Zen and the art of periodontal maintenance: Principles in productive hygiene
Brad Guyton, DDS, MPH, MBA
Jan LeBeau, RDH, BS
In the book Zen and the Art of Motorcycle Maintenance, author Robert Pirsig writes about a 17-day motorcycle journey from the Midwest to the West Coast. He notes that the “ . . . engine idle is loping a little,” which indicates the wrong mix of fuel and air.1 He rectifies the problem and takes off with the bike performing well again. When the author passed away this spring, we looked back at his work, and the parallels to dental practice became evident. Often, our engine idles start to lope a little when the mix in our practices is off. Often this happens when we don’t pay close attention to the hygiene department.
It is well known that a strong hygiene department drives a strong restorative practice. The idea that dental hygiene serves as a loss leader is old-school thinking. In fact, as a percentage of production, hygiene services can often be one of the most profitable procedures for the dental practice. Much like with a motorcycle, practice owners must consider three steps for getting the most out of their practices and rectifying any problems:
- Understand industry benchmarks. (This will serve as your owner’s manual.)
- Recognize the limitations. (Don’t push a bike or vehicle past its redline.)
- Promote the principles for a productive hygiene department. (Follow the rules of the road and the bike to get the most out of the ride.)
Understand industry benchmarks
According to the Centers for Disease Control and Prevention (CDC), 47.2% of people over 30 years of age and 70.1% of people over 65 years of age have periodontitis,2 yet only a fraction of these individuals actually receive the necessary treatment to appropriately manage this chronic infection. Even more alarming is the connection between periodontitis and compromised whole-body health. This presents a tremendous opportunity to diagnose existing periodontal disease earlier in the continuum of care and provide patients with the treatment they need to achieve long-term oral health and overall health.
It typically takes 800 to 1,000 active patients to support one full-time hygienist. Each dental hygienist should be producing approximately three times his or her wage in production.
As a rule of thumb, aim for the hygiene department to contribute 30% of the practice’s gross production. If the hygiene production is over 40%, the practice is likely too dependent on existing patients whose restorative needs have been met. Furthermore, if dental hygiene production is less than 20% of practice revenue, one of two things can be happening: the hygiene department is only doing prophylaxis services and not diagnosing the periodontal disease that exists in the practice, or the office may be a niche practice that does a lot of high-dollar complex cases.
A well-run hygiene department should be identifying approximately 60% of restorative needs in the practice. Using this benchmark, each full-time hygienist should be generating $30,000 to $40,000 of production per month in treatment completed by the restorative dentist.
RecognizE limitations
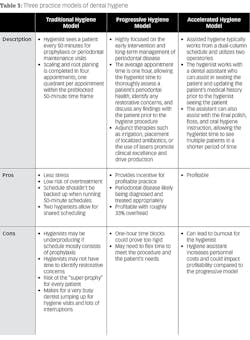
Dental hygiene can be categorized into three models of practice: traditional, progressive, and accelerated. See Table 1.Adjunctive therapies are another service that promotes healthy, happy patients while adding another source of revenue. Research supports the use of lasers to improve healing after SRP.3 Other adjunctive antimicrobial therapies such as Arestin can be placed in the periodontal pocket and have been shown to improve healing over time.4 The cost of goods sold for this treatment can be expensive, and the cost passed on to a patient typically ranges from $500 to $1,000 for 10 to 15 sites. This treatment may be appropriate for a limited number of pockets, whereas laser may be considered for more generalized pocketing.
Promote the principles for a productive hygiene department
There are numerous things owner dentists can do to ensure their hygiene departments are healthy and remain aligned with current industry benchmarks. First and foremost, it’s important to hire hygienists who are the right fit to help maximize patient retention. Active patients typically see their dental hygienist more than once a year. If they like their hygienist, they may be more likely to develop trust in their provider and remain loyal to the practice.
Here are ways to provide effective clinical leadership to dental hygienists to help drive productive restorative schedules:
- Lead and empower hygienists by establishing a consistent clinical culture and incentives.
- Work in collaboration with each dental hygienist to define and align the philosophy of the practice and expectations.
- Ensure that hygienists are trained in the technology available to them in the practice.
- Empower hygienists to identify areas of concern in patients.
- Perfect the hygienist-to-doctor patient handoff.
- Provide consistent coaching and be open to being coached.
A strong dental hygiene program can be highly profitable for the practice and greatly beneficial to patient care and retention. By understanding the typical industry benchmarks and the top principles for a productive hygiene program, owner-dentists can set realistic goals for their practices and implement these goals to realize the benefits of a healthy and profitable hygiene department.
Robert Pirsig wrote, “Working on a motorcycle, working well, caring, is to become part of a process, to achieve an inner peace of mind.”1 Working on our practices and caring for them is no different. We must follow a process to be successful. Try these three steps today and watch the road to success open up before you. Happy riding!
Editor’s note: This article is supported by Pacific Dental Services.
References
1. Pirsig RM. Zen and the Art of Motorcycle Maintenance. New York, NY: 2009.
2. Division of Oral Health, National Center for Chronic Disease Prevention and Health Promotion. CDC website. https://www.cdc.gov/oralhealth/periodontal_disease/. Updated March 10, 2015. Accessed May 18, 2017.
3. Smiley CJ, Tracy SL, Abt E, et al. Systematic review and meta-analysis on the nonsurgical treatment of chronic periodontitis by means of scaling and root planing with or without adjuncts. J Am Dent Assoc. 2015; 146; 508–524.
4. Bonito AJ, Lohr KN, Lux L, et al. Effectiveness of Antimicrobial Adjuncts to Scaling and Root Planing Therapy for Periodontitis Vol. 2. Evidence Tables. Evidence Report/Technology Assessment. NCBI website. https://www.ncbi.nlm.nih.gov/books/NBK11877/. January 2004. Accessed May 18, 2017.
Brad Guyton, DDS, MPH, MBA, serves as vice president of dentist development for Pacific Dental Services and dean of the PDS Institute. He is also an associate professor at University of Colorado School of Dental Medicine and practices dentistry in Denver, Colorado.
Jan LeBeau, RDH, BS, has been in the practice and education of dental hygiene for over 30 years. She currently serves as director of hygiene for Pacific Dental Services and the chair of dental hygiene for the PDS Institute.