A practical look at the subject of fees
Actisite® (tetracycline hydrochloride) Periodontal Fiber Therapy
Today`s dental practitioner must be aware of opportunities presented by new modalities.
Dennis Flanagan, DDS, MAGD
Any discussion of practice productivity you hear today will center almost immediately on a number of disturbing facts and trends facing the profession-facts and trends that will certainly spell trouble for the dentist who insists on practicing dentistry "the way I`ve always practiced." Consider for just a moment that 50% of today`s children under the age of 10 have no decay.1 Add the aging of the U.S. population, increasing pressures for cost containment, plus numerous other pressures, and it`s clear that dentistry of the future will be very different from what we know today. Simply put, technology and demographics are working against practitioners who continue to make operative dentistry the centerpiece of their practices.
Happily, however, this is not the whole picture. Just as technology and demographics have created a crisis in some areas of dentistry, they have also created new modalities for treatment in other areas. In order to remain productive and profitable, today`s dental practitioners must be aware of the opportunities presented by these new modalities and adapt to the changing needs facing the profession.
One such new opportunity is in the treatment of periodontal disease. As virtually all dentists are aware, periodontal disease is more prevalent with age2 and is very widespread. Data indicate that it currently affects almost half of the adult population ages 18 to 64, and up to 86% of adults over the age of 65,3 and it has been estimated that from 90 to 100% of the population will manifest signs of gingivitis at some time during their lifetimes. In addition, periodontal disease tends to be persistent and recurrent, with 17 to 28% of treated periodontal patients developing either refractory or recurrent periodontitis.4
This represents a growth area, where the need for dental services is increasing steadily. Actisite® (tetracycline hydro-chloride) periodontal fiber (manufactured and marketed by the Procter and Gamble/ ALZA Partnership) provides the general dental practitioner a treatment option that offers both a very attractive option to patients and a robust profit center to the typical practice.
Briefly, Actisite® is a tetracycline hydrochloride-impregnated polymer fiber that is indicated as an adjunct to scaling and root planing for the reduction of pocket depth and bleeding on probing in patients with recurrent, site-specific adult periodontitis (and contraindicated in patients with sensitivity to tetracycline). Following scaling and root planing, Actisite® fiber is packed into the pocket, where it is left in place for 10 days, during which the antibiotic is continually released. A six-month clinical trial demonstrated that Actisite® therapy used in conjunction with scaling and root planing provided significantly greater reductions in probing depth and bleeding on probing than scaling and root planing alone.5 And although Actisite® was first made available to general dental practitioners in 1994, case studies from the field reinforce the benefits seen in clinical trials.6-8 Actisite® therapy has relatively few side effects, with the most commonly reported adverse events from the pivotal clinical trials being discomfort on fiber placement (10%) and local erythema following removal (11%). Actisite® should not be used in patients who are hypersensitive to any tetracycline. The safety and effectiveness of Actisite® fiber in children or pregnant women have not been tested. Actisite® fiber should be used in a nursing woman only if clearly needed.
Our practice began using Actisite® in October, 1994, and have found that it is a valuable addition to our more traditional therapies-both for our patients` health and the health of our practice. I see an average of approximately five patients per week who are candidates for this treatment, and have found patients to be very receptive to Actisite® therapy. In addition, Actisite® offers some very practical advantages to the practitioner, including a low start-up investment, short learning curve in using the product, and the uniqueness of the therapy itself that allows us to offer the patient a very attractive treatment.
However, one problem we encountered is that because this is a therapy that is essentially different than traditional treatments, there was little guidance available on how to set our fees. Like most dental practitioners, we were not expert at determining fees that accurately reflect our true costs. Therefore, over the first months we used Actisite®, we were careful to document exactly what went into treatment, and have used those facts to develop formulas that other practitioners can also use to easily calculate an equitable fee that offers the best value possible to the patient and also ensures your practice a profit (Actisite® therapy is currently covered by some insurance carriers, under code number 04381 [localized delivery of chemotherapeutic agents via a controlled release vehicle into the diseased crevicular tissue, per tooth, by report].)
