Calming and educating fearful, anxious patients
Q: Often, when we've explained to our patients the treatment we've done for them and what we expect them to do following the procedure, we find that they did not accomplish the tasks we asked them to do. This occasionally results in poor healing, pain, loose sutures, dry sockets, swelling, inflammation, or outright failure of the treatment. What do you find to be the best ways to ensure that patients understand the treatment that has been done for them and their expected responsibilities after treatment has been completed?
A: Your question is a common problem in most practices. If patients do not remember the postoperative instructions you've provided for them, they do not accomplish what you've instructed them to do.
It is a well-known fact that fear, stress, pain, anxiety, or frustration causes a significant change in human concentration and memory (figure 1). People can't remember well when they are in such situations. They cannot concentrate during those times, and they often have poor judgment. They worry and see only the negative in a situation, and they have anxious or racing thoughts. Remember those times in your life, and you'll accept these statements.
Fear, stress, pain, anxiety, and frustration are present in even the most atraumatic oral treatment procedures. Add helplessness to those feelings and you've described many dental appointments.
It's no wonder that people do not accomplish what you've asked them to do if they can't remember the instructions you gave them. Are there ways to reduce this problem? Can patients be instructed more adequately and thoroughly? My answer is YES! Let's look at some well-proven methods for improvement in postoperative patient behavior.
Use the diagnostic appointment for instruction about the procedure
At a typical diagnostic appointment, patients are just getting to know you. On this initial appointment, they are not fearful; they are only apprehensive and uncertain about you. This is a highly appropriate time to educate patients.
You have undoubtedly heard me talk about having dental staff - assistants, hygienists, and front desk persons - educate patients. It is well-known that patients accept staff, especially female staff members, better than they accept the doctor. Patients will listen well to staff (figure 2). However, staff persons must be educated! I suggest that you have staff education sessions on a routine basis to educate your team to a knowledge level at which they can educate patients.
A good time for these sessions is an hour before starting practice at least once a month. Providing education during the diagnostic appointment is one of the best ways to educate patients. However, they often forget what you tell them. Remember that there is usually significant time between the diagnostic appointment and the treatment appointment where questions can be answered if patients have any concerns about their treatment before it begins.
Send information home with patients
During the diagnostic appointment, patients have usually committed themselves to the treatment or preventive procedures. Could there be a better time to provide them with written information to take home about the treatment they've elected (Fig. 3). You may compose this information yourself, obtain pamphlets from the American Dental Association, or use some of our patient education information sheets from Dr. Christensen's Dental Documents (described later).
Assume they've accepted a treatment plan that includes implants. Do they know about implants? Very few have any knowledge about dental implants. Give them some printed information to take home. Family members or friends can also see and comment on the proposed treatment. More importantly, patients can review the information and better understand the planned treatment or prevention. When patients come in for the first clinical appointment, the apprehension they have is significantly reduced because they're prepared for what's going to happen.
Review proposed treatment with patients before starting
By the time patients are in for treatment, they've forgotten much of what you told them during the diagnostic appointment. It's important to take a few minutes to review what you're going to do before starting (Fig. 4). In a very busy practice, you may have the dental assistant review the procedure while the local anesthetic is working.
Patient education during treatment
During the actual treatment, most patients have some fear of the unknown, in spite of education by you and your staff. Is this a good time for additional education? Yes and no. Some patients do not want to know exactly what you're doing, while others want to know every step in the procedure. You can easily determine the educational desire of a patient, and I suggest that you respond accordingly.
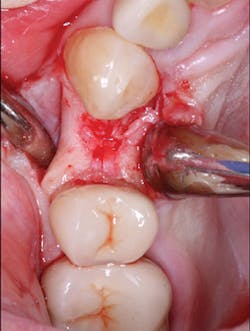
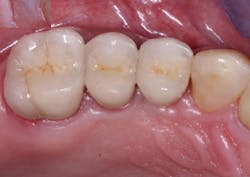
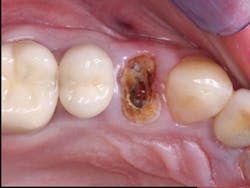
Every procedure is slightly different. If you can briefly draw an understandable and simple picture of someone's exact clinical need, they will understand it better and be calmed. If you can't draw, use illustrations by someone else. I suggest you make photographs of clinical procedures and store them in your clinical computer. Show patients before-and-after photos at the beginning of the procedure and at the diagnostic appointment (figure 5). I do not suggest showing blood or any potentially anxiety-producing procedure (Fig. 6). Just show before-and-after photos. This greatly assures patients that you're capable and know what you're doing, and they become more relaxed.
Tactfully talking to patients during a procedure is usually reassuring. Stating from time to time how well the procedure is going makes them feel good about what you're doing.
Don't expect patients to remember Instructions during or immediately after the procedure
As stated before, the likelihood of the patient remembering your instructions during treatment is minimal. However, it calms patients when they feel everything is going well. On a complex procedure, if possible, have a friend or family member with them who will remember more than the fearful patient will.
Instruction after treatment is completed
In my opinion, this is one of the most important times for providing information to patients, but it must be tangible information to take home, not just verbal. When patients leave the office, they are mentally relieved, the anesthetic is wearing off, and they're returning to normal life. When they get home and become comfortable, most patients will look at the information you provided them.
I'm sure many of you have been to a health practitioner who did not provide written information after a procedure. When you got home, could you remember the instructions you were given? I doubt it. What type of postoperative informational material is best?
Postoperative telephone contact
It is a well-known fact that a postoperative telephone call from the dentist or staff is one of the most important public relations acts you can perform. The person calling can answer questions patients may have and reassure them that the postoperative progress is going along as planned. I suggest that this call should be on the day following the procedure, not on the day of the procedure, to allow the often traumatized tissues to slightly recover.
Summary
Patients don't remember anything in a fear environment. As a result, many do not know what to do when they get home. There are numerous ways to reduce or eliminate this problem. Educate patients in a non-fear environment, and you will have significantly better compliance to proper postoperative care.
MORE FROM DR. CHRISTENSEN
The importance of making and retaining diagnostic casts
Conservative, affordable, implant-supported overdentures
Preventing postoperative tooth sensitivity
Gordon J. Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Dr. Rella Christensen) and CEO of Clinicians Report (formerly Clinical Research Associates).
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.