Case Acceptance Begins and Ends With Trust
If there is a single, common core to all dental practice success - whether measured in treatment success, dollars, or personal fulfillment - it is case acceptance. The patient must accept our recommendations before any of the good things can happen that we bring about with our clinical skills and the latest materials and equipment. Having recognized this as a profession, we have spent countless hours and dollars in recent years on seminars, tapes, CDs, and books dealing with case acceptance. With all that, however, it appears to me that most of this information has missed or simply ignored the most basic point. This is not to say that all efforts have been wasted or useless. Our knowledge and ability to gain treatment acceptance have advanced steadily, and have revolutionized many struggling practices while benefiting millions of patients. But the very essence of what we are attempting to do when we approach a patient with a treatment plan has often been unclear or misunderstood. Boiling down the whole body of case acceptance knowledge to its most basic essence yields this: case acceptance begins and ends with trust - the patient’s trust in the dentist.
Intuitively you knew that already. Like many truths, it is both obvious and profound; so obvious that we may not have looked at it closely enough; so profound that it actually controls our relationship with the patient and the treatment he or she receives. The treatment that the patient accepts or rejects is the purest realization of their level of trust.
The centrality of patient trust in case acceptance was driven home to me by the contrasting behaviors of two patients.
The first of these patients - we’ll call him Roy - has been in the practice for many years. While good-natured, he receives most of our recommendations by saying, “I’ll have to think about it” (he’s been thinking for 18 years now). He routinely questions our fees, refuses treatment if it isn’t covered by insurance, doubts that replacing his missing molars would be of benefit to anyone but me (the dentist), and generally treats whatever we tell him with an air of skepticism. Recently, Roy developed an abscess in a lower bicuspid. When I offered to schedule him for the root canal, he told me he wanted to see a specialist. In spite of my assurances that I had done this procedure hundreds of times and that his was not a difficult tooth to treat, he made up his mind that he was going to the endodontist. The message couldn’t have been any more clear if he had just said, “I don’t trust you.”
The other patient, also in the practice for many years, has not only taken every recommendation we have ever made to her, but she has referred friends to whom she has told we can do no wrong. Her name is Elaine. More than once when discussing her options, she has said, “Do whatever you think is best. I trust you completely.” And she does. But not only that, she is also convinced that nobody else can do her dentistry as well. A while ago, a tooth I had restored with an inlay broke a cusp and needed a crown. By this time, she had moved up the coast, a three-and-a-half-hour drive away. To get to my office, she had to drive past hundreds of other dentists’ offices. She happily accepted my recommendation, never questioning whether I might be at fault for her broken tooth as a low-trust patient might have. Her level of trust prevented her from even entertaining such doubts.
In thinking about these two patients, I could not decipher specifically what caused one to trust so completely and the other never to trust enough to readily accept even a recommendation for basic care. But I realized there was a powerful lesson in the contrast between them. Trust, or the lack thereof, is the prime factor that explains both the high degree of joy and satisfaction there is in treating a patient like Elaine, and the frustration of treating a patient like Roy. Further, the tension we feel in treating Roy is based on a sobering reality. These are the patients who make our lives miserable, who complain and question, who break appointments, who create collection problems, and worst, who may even sue us the moment something unplanned happens.
So, for me, the quest for case acceptance became the quest to build trust. This is the key point I hope to make: we need to shift our focus away from gaining acceptance of treatment plans and toward gaining the patient’s trust. And more importantly perhaps, we must seek to build that trust ultimately for the good of the patient, not for our own gain, because working a trust-building system only for personal gain is inherently untrustworthy. As King Solomon said, “Better to be poor and honest [trustworthy] than a rich person no one can trust.”
How can we reliably gain and maintain our patients’ trust when they enter our practice? The generic answer to this question is that we must be trustworthy and communicate it to the patient in our actions even more than our words. Trustworthiness comes from who we are, our character, and the behaviors that express the qualities comprising our character.
We must exhibit trustworthiness to such a high degree that it will overcome the inherent conflict of interest there is in being a private practice health-care professional. The conflict arises from the fact that the person who diagnoses and describes the problem is the same person who decides on the solution, sets the fee, performs the service, and profits from doing it. At some level, our patients are aware of this conflict of interest, and so will resist taking our recommendations for treatment until they feel comfortable with the knowledge that we have placed their interests ahead of our own. Patients look for clues regarding our trustworthiness.
Following are some of the components of trustworthiness as they relate to the new patient and case acceptance. These form some of the clues our patients are hoping to find.
1) Competence - Strive to continually improve your skills while making sure that the treatment you propose is within your competence. Don’t promise what you can’t deliver with excellence. A corollary is that you present the best treatment for the patient even if you can’t deliver it yourself, in which case you make the appropriate referral.
2) Consistency, integrity - Everyone on your team tells the patient the same thing - not because they memorize what you tell them to say, but because you and your team all share the same beliefs about what you do. Judge your own work by the same standard you use to judge the work of the patient’s previous dentist, which means if it needs to be redone, you will recommend that to the patient whether you or someone else did the failing work.
3) Listen before you talk - Ask before you tell. Offer a solution only after you have listened and fully understand the problem. The solutions (treatment) you offer are tentative until patients have a chance to decide if it is right for them.