We began with the basic general formula shown in Figure 1. This equation simply reflects the following costs that must be covered in order to ensure the practice a profit:
1. Labor-the salaries and benefits of the practice staff, including dentist, hygienist and assistant.
2. Materials and supplies-the costs of materials and supplies consumed in the treatment.
3. Overhead-the substantial "hidden" costs that reflect what it costs to supply the office and "keep the doors open."
Having reviewed these basics, let`s get to the more difficult matter of how we determined the exact values to plug in to each of these slots in order to calculate a final dollar fee.
Labor Costs
Determining your labor costs requires that you carefully consider the various patient visits that will be involved in the course of Actisite® treatment, which members of the practice staff will be involved at each visit, and for how long. As you do so, you must be careful to isolate the costs of Actisite® treatment itself (for which you will assign a separate fee) from other related therapies.
Overview of Actisite® Treatment Appointments
In order to first see the entire spectrum, let`s quickly review the complete list of patient visits that are related to Actisite® therapy:
- Scaling and root planing.
- Three-week follow-up. After healing from scaling and root planing, the patient will return for follow-up evaluation, and if the pocket(s) remains, the final decision to use Actisite® will be made.
- Actisite® placement. De-pending on office practice and scheduling, placement can be done at the three-week follow-up visit or a separate visit.
- Actisite® removal. Per-formed 10 days after fiber placement.
- Recare visits. Recare appointments at 3- to 4-month intervals are recommended following periodontal treatment.
This article will assume that your fee for Actisite® treatment will cover only the placement and removal appointments, with other related visits charged separately, in accordance with your existing fee structure. This approach allows you more flexibility- and means less work is required to determine an appropriate fee for Actisite® therapy.
How Much Time Is Involved?
One of the most attractive features of Actisite® is that the placement and removal procedures are relatively easy. Placing the fiber is basically the same as packing retraction cord. You may find that at first Actisite® fiber is somewhat more difficult to place in that it is smaller than retraction cord, making it a little harder to handle. It can also tend to spring back, swell slightly and become slippery. Nonetheless, these are not major concerns, and most practitioners should feel fairly comfortable with their placement technique after placing the fiber in a couple of patients. Likewise, removing the fiber generally presents no problems. The only real concern is ensuring that all fiber is removed, which can be accomplished by careful inspection. The manufacturer suggests that the placement time required per tooth will be 5 to 10 minutes, and we have found that this is a very fair estimation in the vast majority of cases. (Placement also involves securing the fiber with the accompanying adhesive, which is included in the 5 to 10 minute time estimate.) In fact, with experience it is possible that your actual placement time could be as low as 3 to 4 minutes per tooth.
Naturally, there will be some variation from case to case. Deeper pockets in harder-to-reach areas may take somewhat more time. And in rare cases, a particularly sensitive patient may require anesthesia, which will also require additional time. On the other hand, we have found that there are a number of things the dentist can do to work most efficiently. For example, we have found that it is cost effective to have an assistant aid the dentist in placing and removing the fiber. Similarly, with experience, the practitioner will realize the most efficient techniques. For example, Actisite® fiber does not need to be packed all the way to the top of the pocket. We have found that within 1 to 2 mm of the gingival crest is generally adequate, and will also help keep the fiber in the pocket over the 10-day treatment period.
How does this translate to actual chair time, factoring in all of the time that staff will actually spend with the patient? Our office uses the following general scheduling guidelines, assuming a standard time unit of 15 minutes per unit. (Note, since Actisite® is indicated for site-specific periodontal disease, for use in isolated sites, the vast majority of procedures will fall into the "1 tooth" or "2-3 teeth" categories.)
1. Placement time:
- 1 tooth-1 unit
- 2-3 teeth-2 units
- 4-5 teeth-3 units
2. Removal time:
- 1 time unit to remove fiber, examine, and record results.
Who Is Involved?
