8 watts continuous wave to make a releasing incision at the base where the frenum attaches to the maxilla. The muscle attachment was followed laterally and apically to minimize reattachment. The completed surgical area had the classic diamond shape. Since traditional scalpel incisions were not used, sutures were not needed.
Postoperative care directions given to the patient included doxycycline 100mg BID for one week, Dolobid (diflunisal) 500mg, and Oxygel (ozonated olive oil) to be applied to the affected area two times a day. A postop check was done the following day and the patient reported that she experienced "slight discomfort." On a scale of 1 to 10, the patient rated her pain as a "2." This lasted one day, during which she took Dolobid. For approximately one week following, she reported having to take only Tylenol as needed.
The gingival contouring healed in four to five days. The patient was very pleased with the results of the procedure and reported that one of her friends said, "It is beautiful! It looks like it has been airbrushed, like in a magazine. It is so perfect!" (see Fig. 2)
Office philosophy and methodology
It is the philosophy of our office to be patient–centered, and it is our mission to diagnose and treat periodontal disease, including gingivitis in its earliest form. The methodology to accomplish this is conservative, nonsurgical treatment, with active patient involvement.
Our periodontal evaluation form also becomes an educational tool for each patient. We record six–point pocket depths for each tooth, bleeding points, recession, furcations, mobility, tissue contour, tissue color, plaque scores, and calculus present. We explain to patients that this is the most efficient way to determine their progress and periodontal health at a glance.
We also point out to the patient all of the etiological factors that affect periodontal health and may compromise treatment. These include genetics, general systemic health, hormonal changes, diet, oral hygiene, occlusion, tobacco use, and stress.
It becomes evident to patients that they can develop a "barometer" to measure their periodontal health and susceptibility to disease. All of the data and variables are used as instruments to map the course of treatment. This "map" is developed with patients' input based on their own treatment goals. They become actively involved in their treatment recommendations.
Conservative treatment
Co–diagnosis and treatment–planning with the patient sets the stage for the next step — providing conservative treatment. This includes the number of therapy appointments to be scheduled, the sequence in scheduling, and the actual clinical modalities to be used. The ultimate goal of periodontal therapy (PT) is to stop disease progression and stabilize and improve tooth attachment. Treatment includes the use of hand instruments for scaling and root–planing.
We use microultrasonics for debridement and irrigation. Microultrasonics refers to power scalers that utilize acoustic energy. This allows mechanical vibrations to burst calculus or plaque deposits off tooth surfaces. Microultrasonic devices utilize thinner tips that are comparable to the thickness of a periodontal probe.
These tips give better access to deep, narrow pockets, as well as furcations. In addition, the fluid lavage of microultrasonics flushes bacteria and bacterial toxins, and the cavitational effect of the water from the rapidly moving ultrasonic tip breaks the cell walls of bacteria.
We use a diode laser to remove diseased epithelium and for bacterial decontamination. Local antimicrobials such as Atridox® are used when pocket depths are 5 mm or greater.
Finally, Periostat® is used at three–, six–, nine–, or 12–month intervals, depending on the patient's progress. This subantimicrobial dose of doxycycline (20 mg), used twice daily, is FDA–approved for enzyme suppression to manage periodontitis.
Regardless of the treatment modalities used, the purpose is to achieve a gradual healing process and continue treatment until the disease process is controlled. Cotherapy by the patient is critical. Our recommendations for this include daily use of power toothbrush, floss, and chlorine dioxide toothpaste and rinses such as CloSYS™. Follow–up after periodontal therapy is crucial.
Our system involves reevaluation after six weeks, and a second reevaluation after three months. Maintenance intervals of supportive periodontal therapy (SPT) are determined by the progress patients achieve. Our typical recommendation is a three–month cycle, but it can be as short as eight weeks.
Many benefits of the diode laser
The diode laser represents the latest advance in laser technology. It is a surgical instrument that is reliable, portable, and powerful. It provides quick, precise soft–tissue surgeries with minimal or no bleeding, swelling, or post–operative pain. It has a broad range of applications, which includes tissue retraction during restorative procedures, gingivectomy, gingivoplasty, crown–lengthening, frenectomy, bacterial decontamination, and removal of diseased epithelial lining during periodontal treatments. Its use enhances placement of contemporary materials and enables soft–tissue corrections both for restorations and natural dentition.
David P. Reichwage, DDS, maintains a private practice in Fort Wayne, Ind. He holds program certifications from the Las Vegas Institute for Advanced Dental Studies, Pacific Esthetic Continuum, the Academy of Laser Dentistry, JP Consultants Institute, Comprehensive Care Consulting, and Dr. James Carlson. Dr. Reichwage is a member of the Academy of Operative Dentistry, the Academy of Laser Dentistry, the American Dental Association, Indiana Dental Association, and the Isaac Knapp District Dental Society. He has served organized dentistry on state and local levels, and is a past president of the Isaac Knapp District.