4) Open and honest communication - Give your patients all the options - both pros and cons (no hype) - and then trust them to decide. People have a newly heightened desire for genuine communication. Most people now know that even with all the advances in dental care, there is also a potential downside. They don’t want that hidden or glossed over.
5) Be trusting - Trust begets trust. Inform the patient, ask for a decision, and listen closely. Don’t “hard-sell” if they choose differently than you hoped. Your trust in your patients to make the right choice for themselves, even if it is not the choice you would make, will be rewarded by a greater likelihood that they will trust you.
6) Keep your word - Under-promise and over-deliver. Don’t set yourself up to break your word by promising more than you can deliver. It is better to disappoint your patient before treatment about how long the implant will take than after the implant is placed and they discover they are trapped in a six-month wait.
7) Keep confidences; do not gossip - Don’t let patients hear you discussing another patient by name (even in ways not prohibited by HIPAA). They might fear you’ll discuss them in the presence of others.
Once trustworthiness infuses the atmosphere in your office, look at your systems from the perspective of trust-building. While you may be personally trustworthy, your systems may work against you to erode trust. One key principle in designing systems that build trust is to remember that a patient’s trust grows gradually. Certain steps in the process from the initial phone call to actual treatment require greater levels of trust than others. Those steps that require greater trust need to be held off until the patient’s trust level is sufficient.
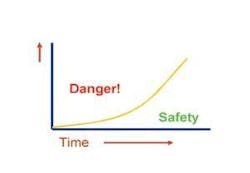
A useful tool in conceptualizing this abstraction is what I call the trust curve. The trust curve is a simple graph depicting the change in a patient’s trust level over time (Figure 1).
The danger zone depicted here represents the higher level of trust that the patient hasn’t reached yet. It is dangerous to expect patients to do something, such as accept complex treatment, before they have built sufficient trust. However, as time goes on, if you are successful in communicating trustworthiness, the patient’s level of trust rises to allow them to accept that same treatment. Staying in the safe zone of the patient’s current trust level is what I call “staying inside the trust curve.”
Applying the concept of the trust curve to the critical system by which we bring new patients into the practice will help determine the schedule of the first office visit. I have written previously (“Challenging Dentistry’s Dogmas,” March 2000 Dental Economics®) about the advantages of not insisting that new patients agree to a comprehensive exam and case presentation on their first visit. This is one of the more pointed examples of how using the trust curve principle can dramatically change a system we have clung to for years. First, attempting on the very first contact to persuade new patients that what they want (a “cleaning”) is the wrong choice requires a verbal maneuver that, even if executed skillfully, threatens to start the relationship with a trust-eroding confrontation.
Second, no matter how up-to-date your office and equipment are, no matter how many diplomas and certificates decorate your walls, no matter how beautifully attired your team is, the first time a new patient meets you is not the time to present treatment that may be far more complex and expensive than he or she anticipated. The trust curve principle suggests that the exam and case presentation be held until the patient has been in the office at least once before to start building trust.
An initial visit for a prophy, X-rays, or even a simple meet-and-greet will give you an opportunity to demonstrate trustworthiness and start to gain that patient’s trust.
Another area where the trust curve principle may influence your systems is in deciding when to discuss your policies. Be very careful with policies. Personally, I bristle when I hear the phrase “our policy is…,” and I think many of our patients feel the same. A policy is nearly always something that benefits the practice at the expense of the patient (payment policy, cancellation policy, insurance policy, etc.). While these may be necessary to a degree, how and when you communicate them is critically important in building trust. In general, policies should not be a part of the initial phone conversation. In my opinion, the earliest time to broach the subject is at the end of the first visit, and preferably later after the patient has committed to a course of treatment.
One last area where the trust curve principle may cause a shift in our thinking is regarding the referral source of a new patient. We know that a patient referred by a satisfied patient has always been considered the “best” kind of new patient. Practice-management experts mostly agree that the goal is to have as many of our new patients as possible come from direct patient referrals. I don’t disagree that referred patients are usually more receptive to our recommendations and less likely to question what we do. This is because the referred patient who has been told good things about your practice enters with a higher level of trust. In other words, they start off higher on the trust curve. But that does not make a Yellow Pages-referred patient a “junk patient” as so many practitioners have concluded. It only means that you must respect and make allowances for their need to build trust from a lower starting point. If your systems allow for that, you will find that all new patients are just people seeking care, no matter how they heard about your practice. How you treat them once they call you is far more important in determining their receptiveness than the referral source. If your advertising represents your practice accurately and you meet people where they are on their trust curve, you will find that there is ultimately no difference between a referred patient and a media-generated patient once they have had a chance to find the clues to your trustworthiness.
For any practitioner who strives to achieve greater success in delivering comprehensive care that fits the patient’s true needs and desires, a shift in the goal from case acceptance to patient trust is the foundation. There is no case acceptance without trust. By intentionally becoming trustworthy, and by creating a practice culture based on trust-building principles to increase our ability to meet the real needs of patients, we will realize the fulfillment of our purpose as dental professionals.
Ted Morgan, DDS, maintains a private practice of general, restorative, and cosmetic dentistry in Gorham, Maine. Since 1996, he has presented and created seminars teaching success skills, leadership, and case acceptance. Currently, at Dental Boot Kamp, he teaches dental teams how to communicate effectively with patients, build trust, and reach mutual agreement on treatment decisions. Dr. Morgan can be reached at (207) 839-2655 or [email protected].