The next step is to consider exactly how you want to handle the placement and removal of the Actisite® fiber, and which of your practice staff will be involved at each step. The biggest variable in this area is who will do the actual fiber placement or removal-dentist or hygienist. This decision is largely out of your hands, as state dental practice acts determine whether hygienists are permitted to place and remove the fiber.
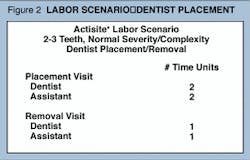
The next step is to construct one or more scenarios in which you anticipate the exact chain of events during the placement and removal appointments. The purpose of this is to detail exactly the amount of staff time that will be involved and allow you to calculate your labor costs as precisely as possible. Figures 2 and 3 present two examples of such scenarios for the placement and removal visits, Figure 2 with the dentist performing the placement/ removal, and Figure 3 reflecting the practice in an office where the hygienist does placement/removal. In Figure 2, the dentist has decided to work with an assistant, so the total labor costs consist of the dentist`s time plus the assistant`s time. In Figure 3, in addition to the hygienist`s time, the dentist performs a brief examination before and after the placement procedure and conducts a more extensive examination at the removal visit. Therefore, for this example, the labor costs consist of the hygienist`s time, plus one unit of the dentist`s time.
Creating a Labor Cost Equation
From such scenarios, construct a simple equation to calculate labor costs. For example, for the scenario in Figure 2, the equation would be:
Labor cost = (3 units x assistant`s rate) + (3 units x dentist`s rate)
And the scenario for Figure 3 would produce the following equation:
Labor cost = (3 units x hygienist`s rate) + (1 unit x dentist`s rate)
To obtain a dollar value, simply translate the units into hours (assuming units of 15 minutes each, one unit equals .25 hour, three units equal .75 hour, etc.), insert the appropriate dollar value for each individual`s rate, and complete the math. In order to ensure that these calculations accurately reflect your costs, be sure that the hourly rates you`re using include the costs of all benefits. If not immediately available, consult your accountant for the inclusive labor rates for members of your staff. If not sure of an appropriate rate to charge for your time (i.e., dentist`s time), you can estimate a rate by taking your yearly before-tax production (or desired pre-tax income), divide by 35 hours per week (average weekly hours spent seeing patients), and divide by the number of weeks per year you see patients.
Materials and Supply Costs
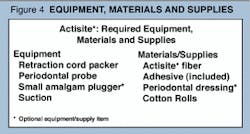
Calculating the material and supply costs required for Actisite® treatment is relatively easy because, as shown in Figure 4, relatively few supplies and no special equipment are needed. Clearly, all needed equipment will be available in any office environment (and its amortized cost will be considered as part of overhead). We also consider cotton rolls a "given," which leaves only the costs of the periodontal dressing (if used) and the Actisite® fiber and adhesive to be considered separately.
Actisite® fiber comes with a supply of adhesive included in the product price. Determining the amount of Actisite® needed can, likewise, be done using a simple formula. Generally, one 23 cm strand of Actisite® will treat one or two teeth, depending on the depth and breadth of the pocket-the deeper and broader a pocket, the more fiber it will accept.
In addition, there are several points to keep in mind. Although a single fiber may be long enough to treat more than one tooth, the fiber cannot be cut and stored for subsequent use on a different patient. Therefore, a minimum materials cost of one Actisite® strand per procedure is a wise starting point. When you are treating multiple teeth in the same patient (at the same visit), however, a single fiber may be cut and used on multiple teeth. So, for example, two strands might adequately treat three teeth.
