Increase production and decrease expenses in sterilization
by Mark Tholen, DDS, MBA
For more on this topic, go to www.dentaleconomics.com and search using the following key words: sterilization, profitability, practice expenses, practice production, equipment.
Our thoughts do not naturally turn to the sterilization area when we consider methods of increasing production in the dental office. But many times production is a euphemism for profitability, and there are many opportunities to improve practice profits in the average sterilization area — 10 to be exact.
Let's start with the big picture.
Labor is the single largest expense in the practice's annual operating budget; it usually consumes about 25% of the practice's annual budget. The sterilization area is the most labor–intensive area of the office as the average dental assistant enters this area more than 80 times each day. This represents significant cost to the practice.
Many practices avoid cleaning and sterilization equipment purchases (which will pay for themselves within a year in labor savings) because they mistakenly believe they are saving money. They spend money on labor instead of equipment, month after month, year after year. It is an insidious expense to which we become accustomed and accept, whereas the extraordinary capital expense always demands our attention and distracts us from the real financial opportunity of reducing labor cost.
Idea 1: Stop handling individual instruments
From the moment the procedure ends in the operatory, significant labor savings can be achieved by minimizing the repetitive handling of instruments as they are processed through sterilization. How is this done?
Cassettes achieve significant labor savings for the practice. A careful analysis of the potential time savings revealed that more than one hour of labor can be saved for every nine procedural set–ups processed when using cassettes. Hand scrubbing instruments, disinfecting trays, sorting instrumentation, and tray assembly are all eliminated from the sterilization cycle, thereby accelerating the flow of instrumentation through the cycle. In a week, this translates into a noticeable savings that falls to the bottom line of the income statement; i.e., net profit.
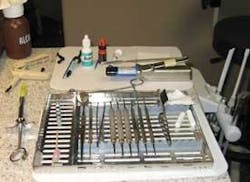
A high–quality set of cassettes, such as the Hu–Friedy Instrument Management System™ stainless steel cassettes, equipping a five–operatory office including instruments, will cost approximately $8,000 (Fig. 1). Amortized over the life of the practice, this expenditure does not amount to daily pocket change, and the return is yielded daily in significant labor savings.
Idea 2: Stop hand washing and drying instruments
Decontaminating, washing, rinsing, and drying instruments are extremely labor intensive and dramatically reduce the throughput speed of instrumentation through sterilization. Even the use of an ultrasonic cleaner does not materially enhance instrument processing speed or reduce labor. How do you combine all of these tasks to reduce labor cost?
A dedicated instrument washer specifically designed to debride, wash, rinse, and dry instruments is the single greatest labor–saving device in the office. Used in combination with cassettes, approximately one hour of labor can be saved for every nine procedural set–ups that are processed through sterilization.
Between cassettes and an instrument washer, a minimum of 10 labor hours can be saved each week, or 40 hours each month. A savings of one employee week in labor each month is significant!
A quality instrument washer can easily handle the instrument throughput needs of a four– to six–operatory office, and costs approximately $8,500 (Fig. 2). Again, amortized over eight years, the return on the investment in labor savings is staggering.
Idea 3: Match the instrument cleaning and sterilization capability
Practices often make the mistake of increasing the instrument cleaning capability in the cleaning workstation area with an instrument washer, but not improving the instrument sterilization capacity ... or vice versa. In order to accelerate instrument throughput and dramatically reduce labor costs, it is important to match the processing capability of the cleaning device(s) with that of the sterilizer(s). As a general rule, it is a good practice to have a standard autoclave with a chamber size of at least an 11–inch diameter and a flash sterilizer. Larger practices may need multiple autoclaves and larger flash sterilization capability.
Idea 4: Instrument flow and efficiencies are optimized with proper workstation sequence
Used instruments should enter a designated contaminated area in central sterilization, move to a clean area after they have been washed/dried, packaged and sterilized, and finally transported to a designated sterile instrument storage area. The u–shaped central sterilization area demonstrates this instrument flow most graphically (Fig. 3). Orderly instrument flow can work in a clockwise or counterclockwise direction; direction of instrument flow is determined with the location of the sink and recessed ultrasonic cleaner.
