Interaction between GPs and specialists
Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Q I've been practicing as a general practitioner for over 20 years. I've achieved Fellowship and Mastership status in the Academy of General Dentistry, and I accomplish at least some procedures in all areas of dentistry on a routine basis. Recently, some of the very competent general dentists in our community have received significant criticism from a few specialists for including some of the procedures in their practices that are also accomplished by specialists. What is your opinion relative to these frustrating situations that confuse the public and make our profession appear to be fighting within itself?
A You have asked a question on a topic that is of great frustration to me also, and I'll be pleased to provide my opinions on the subject. Please keep in mind that I'm a practicing board certified prosthodontist who accomplishes research in all areas of dentistry, and I also observe dentistry throughout the world.
If asked how I personally would compartmentalize dentistry into various areas, I would identify overall dentistry itself as the largest specialty in medicine, and I would classify the now ADA-recognized specialties of dentistry as subspecialties of the major specialty, dentistry. Just as in most medical specialties, a dentist would have to show competency in the parent specialty, "dentistry," before being allowed to subspecialize in the other seven areas. Examples are subspecialties in surgery. Plastic surgeons and others must become competent and qualify as general surgeons before subspecializing in plastic surgery.
It has been my observation that some dental specialists elect to become further educated in a current dental specialty without having achieved competency or knowledge in overall dentistry. Unfortunately, the result is a lack of overall dental knowledge that is clearly observable as a characteristic of some specialists.
What is the result of this situation? I could describe numerous examples in which specialists and/or general dentists could have communicated more thoroughly before a specific treatment plan was initiated. I'll use a recent clinical example that I encountered and have subsequently treated.
I'm not critical of the specialist who previously treated this patient. He tried his best to satisfy the patient's challenging needs within the realm of his specialty knowledge. However, this clinical example will show the desirability for specialists to have broader clinical knowledge and be able to provide complete descriptions of ALL of the clinical possibilities before accomplishing treatment. The patient should be heavily involved with the final decision about treatment after hearing all of the advantages and disadvantages of each. In other words, thorough informed consent should be accomplished before beginning any treatment.
In the case of the following patient, unpredictable complications could also have led to failed treatment. However, it is an excellent example of a situation for which several treatment plans could have been discussed with the patient.
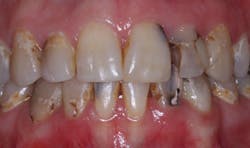
I was told that before any of the current surgery, the patient had very minimal bone in the edentulous maxillary arch. Before I saw the patient, one of the treatment plan options was to provide bone grafting on the maxillary arch, place implants in the grafted sites, and provide an overdenture or fixed prosthesis supported and retained by the implants. A surgical specialist accomplished the surgical procedures. Unfortunately for both the dentist and the patient, the grafts and implants did not stabilize, and the patient was left in worse condition than before the surgery (Fig. 1). Grafting and further placement of implants then became an unacceptable option for either the specialist or patient.
The patient's mandibular arch had several missing posterior teeth, inadequate bone for implants, and several remaining adequately stable anterior teeth. The specialist's plan was to provide bone grafting for the posterior mandibular arch, place implants, and eventually have another dentist seat fixed prostheses on the implants. The surgical specialist accomplished the grafting. However, after it healed, and on my first observation of the patient, the bone density and quantity in the posterior mandibular area was still questionable, as shown by the low Hounsfield unit designations of about 200 on the cone beam radiographs (Fig. 2).
This frustrating dilemma could have happened to any of us. Additionally, the patient could have had numerous systemic conditions that negatively influenced the lack of success of the treatment. The fact remained that when I first saw this patient, she still had to receive some form of oral treatment that would allow her to have adequate oral function and esthetics.
What additional options were available for this patient before the failure of the surgical treatment? A few nonprioritized plans are:
- Option 1: Placement of two conventional diameter implants (3 mm or more in diameter) in the maxillary canine areas in the bone present in the canine eminence area. After adequate implant integration, placement of a maxillary overdenture supported and retained by the two conventional diameter implants.
- Option 2: In the event of minimal bone, placement of four or more small diameter implants (1.8 mm to 2.9 mm in diameter) in the premaxillary area, either immediately loading the small diameter implants, or if the bone was somewhat questionable, waiting for a few weeks of healing before making a maxillary overdenture.
- Option 3: Placement of a flange denture without use of implants, which is currently not well known by either dentists or laboratory technicians. These dentures do not have conventional border molding. The borders extend far into the cheek area nearly to the teeth. Pictures of this technique are shown in this article.