Because of these variations, you will probably want to develop a set of guidelines for determining average materials cost, instead of pricing each individual procedure separately. For example, our office began by figuring the fiber costs as follows:
- One strand-for treatment of 1-2 teeth with 5-7 mm pockets or 1 tooth with 8 mm pockets at one appointment
- Two strands-for treatment of 3-4 teeth with 5-7 mm pockets or 2 teeth with 8 mm pockets at one appointment
- Three strands-for treatment of 5 teeth with 5-7 mm pockets or 3-4 teeth with 8 mm pockets at one appointment
With experience, we have found determining the number of fibers can be quite accurately estimated by multiplying the number of teeth to be treated at a single appointment by .75 and rounding the result up to the next highest whole number:
# teeth x .75 = Actisite® fibers (round up to next whole number)
Using these guidelines and the materials list from Figure 4, you can construct a materials/ supplies cost equation as follows:
Materials cost = (Price of a single Actisite® fiber x the number of fibers used) + cost of 1 periodontal dressing (optional)
Overhead Costs
The final area of our original equation (Figure 1) is the very important area of overhead. Overhead can be calculated in a number of ways, but in our example (since we`ve considered all labor costs separately), overhead refers to all the costs associated with "keeping your doors open" (including rent, insurance, utilities, general supplies, etc.) and ongoing basic costs that are part of all procedures (infection control, etc.). It is important to remember that these costs are substantial and as such must be a part of any fee. But they are also extremely difficult for most practitioners to calculate with any degree of accuracy.
Your accountant may be able to provide you with a sense of your practice`s overhead as percentage of gross. If not, we recommend using an industry average.
Recent data is quite consistent in indicating average total overhead costs (including salaries and benefits) of 60 - 65%, and overheads not including salaries/benefits of approximately 30 to 45%.9-10 Based on these figures, a reasonable overhead for most practices would thus be 40% of the gross fee.
Assuming overhead as 40% of gross, you can calculate a dollar figure for the overhead for Actisite® therapy as described below. If overhead is 40% of your total fee, then the other elements (labor plus materials/supplies) must make up 60% of the fee. This can be ex-pressed arithmetically in the following equations:
Labor + Materials = 60% (Total Fee)
Overhead = 40% (Total Fee)
Thus, assuming you have already calculated your labor and materials costs (as described earlier), you can determine a total fee as follows.
Assuming that:
Labor + Materials = 60% (Total Fee)
Then:
Fee = Labor + Materials ÷ .6
Once the total fee has been determined, overhead costs can easily be isolated as follows:
Overhead = .40 x Fee
Return on Investment
One final element you may want to consider as part of your fee is what would generally be termed "profit." This is an area that makes many in our profession uncomfortable. Until recently, dentistry was seen more as a professional calling, and less as a "business." While dentists certainly understand that it is essential that their practice "make a profit," it is less common that we consider this element as a distinct part of our fees. However, given today`s environment, you should at least consider the implications of including a specific amount for "profit" as an independent "cost" to be considered when calculating your fees.
The concept behind factoring a "profit" into your fees is that your practice represents a substantial monetary investment. If you had not made this investment, theoretically this money would be available for other investments and would be earning you a return. There-fore, when considering "profit" I think it is more appropriate to think of terms of "return on investment." Again, accurately calculating a fair amount to allot for this is very difficult. The best advice on this can be obtained from your accountant or practice management specialist.
Summing It All Up
Thus far, we`ve concentrated on explaining how you can thoroughly examine the actual costs you will incur in providing Actisite® therapy to your patients. I want to stress how important this process is. Especially with a treatment option like Actisite®, you have no "history" or "industry average" on which to base a fee. Therefore, there is a real danger of inadvertently setting a fee which has you treating patients at a loss. Following the simple techniques ex-plained thus far should minimize the possibility of setting an unrealistic fee.
However, once you`ve done this analysis, you need to transform all your calculations into a form that`s easy to adapt to the day-to-day running of your office. One option, of course, is to create a set of fees that vary depending on many variables-number of teeth, depth of pocket, etc. However, this could become cumbersome. Therefore, in our office we`ve constructed a single, simple calculation that can be used for all our Actisite® patients.
