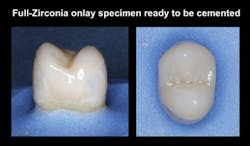
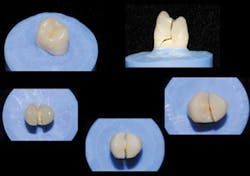
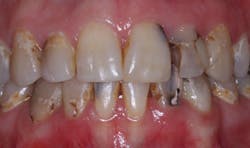
What Makes Small Diameter Implants Fail?
By Gordon J. Christensen, DDS, MSD, PhD
Q I understand that small diameter implants (minis) are being used for patients with various conditions or situations that do not allow placement of conventional diameter implants. Why can't conventional diameter implants be placed in some patients, and what conditions must be present to expect clinical success with small diameter implants?
A Thanks for asking the questions. They are very important questions that make some dentists reluctant to use small diameter implants (SDIs). First, let's define a small diameter implant. Root-form implants ranging in diameter from 1.8 mm to 2.9 mm are considered to be SDIs. Implants 3.0 mm and over in diameter are considered to be conventional diameter implants. These definitions are related primarily to when each category was cleared for use by the FDA, which was 1997 for SDIs and 1976 for conventional diameter implants.
There are numerous reasons why SDIs are necessary for treatment of some patients.
Bone availability -- For placement of a conventional diameter root form implant, most would agree that without bone grafting, 6 mm of bone in a facial-lingual direction and 10 mm in a crestal-apical direction are minimally adequate. Of course, there are exceptions to these measurements. Many patients do not have this much bone.
Potential reasons for use of SDIs -- In my opinion and experience, the following are major reasons for placement of SDIs:
- Inadequate bone quantity and no interest in or desire for bone grafting.
- Inadequate bone quantity and lack of financial resources for grafting.
- Inadequate bone and too physically debilitated for grafting.
- Adequate bone but too physically debilitated for conventional implant placement, which is usually more aggressive than placement of SDIs.
- The patient wants the most minimally invasive procedure, and SDIs fit that requirement.
I have asked questions in many continuing education groups to determine the frequency of major bone grafting procedures as reported by general dentists. A typical question that I ask is, "Who has accomplished or referred a patient for a major bone graft, such as a chin graft or an iliac crest graft during the last year?"
In typical groups of 200 to 300 participants, I usually have one or two dentists say that they have accomplished a graft or referred someone for a major graft in the last year. I conclude that the use of major bone grafting procedures in the profession is very low.
Assuming that grafting is usually not an alternative chosen by the patient, what options does the patient have? There are a few:
- Do nothing and suffer with whatever oral condition is present. In the past, this was the course of action most often elected by the patient.
- Assuming the crestal-apical bone tapers to a knife edge on the crest and there is significant bone height crestal-apical, have the crestal bone removed to the level where at least 6 mm of bone is remaining in a facial-lingual direction. Implants are then placed, and a fixed or removable appliance placed to restore the teeth. The surgery, implant placement, and prostheses required with this now popular procedure (All-on-4®) are successful, but well beyond the financial capability of most patients.
- Place SDIs and an overdenture, which has minimal expense, only slight discomfort, and high success. (Figs. 1-4)
After successfully placing SDIs for such patients since 1997, I am convinced that SDI placement followed by placement of a well-made overdenture is a financially feasible, highly successful, and much appreciated solution for these unfortunate patients.
Conditions that must be present for success with small-diameter implants
In my opinion, the following conditions are necessary for success with SDIs. I have had a few failures during the years of placing SDIs. In each failing case, I have violated one or more of the following points. Assuming all of the following conditions are positive, I see no reason for failure of the SDIs during service. Please observe the several photos in this article that demonstrate some of the most positive and negative important points.
- Bone quantity -- At least 4 mm of bone in a facial-lingual direction and preferably 13 mm of bone in a crestal-apical direction provide relatively acceptable conditions. However, success can be achieved with as little bone as 3 mm and 10 mm respectively.
- Bone quality -- When screwing the SDI into place, at least 30 Ncm of resistance should be present. If that level of resistance is not present, implant failure is likely. Refer to Fig. 5 and note that the bone on both the maxillary and mandibular arches is not dense. This patient did not receive implants on the maxillary arch, but he had SDIs placed on the mandibular arch that have served for many years. As you know, the maxillary bone is usually not as dense as mandibular bone.
- Width of implant -- The diameter of the SDI should be as wide as the bone that is present will allow. Use of the smallest diameter SDI (1.8 mm) is not advisable if wider implants can be used.
- Length of implant -- The average most used length for SDIs is 13 mm as reported by companies selling SDIs. Observational data confirms the success of this length, although shorter SDIs can be used with caution.
- Occlusion -- Bruxers, either grinding or clenching, are not good candidates for SDIs. If SDIs are used on these patients, flexible attachments such as rubber "O" ring attachments should be used to provide resilience.
- Soft-tissue (Fig. 6) -- Soft tissue more than 2 mm thick coronal to the bone should be removed to reduce excess stress on the SDIs.
- Parallelism (Fig. 7) -- Place SDIs parallel to one another! More than 15 degrees of non-parallelism can be negative.
- Separation of implants -- Do not place implants too close together. Leave space for the housings or attachments, which are at least 4 mm in diameter.
- Immediate loading of implant -- If the bone quality is questionable, place soft denture reline material in an indentation inside the denture over the implants and allow the implants to integrate into the bone for a few months before loading. However, most SDIs used for support and retention of complete dentures can be loaded the day they are placed.
If these nine requirements are observed and accomplished, there remain only a few obscure and infrequent reasons for SDI failure.
I hope I have answered your questions. Grafting is either not possible or too expensive for many patients. Small diameter implants are an excellent alternative. However, they must be placed and restored properly. Observance of the suggestions I have made will ensure clinical success.
Gordon Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Dr. Rella Christensen) and CEO of CLINICIANS REPORT (formerly Clinical Research Associates).
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Additional Resources
PRACTICAL CLINICAL COURSES has many professionally made videos on implants available. Our recent video on SDIs shows Dr. Christensen placing four mandibular SDIs in a typical patient who has minimal bone. The close-up, live, one-hour video demonstration makes placement relatively simple for those observing the video.
It is item V2360, Placing Mini Implants -- Simple, Safe, and Effective. A companion video that will help your staff is item V2342, Integrating Staff for Mini Implant Success.
For information, call (800) 223-6569 or visit www.pccdental.com.
Past DE Issues