What alternative techniques could have been accomplished on the lower arch in addition to grafting and placement of conventional diameter implants? At least two viable plans were present, the two options below:
- Placement of fixed prostheses abutted to at least two natural teeth on each side, with cantilever extensions to the posterior to simulate first molar occlusion.
- A distal bilateral extension removable partial denture.Implants did not appear to be a viable treatment option due to the minimal density of bone as shown on the radiograph and discussed above.
It is logical to assume that a surgical specialist has adequate knowledge and experience in the prosthodontic procedures to predict the best procedure for the patient. In any clinical situation, if the specialist does not feel adequately prepared to provide complete informed consent and patient education, the patient should be referred to someone competent in prosthodontics (GP or prosthodontist) before a final treatment plan is developed. The likelihood of success or failure should be thoroughly discussed with a patient before accomplishing any procedure.
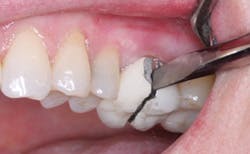
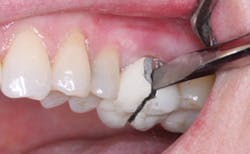
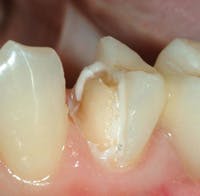
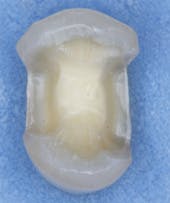
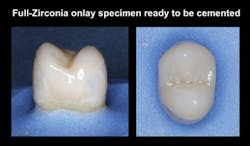
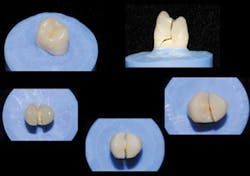
The surgical dentist who had the unfortunate failures I described referred the patient to me. After consultation with the surgical specialist, long consideration of the alternatives, and discussion with the patient, a treatment plan was agreed upon. Because of the lack of bone and the undesirability of further bone grafting, we were pleased to provide the patient with a flange maxillary denture (Figs. 3-6) and two mandibular cantilever fixed partial dentures as shown in Fig. 7.
My answer to your original question can be summed up like this. After being a practicing dentist/prosthodontist for several decades, very few concepts or techniques that I learned in dental school are still viable. My graduate programs are similarly out-of-date. Where did I receive the education and experience to accomplish the preventive and treatment procedures that I now use? You guessed it -- two types of education have allowed me the continue to practice on a state-of-the-art level, and those are hundreds of hours of continuing education as the profession has continued to evolve, and personal observation obtained in the "school of hard knocks," including thousands of hours observing preventive and treatment procedures in my own and others' practices.
Dentists, or people in any other vocation, gain their expertise through their original education, subsequent continuing education, constant observation of valid research, and clinical observation and experience. After years of practice, the original rudimentary knowledge obtained in predoctoral dental school or any graduate programs fade into history. As that occurs, the practitioner is responsible to stay up-to-date.
I will be criticized by some specialists for the following statement. Dentists who have made the effort to obtain adequate continuing education and achieve clinical competency in the area of dentistry they choose deserve to accomplish the procedures in those areas of dentistry. Regardless of the location or date of their initial dental degree, the postgraduate or graduate education they have taken, or the certificates they have gained, they should be able to treat patients in most areas of dentistry in which they have been educated.
Conclusion and answer to the question.
The bottom line to which I strongly adhere is, "Don't do anything to a patient that you would not do to yourself." If you or others feel competent to accomplish a procedure and you can do it to the level of a specialist, do not hesitate to incorporate that procedure into your practice. A pertinent question then arises -- why are there specialists? Many dentists do not want to take the time or spend the money to obtain adequate continuing education to increase their expertise, and these dentists prefer to refer patients who need specialty care to specialists.
Practical Clinical Courses provides CE that relates directly to your question:
One-hour DVDs
- Making Complete Dentures a "Win-Win" Service (Dentures using implants for retention and support) Item #V2549
- Placing Mini Implants Simple, Safe, and Effective Item #V2360
Two-day AGD mastership level courses in Utah:
- Practical, Real World Dentistry - Fixed Prosthodontics
- Simplified Implant Surgery
- Mini Implants, Easy Placement and Immediate Restoration
Visit our website www.pcccdental.com or call (800) 223-6569 for further information.
Gordon Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Dr. Rella Christensen) and CEO of CLINICIANS REPORT (formerly Clinical Research Associates).
Past DE Issues