To construct a final simplified fee equation your practice can use on a day-to-day basis, I suggest beginning with the following simplified equation:
Fee = (Price of a single Actisite® fiber x the number of fibers used) + "Set Fees"
Using the techniques previously described, determine "set" costs for labor, supplies other than Actisite®, and overhead by performing the calculations, assuming as many reasonable variables/scenarios as possible. Examine your results, and chose a dollar amount for each element that fairly represents the foreseeable costs involved in the majority of cases. When in doubt, round up slightly.
While it may sound complex, in our experience this determination of our "set costs" was actually quite simple. Remem-ber, Actisite® is indicated as an adjunct to scaling and root planing for site-specific periodontitis and is for use in localized sites. Therefore, the labor variations between the "simplest" and "most complex" scenarios for any single appointment are not great. The only materials cost other than the Actisite® itself is the optional periodontal dressing (a truly set cost). And for a set overhead cost, we simply calculated a "low end" and "high end" total fee, and chose an overhead cost approximately half-way between the two.
This leaves only the number of Actisite® strands to be determined for each individual procedure. To do so, we use the final equation described in the "Materials" section (number of teeth treated times .75, rounding result up to next whole number).
Thus, in actual day-to-day practice, we use the final simplified equation shown in Figure 5. Coming up with a fee to quote to a patient involves only three simple steps: multiplying the number of teeth times .75 (and rounding up), and then multiplying times the product price, and adding the set costs! In over 10 months of using Actisite® we`ve found that this is a simple, quick and most importantly, an accurate way of setting our fees for Actisite® placement.
This Special Feature is presented with the cooperation of Procter and Gamble/Alza.
REFERENCES
1-Oral Health of United States Children: The National Survey of Dental Caries in U.S. School Children: 1986-1987. Epidemiology and Oral Disease Prevention Program, National Institute of Dental Research. Bethesda, Maryland. NIH publication No. 89-2247, September 1989.
2-Page RC. Critical issues in periodontal research. J Dent Res 74(4):1118-1128, April 1995.
3-Oral Health of United States Adults: The national Survey of Oral Health in U.S. Employed Adults and Seniors: 1985-1986. Epidemiology and Oral Disease Preven-tion Program, National Institute of Dental Research. Bethesda, Maryland. NIH Publication NO. 87-28868. August 1987.
4-Maynard JG. "Eras in periodontics" in: Periodontal disease management: a new educational opportunity designed specifically for three distinct dental teams...Chicago: The American Academy of Periodontolo-gy @1994, 3-10.
5-Newman MG, Kornman KS, Doherty FM. A 6-month multi-center evaluation of adjunctive tetracycline fiber therapy used in conjunction with scaling and root planing in maintenance patients: Clinical results. J Periodontol 1994;65:685-691.
6-Corsair AC. Long-term effect of tetracycline fibers on recurrent lesions in periodontal maintenance patients. Periodontal Clinical Investigations 1994;16:8-13.
7-Tonetti MS, Pini-Prato G, Cortellini P. Principles and clinical applications of periodontal controlled drug delivery with tetracycline fibers. International Journal of Periodontics & Restorative Dentistry 1994;14:421-435.
8-Kerry G. Tetracycline-loaded fibers as adjunctive treatment in periodontal disease. JADA 1995;125:1199-1203.
9-Anderson PE. Where do you stand? Practice survey shows median income increases seven percent for second straight year. Dental Economics October 1994:40-52.
10-Focus group shares ways to reduce your overhead. Dental Group News (an independent publication prepared exclusively by the editors of Dental Products Report as a demographic supplement) June 1994:1,3
Dr. Flanagan is co-owner of a two-location, dental group practice in Willimantic and Groton, CT, which employs five dentists, eight hygienists, eight dental assistants, four lab technicians and 10 managerial staff members. He is a graduate of the Georgetown University School of Dentistry. He has served two terms as Chief of Dental Staff at Windham Community Memorial Hospital and is a dental consultant to the Windham School Systems. He has authored several clinical articles, is certified for Branemark, Core Vent and subperosteal implants, and holds two patents for dental devices. Additionally, he is active in community affairs and service work both for his community and the dental profession.