In order to maximize production, minimize staff stress, and increase scheduling flexibility, four important principles of medical and dental office design must be observed that will directly impact the efficiency and throughput in central sterilization:
- All operatories should be identically equipped.
- All instrumentation should be stored in central sterilization.
- Instrumentation should be organized into procedural set–ups (cassettes) to optimize flow and efficiency.
- Instrumentation is brought from central sterilization to the operator; the operatory function is defined by the instrumentation.
Idea 5: Being tubby is a good thing ... in sterilization
Of course, procedure tubs provide an efficient method of storing and using individual procedure consumables. These portable operatory drawers allow staff to store and transport consumable materials by procedure type (Fig. 4). The tubs can be color–coded to match the designated sterilization cassette rails when they are used in conjunction with cassettes, and the labor savings is compounded. This idea, along with the tub and cassette(s), provides for the implementation of the four principles described above.
Idea 6: All upper cabinets in sterilization cabinetry should have translucent (smoked) glass doors
Due to the heavy traffic in this area, a “doorless” central sterilization area is recommended. With doorless sterilization areas, patients are likely to view the area on their travel to or from treatment. To portray a clean and orderly office, place dark (smoked) glass on the upper cabinet doors so that soiled/used trays or cassettes can be placed in the cabinets. The patients will see only an orderly sterilization center and the assistants will be able to determine whether soiled cassettes/trays need attention by looking directly into the dark glass of the cabinets.
Idea 7: Avoid the ‘dental two–step' in sterilization
Regardless of the shape of the office's (anticipated or planned) sterilization area, there should be a four–foot–wide aisle in sterilization that allows two people to pass each other without turning to avoid collision. Dental offices typically attempt to save space by skimping on hallway space, but the sterilization area is the most trafficked area of the office, and adequate space for personnel movement maximizes efficiency. Create aisles that accommodate the staff traffic in the office.
Idea 8: The sterilization area sink needs two faucets/ water sources
A sink should be large enough (24 inches wide and 9 inches deep) for two assistants to use simultaneously. The sink should also have two, 12–inch curved faucets or two water sources for the assistants to work side by side. It is not efficient to have staff members in line waiting to use a $150 sink. An additional faucet costs approximately $80 (during construction), and the average office life is 17 years ... you do the math. Labor is minimized in sterilization when there is adequate equipment to support the staff.
Idea 9: Let there be light ... under the countertops
Adequate lighting brightens the staff's mood and increases efficiency. Lighting of the cabinetry counter space and the entire sterilization area can be accomplished with task lighting under the upper cabinets and recessed ceiling lighting using parabolic lenses. Ideally, 150 to 200 foot candles of light should be provided on countertop surfaces for effective, but not irritating, illumination of workstations.
Idea 10: Sterilization area entrance should not be more than 30 feet from the most distant operatory
The sterilization area should be centrally located in relation to the operatories. Ideally, every operatory opening should be within 30 feet of the sterilization area ingress/egress to maximize staff flow, efficiency, and operatory turnover. In large practices where this dimensional principle cannot be employed, the use of satellite sterilization areas should be considered.
There you have it: 10 ideas that can save labor and expense, dropping money to the bottom line of the practice's income statement. Perhaps you can use one idea or all 10 tomorrow, but each concept has been tried and tested in thousands of practices across the country for the past 30 years. They are not just ideas, but principles that have increased the productivity and reduced the physical stress of tens of thousands of dental staff.
Mark Tholen, DDS, MBA, is the former CEO of T.H.E. Design, which designed more than 3,000 dental offices. He is also the author of “A Guide to Designing the Elegant Dental or Medical Office ... The Largest Marketing Tool of Your Career,” available at Amazon.com. Dr. Tholen can be contacted at [email protected].